The human brain, with an average weight of 1.36 kilograms, is an extraordinary organ. Though it might first appear as a disorganized sponge, it holds more than 100 million neurons and 100 trillion synaptic connections. It remains the most complex known structure in the universe. Given its intricate nature, it's unsurprising that the brain can face significant challenges. This article highlights 10 individuals who have encountered such challenges—when parts of their brains malfunctioned in unusual ways. By the end, you'll likely develop a deeper appreciation for your own brain and understand the importance of keeping it healthy and protected.
10. Peter The Split-Brain Patient Struggling with Inner Conflicts
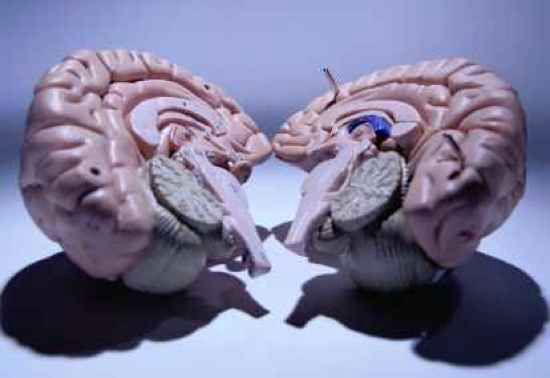
Area of Damage: Corpus Callosum
Peter's battle with complex partial seizures began at the age of 8. Despite taking antiepileptic medications, his seizures were severe, leading to a difficult journey. By the time he turned 20, after enduring over 12 years of this condition, Peter and his doctors made the decision to perform a commissurotomy.
The commissurotomy procedure involved surgically cutting Peter’s corpus callosum, the main nerve tract that connects the brain’s right and left hemispheres. This crucial structure is responsible for allowing communication between the two sides of the brain, so damaging or removing it results in a breakdown of interhemispheric communication.
Peter’s surgery achieved partial success in reducing the severity of his seizures, but it also left him drastically changed. For instance, he could no longer respond with his left side to verbal commands. If told to “Stand like a Boxer,” his left side would droop and lack movement, while his right side would respond as expected. With his brain essentially divided, his left and right sides often acted like two separate individuals. Peter reported that his left hand would unintentionally turn off the TV while he was watching, his left leg would sometimes move in the wrong direction, and his left arm would occasionally battle his right side. Peter’s case highlights the importance of the brain functioning as a unified whole rather than separate parts.
9. D.B. The Man Who Was Struck by Confusion Due to His Own Blindsight

Area of Damage: Primary Visual Cortex (Occipital Lobe)
In our everyday experience, perceiving and being consciously aware of something are thought to be two sides of the same coin; they are inseparable. We naturally assume that anyone who sees something will also be able to recognize and describe it. This ability to consciously see and perceive is so common that we take it for granted. The case of D.B. provides a striking example of how this assumption can be challenged.
D.B. suffers from a neurological condition known as blindsight, which causes an individual to be unable to consciously perceive objects they can still see. While D.B.’s vision is excellent—better than most people's—his brain suffers from damage to his primary visual cortex, located in the occipital lobe. As a result of this damage, D.B. has lost awareness of what he ‘sees’ in his left visual field, but he has demonstrated some surprising abilities: (a) he can accurately reach for visual stimuli in that field; (b) he can distinguish between vertical and diagonal or horizontal lines; (c) he can tell the difference between the letters “X” and “O” when they appear in his blind visual field.
His doctors repeatedly questioned him about the vision in his left visual field, only for him to insist that he saw nothing. However, when shown the results (through his functional right visual field), D.B. expressed amazement and claimed that he had been “guessing.” He was astonished to see video footage of himself accurately reaching and identifying the orientation of lines. Though he couldn’t consciously register what he was seeing in his ‘blind’ field, he still had the ability to respond to visual stimuli, which is why his condition is referred to as ‘blindsight’.
8. R.P. A Classic Case of Prosopagnosia

