According to Charles Darwin’s theory of evolution, organisms adapt and acquire beneficial traits to secure their survival. Pathogens such as viruses and bacteria exemplify this by mutating and evolving to withstand medications, vaccines, treatments, and our body’s defenses.
While their survival efforts conflict with our well-being, from their perspective, it’s merely about existence—no malice intended. In their position, we would likely act similarly.
10. HIV
HIV is categorized into two main types: HIV-1 and HIV-2. HIV-1, the more prevalent type, is divided into four groups: M, N, O, and P. Among these, Group M is the most widespread and is further split into subtypes A, B, C, D, F, G, H, J, and K. These subtypes are genetically distinct and can combine to form new hybrids known as circulating recombinant forms (CRFs). To date, 89 such CRFs have been identified.
This implies that individuals already infected with HIV remain vulnerable to reinfection, whether at the type, group, or subtype level. Reinfection can lead to the merging of two HIV strains, creating a new strain that may develop resistance to drugs. This phenomenon is referred to as dual infection, though terms like coinfection or superinfection may also be used depending on the transmission method. All these terms essentially convey the same meaning.
To make matters worse, these hybrid CRFs can further combine with other HIV strains, producing even more dangerous hybrids. One such CRF, known as CRF19, is particularly widespread in Cuba. It originated from the fusion of HIV-1 Group M subtypes A, D, and G. CRF19 accelerates the progression to AIDS within three years, compared to the usual 10–15 years.
9. Guinea Worm

Since 1986, former US President Jimmy Carter has dedicated himself to eradicating guinea worm, a debilitating condition that culminates in a worm over 1 meter (3.3 ft) long painfully exiting the body over the course of a month. In 2016, only 11 cases were reported, a significant drop from the million cases recorded in 1986 when Carter launched his campaign.
If Carter succeeds, guinea worm will become the second disease eradicated by humans (after smallpox) and the first to be eliminated without the use of vaccines. However, guinea worms are resisting eradication fiercely.
How? They’re adapting by infecting new hosts: dogs.
In Chad, one of the last nations still fighting guinea worm, infections in dogs have been reported since 2012. Approximately 600 dogs were confirmed infected in 2016, though the actual number is likely higher. Monitoring these dogs is challenging due to their free-roaming nature, which also makes it hard to prevent them from accessing water, a critical element for guinea worm reproduction.
Adult guinea worms cause a burning sensation in infected individuals, driving them to seek water to alleviate the pain. The worm then releases its larvae into the water. These larvae are ingested by small aquatic creatures, which are later consumed by humans drinking the contaminated water.
These larvae mature into adult worms inside the human body, perpetuating the cycle. The exact method by which dogs contract guinea worms remains unclear, though contaminated fish is a suspected source.
8. Bubonic Plague
The Black Death, a devastating pandemic that swept through Europe in the 14th century, claimed approximately 25 million lives, wiping out up to one-third of Europe’s population. It was caused by the Yersinia pestis bacterium, which spreads from infected rodents to humans via fleas. This bacterium can cause bubonic, pneumonic, or septicemic plague in humans.
Despite its terrifying history, Yersinia pestis remains active today. It is currently found in 25 countries, including Madagascar, which experienced a minor outbreak from August 1 to November 22, 2017.
The more alarming aspect of the plague is its growing resistance to drugs. By 2017, at least 10 commonly used antibiotics had lost their effectiveness against the disease. This resistance is thought to result from gene exchange between Yersinia pestis and other bacteria such as E. coli, Klebsiella, and Salmonella, all of which are present in food.
7. Polio
Polio was once a leading cause of death among young children, often leaving survivors with permanent paralysis. However, vaccination efforts have significantly reduced its impact. Typically, children receive oral doses of a weakened polio virus, enabling their immune systems to develop resistance to the stronger, natural strain.
Recently, it has been observed that this weakened polio virus, excreted by children, can regain strength, mutate, and infect others. This mutated form is more dangerous than the natural virus and, unfortunately, is resistant to existing vaccines.
Consequently, children who have been vaccinated against polio remain vulnerable to this new, mutated strain, which originates from the very vaccine designed to protect them. In one outbreak in the Democratic Republic of Congo, 47 percent of the 445 infected children died, despite having received the vaccine.
6. Ebola

Many first learned about Ebola during the 2014–2016 outbreak in West Africa. This period, spanning March 23, 2014, to January 13, 2016, marked Ebola’s deadliest outbreak, claiming at least 11,315 lives—five times more than all previous epidemics since its discovery in 1976. This number is likely an underestimate, with the actual toll believed to be much higher.
The 2014 Ebola outbreak began in December 2013 with the death of a two-year-old child in Guinea. By March 2014, it had reached Liberia and soon spread to Sierra Leone and neighboring nations. During this time, it infected over 28,000 people, a figure 100 times greater than in earlier Ebola epidemics.
Two separate teams of virologists studying the epidemic concluded that its increased lethality was due to a mutated strain of the original Ebola virus. This mutant, named A82V, was responsible for over 90 percent of all infections during the outbreak.
Researchers suggest that the A82V mutant was eradicated alongside the epidemic because it struggled to infect nonhuman hosts, such as fruit bats, which are thought to transmit Ebola to humans.
5. Gonorrhea
Data from 77 countries reveals that gonorrhea is increasingly resistant to all available drugs. Azithromycin, the primary treatment, now fails in 81 percent of cases. Other drugs, such as extended-spectrum cephalosporins (ESCs), including oral cefixime and injectable ceftriaxone, fail 66 percent of the time.
The United Kingdom is grappling with an outbreak of drug-resistant gonorrhea. This strain, dubbed “super gonorrhea,” is completely resistant to azithromycin and may soon develop resistance to ceftriaxone as well. Investigations by the BBC suggest that the resistance to azithromycin arose because patients were taking it alone instead of combining it with ceftriaxone, as recommended by UK healthcare guidelines.
4. Cholera

