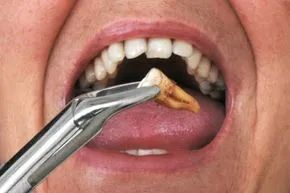
 Cracked teeth are frequently removed to avoid root canal infections.
©iStockphoto.com/choicegraphx
Cracked teeth are frequently removed to avoid root canal infections.
©iStockphoto.com/choicegraphxAlthough teeth whitening ranks as the top cosmetic dental procedure in the U.S., achieving a radiant smile goes beyond bleaching — maintaining excellent oral hygiene is essential for a healthy mouth.
Most of us have experienced a cavity at some point. In fact, 92% of Americans aged 20 to 64 have had at least one cavity in their permanent teeth [source: NIDCR]. This leads to countless dental fillings. Untreated decay, even in small areas, can worsen over time. In cases where damage or decay is too severe for fillings, crowns, root canals, or other treatments, extraction becomes necessary. Extracting a tooth means permanently removing it from the mouth. Infected teeth are also candidates for removal, as antibiotics can't reach the infected nerve inside the tooth. Removing the tooth eliminates decay and infection, preventing it from spreading to other parts of the mouth or body.
Loose teeth or those lacking supportive bone and soft tissue are often extracted, as are impacted wisdom teeth. Wisdom teeth, or third molars, can become impacted when there's insufficient space, causing them to get stuck in the jaw and fail to emerge. Partial eruption due to overcrowding is also common. If not removed, impacted wisdom teeth can lead to pain, swelling, and other issues.
Tooth extractions can also be elective, often to prepare for other dental or orthodontic treatments like braces. Cancer and organ-transplant patients, who face higher infection risks, may need teeth removed before or after treatment if those teeth could cause or develop infections during treatment or recovery.
Sometimes, extractions are necessary due to individual anatomy. Some people simply have more teeth than their mouth can accommodate, and removing teeth helps alleviate crowding.
While you now understand the reasons for tooth removal, did you know there are different types of extractions? Let’s explore the process in detail, from preparation to the actual procedure.
Tooth Extraction Procedure
Before diving into tooth extraction, let’s cover some basics about our teeth. The crown is the visible part above the gum line, while the root lies hidden beneath it. Roots are anchored in a jawbone socket, supported by connective tissues that hold the tooth securely in place.
Prior to the procedure, your dentist will conduct an oral examination and take X-rays of the tooth (or teeth) slated for removal, as well as the surrounding area, to assess the situation below the gum line.
Once preparation is complete, the extraction begins. There are two main types of tooth extraction: simple and surgical.
A simple extraction is performed when the tooth is visible in the mouth. If the tooth is not visible because it hasn’t erupted, is impacted, or has broken at or below the gum line, a surgical extraction is required. Over 10 million teeth are surgically removed annually in the U.S. [source: Boyd].
Let’s start by discussing simple extractions.
Simple extractions are typically handled by your dentist under local anesthesia. During this procedure, an elevator and forceps are used to remove the tooth. The elevator is a specialized tool that detaches the tooth’s root from its socket, loosening it, while the forceps grip the crown to extract it. Stitches may or may not be needed to close the extraction site.
Surgical extractions are more complex, as they involve removing a tooth from the bone. These are usually performed by oral and maxillofacial surgeons, with local or general anesthesia administered based on the case. Unlike simple extractions, surgical procedures require cutting the gum to access the tooth below the gum line. The tooth is then removed, sometimes in pieces, and the wound is stitched closed.
Right after a tooth is extracted, your dentist will place gauze over the wound and ask you to bite down -- this pressure aids in forming a blood clot in the socket, which is crucial for proper healing.
Dental implants are increasingly preferred over other dental prosthetics like crowns, bridges, and dentures. They provide a permanent solution for missing teeth, using titanium roots that integrate with regrown bone and connective tissue.
Tooth Extraction Healing
In the first 24 hours post-extraction, patients may experience some bleeding, which can persist for a few hours. Swelling and mild to moderate pain are also common. The intensity of pain depends on factors like the number of teeth removed, the type and location of the extraction, the presence of infection, and the patient’s pain tolerance.
If pain intensifies instead of subsiding after two to three days, it could indicate a complication called dry socket.
Following a tooth extraction, a blood clot forms in the empty socket. It’s crucial to avoid rinsing, spitting, or sucking (including smoking) to prevent disrupting or dislodging the clot. If the clot is damaged, it exposes the underlying nerves and bone to air, saliva, and food debris, leading to severe pain. Dry socket, though rare (affecting only 2 to 5 percent of patients), is treated with antibiotics and wound cleaning [source: Mayo Clinic].
Curious about when the extraction site will heal? Without complications, new gum tissue typically closes the hole within one to two weeks, with full healing of soft tissues and bone continuing over the next month.
Most patients recover from an uncomplicated extraction in a few days, but complete healing takes several weeks. Proper aftercare is essential for a smooth recovery. Let’s explore the care needed from the first 24 hours post-surgery until the stitches are removed.
Tooth Extraction Aftercare
If you're curious about aftercare, pain management is likely your first concern. In the initial 24 hours post-extraction, most patients rely on painkillers, either prescribed by their dentist or over-the-counter options like ibuprofen. Using a cold compress on the face or jaw can help reduce swelling and alleviate pain by constricting blood vessels.
What about meals? While you don’t need to fast after a tooth extraction, stick to liquids until the numbness wears off to avoid disturbing the wound. Once sensation returns, opt for soft foods like pudding, oatmeal, or mashed potatoes for the first few days. Gradually reintroduce solid foods as healing progresses, unless your dentist advises otherwise.
After the first 24 hours, most patients continue using pain relievers, though prescription medications are usually unnecessary after three days. Over-the-counter anti-inflammatories like ibuprofen can manage pain and swelling for several days post-extraction.
Rinsing gently with warm salt water can help reduce pain and swelling, but wait until after the first 24 hours to avoid disrupting the blood clot. Brush and floss your teeth carefully, avoiding the extraction site and any stitches. Some stitches dissolve on their own, while others require removal during a follow-up visit.
Lying flat or engaging in physical activity can extend bleeding, so take it easy -- consider reclining or using pillows to support yourself while you recover.