Area of Damage: Fusiform Face Area
We depend heavily on our ability to recognize others by their faces. Imagine if everyone you knew wore a paper bag over their head to hide their identity—strange, right? This is the reality R.P. faces every day. R.P. suffers from prosopagnosia, a condition where one cannot recognize faces. Prosopagnosia is one of many types of visual agnosia (agnosia refers to a failure of recognition), which also includes movement agnosia, object agnosia, and color agnosia.
While R.P. can often tell that something is a face, she struggles to identify whose face it is. She reports no other recognition difficulties, and like D.B. from the previous case, her vision is exceptional. Those with prosopagnosia typically perceive a fragmented view of facial features, unable to recognize a face as a cohesive whole. In extreme cases, individuals may not even recognize their own face. Prosopagnosia is linked to damage in the fusiform face area, located at the junction of the occipital and temporal lobes of the brain.
7. N.I. The Woman Who Read with Her Right Hemisphere
Area of Damage: Complete Removal of Left Hemisphere
Before falling ill, N.I. was an entirely normal young girl. However, at the age of 13, she began experiencing seizures and a rapid decline in her speech and motor abilities. CT scans revealed ischemic damage (lack of blood flow) to her left hemisphere. Even two years after the onset of her illness, N.I. continued to suffer, and her right side became paralyzed. To alleviate her symptoms, doctors decided to perform a total left hemispherectomy (removal of her left brain hemisphere). Following the procedure, her seizures completely stopped. Unfortunately, the surgery resulted in her losing the ability to read properly, as most people, including N.I., rely on the left hemisphere for language tasks.
After the surgery, N.I. was able to recognize individual letters, but was unable to convert them into sounds. She could read simple, familiar words (like 'fan'), but struggled to pronounce even simple made-up words (like 'neg'). Her reading mistakes suggested that she relied on the meaning and visual appearance of words, rather than converting the letters into sounds. For instance, when shown the word “fruit,” she would say “juice.” This pattern of errors is similar to a condition known as 'deep dyslexia,' in which individuals struggle to apply pronunciation rules when reading. People with deep dyslexia can still read familiar words based on memory, but like N.I., they can't pronounce unfamiliar or nonsensical words.
6. W.M. The Man Who Reduced His Blind Spot With His Hand

Area of Damage: Right Occipital and Parietal Lobes
W.M. suffered a stroke in the right posterior cerebral artery, leading to significant damage to his right occipital and temporal lobes. As a result, he developed severe left hemianopsia, a condition where half of his visual field was obstructed by a blind spot. Essentially, W.M. was nearly blind in his left visual field. During tests, with his left hand resting on his lap, W.M. was able to detect 97.8% of stimuli in his right visual field but only 13.6% in the left.
What makes W.M.’s case intriguing is that when his left hand was extended into his left visual field, his ability to detect stimuli greatly improved. His brain allowed him to detect objects near his left hand, even when the hand was in the scotoma (the blind spot). Remarkably, this effect was enhanced when W.M. held a tennis racket in his extended left hand. His case demonstrates the brain’s remarkable adaptability, as it found ways to compensate for the damage and adapt to its limitations.
5. Miss C. The Woman Impervious To Pain

Damage Location: Unknown (most likely the result of a genetic disorder that interferes with the production of sodium ion channels in the anterior cingulate cortex of the brain)
Pain perception is paradoxical—it is both something hard to endure and something hard to live without. It’s fascinating how an experience that seems entirely negative is actually vital for our survival. Pain serves as a protective mechanism, warning us to stop engaging in harmful actions. The significance of pain is most evident in cases where individuals experience no pain at all, such as the case of Miss C.
Miss C. was an exceptionally bright young woman, with no health concerns aside from one striking issue: she had never felt pain, not even a hint of it. As a child, she accidentally bit off the tip of her tongue while eating. Her body bore signs of third-degree burns, a result of unknowingly kneeling on a hot radiator. She never felt the electric shock coursing through her body, nor did she feel pain from extremely hot or cold water. Remarkably, her body showed no signs of physiological changes, such as alterations in blood pressure, heart rate, or respiration, when subjected to these extreme conditions.
When questioned, Miss C. couldn’t recall the last time she coughed or sneezed. Her gag reflex was nearly impossible to trigger, and she lacked corneal reflexes (the automatic blinking response). She didn’t shift her weight while standing or turn over while sleeping—actions typically needed to prevent joint inflammation. Tragically, Miss C. passed away at 29 due to complications arising from infections, as well as skin and bone trauma, all of which could have been prevented had she been able to feel pain.
4. Mrs. S The Woman Who Turned Round And Round

Location of Damage: Right Posterior Parietal Cortex
After suffering a stroke, Mrs. S. lost the ability to recognize or react to anything on her left side, including both external objects and parts of her own body. For instance, she would often apply makeup to the right side of her face, but leave the left side untouched. Mrs. S. was affected by contralateral neglect, a condition where a person fails to respond to stimuli on the side of the body opposite the brain injury. Since her stroke had impaired the right posterior parietal lobe, she struggled with left-sided neglect.
This condition led to various difficulties in her daily life. One of the most challenging issues was her inability to eat enough. When a plate of food was placed in front of her, she could only perceive and consume the food on the right side of the plate, even though she was still very hungry. To solve this, Mrs. S. developed a unique strategy to ensure she got more food. While sitting in her wheelchair, she would spin it around in a full circle to the right, stopping when the untouched portion of her meal appeared. She would then eat it and repeat the process until either the plate was empty or she felt satisfied.
3. H.M. The Man Frozen In Time