Cholera is triggered by ingesting food or water contaminated with the Vibrio cholerae bacterium. While it often results in mild diarrhea, some infected individuals may not even realize they have it. In severe cases, it leads to extreme dehydration, vomiting, and diarrhea, which can be fatal within hours.
Haiti experienced a devastating cholera outbreak 10 months after the catastrophic January 2010 earthquake. The epidemic claimed 9,200 lives, though organizations like Doctors Without Borders argue the actual number is much higher, as many cholera-related deaths went unrecorded. In some areas, only 10 percent of deaths were reported.
The cholera outbreak in Haiti was caused by a mutated strain known as “altered El Tor.” This strain is more lethal than typical cholera and has been compared to the deadly cholera outbreaks of the 1800s. Altered El Tor underwent three mutations that enabled it to evade the body’s initial warning system. First identified in 2000, it has been linked to Nepal.
3. Cancer

Cancer has been recognized for its ability to evolve and mutate since the 1970s. These mutations enable cancer to resist drugs, expel medications from the body, and repair cells damaged by treatment. Researchers attribute this behavior to cancer cells that survive initial therapies.
Prostate cancer is one type known to mutate. It relies on testosterone for growth, and treatment often involves depriving the body of this hormone. However, prostate cancer cells have adapted by using alternative molecules in place of testosterone, leading to castrate-resistant prostate cancer, which is frequently fatal.
Lung and colorectal cancers also possess the ability to mutate. Their cells develop resistance to radiation and chemotherapy, rendering them untreatable.
One potential solution for treating these mutant cancers is “individual-specific therapy,” a personalized treatment approach. However, this method is not without its limitations.
Herceptin, one of the first drugs developed for “individual-specific therapy,” targets the HER2 protein to eliminate breast cancer cells. However, the cancer adapted by destroying the HER2 protein regions where Herceptin binds. Often, the body responds by producing HER3 cells, complicating treatment since Herceptin cannot bind to HER3.
2. Tuberculosis

Tuberculosis is undergoing significant mutations, leading to two new forms: multidrug-resistant tuberculosis (MDR-TB) and extensively drug-resistant tuberculosis (XDR-TB).
MDR-TB resists isoniazid and rifampicin, the two most effective drugs for treating tuberculosis. XDR-TB, a more severe form of MDR-TB, is resistant to isoniazid, rifampicin, and multiple other medications.
In 2015, approximately 580,000 cases of MDR-TB were reported, with 55,100 (9.5 percent) being XDR-TB cases. XDR-TB has been identified in 117 countries, indicating its emergence as a global issue.
It is believed that tuberculosis developed drug resistance due to improper storage or administration of medications. Tuberculosis treatment requires a strict six-month regimen without interruption. Any disruption can lead to drug resistance.
1. Syphilis
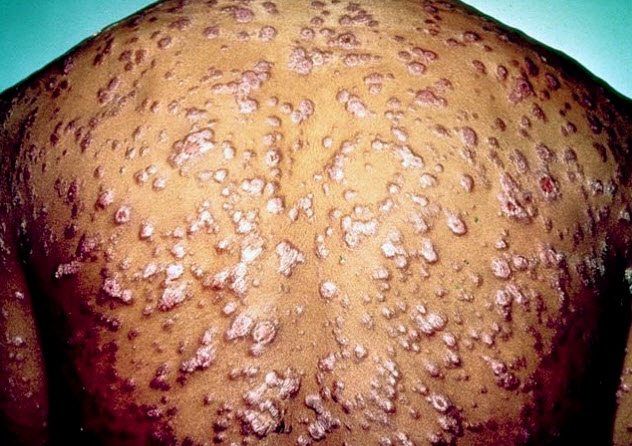
Syphilis is often referred to as the “great imitator” because its symptoms closely mimic those of other illnesses. It is primarily transmitted through sexual contact but can also pass from mother to child during pregnancy.
Researchers have found that Nichols and Street Strain 14 (SS14), the two primary strains of syphilis, are undergoing mutations. These changes are making them resistant to standard antibiotics like penicillin and macrolides, which are commonly used for treatment.
The mutation is more common in SS14. In one study, approximately 90 percent of SS14 samples showed drug resistance, compared to 25 percent for the Nichols strain. This growing resistance is contributing to the resurgence of syphilis.
Since 2013, syphilis cases have risen by 15 percent. While most antibiotics remain effective for now, the disease could develop resistance to these treatments over time.