Location of Damage: Removal of Both Medial Temporal Lobes (Loss of hippocampus, amygdala, and perirhinal cortex)
H.M. (Henry Molaison) is arguably one of the most famous cases in the study of memory, despite the sorrow surrounding his condition. His story has played a crucial role in advancing scientific understanding of human memory. If you are unfamiliar with it, here is a summary of his experience:
H.M. had been suffering from debilitating epilepsy for eleven years prior to his surgery. He endured an average of one generalized seizure per week and numerous partial seizures each day, even while taking anticonvulsant medication. Electroencephalogram (EEG) results revealed that his seizures originated from the medial (inner) regions of his left and right temporal lobes. In an attempt to stop the seizures, doctors decided to remove both of these lobes in a procedure known as a bilateral medial temporal lobectomy.
The surgery was effective in reducing H.M.'s seizures, completely eliminating the generalized ones and significantly reducing the partial seizures to only one or two per day. However, it was also the last time the procedure was performed, as it caused severe amnesic effects. Following the surgery, H.M. developed profound anterograde amnesia. This type of amnesia prevents the ability to remember events that occur after brain damage, unlike retrograde amnesia, which affects memory for events that happened before the injury.
Interestingly, H.M.'s general intelligence remained unaffected by the surgery, as he scored above average on standardized intelligence tests. His memory for events that occurred before the operation was also largely intact. Furthermore, his short-term memory for recent events remained normal (for example, he could easily repeat a sequence of six digits). However, H.M. was unable to form new long-term memories. Once he stopped thinking about an event, it would fade from his memory permanently. He could not recognize people he met after the surgery and would need to be reintroduced each time as though they were strangers. H.M. spent much of his days doing crossword puzzles in the nursing home, but because he always wrote down his progress, he could continue working on them. For the rest of his life, H.M. was trapped in the present, a prisoner of his own mind.
2. K.C. The Man Who Cannot Time Travel

Location of Damage: Diffuse damage; mainly the medial temporal lobes
K.C. was involved in a motorcycle accident in 1981, which resulted in diffuse brain damage and severe amnesia. Despite the impairment to his memory, K.C.'s other cognitive functions remained largely intact. He had no trouble concentrating, and enjoyed activities such as playing chess, the organ, and card games. His reasoning skills were good, and his knowledge in areas like mathematics, science, history, geography, and other school subjects was preserved. He was able to retain many facts from his early life, such as his birthdate, childhood address, and the names of his schools. A notable feature of his intact memories is that they are all factual in nature, known as semantic memories.
Although K.C.'s semantic memory remains intact, he suffers from severe amnesia when it comes to personal experiences. He cannot recall a single event from his personal life for more than a minute. This extends to all events he has ever experienced. Despite these memory issues, K.C. can hold a conversation without difficulty, and his memory problems are not as apparent as one might expect. He effectively uses his semantic memory in conversations. For instance, when asked about his brother's funeral, he would answer, 'Sad, very sad.' However, K.C. could not remember having a brother, or whether he was still alive. He used his semantic memory, knowing funerals are typically sad events, to respond accordingly. While K.C. understands the concept of time, he cannot mentally 'time travel' to the past or future. He cannot recall his past any more clearly than he can envision his future. In essence, he is unable to imagine what he will be doing for the rest of the day, week, or the rest of his life.
1. Jimmie G. The Man Who Thought He Was Younger

Location of Damage: Medial Diencephalon (Medial Thalamus and Medial Hypothalamus)
The last three entries in this list will focus on arguably the most infamous of psychopathological conditions, namely, amnesia (a disruption of memory). We begin by exploring the unfortunate case of Jimmie G.
Jimmie G. was a lively 49-year-old man who loved talking about his school days and his time in the navy. He was an intelligent individual, with exceptional skills in mathematics and science. Given this description, it would be hard for anyone to imagine that he was a patient in a neurological ward. His issues were apparent when one paid close attention to how he described his past. When recalling his school experiences, he used past tense, but when discussing his navy days, he switched to the present tense. Even more puzzling was the fact that he never mentioned anything that had happened to him after his time in the navy.
Jimmie G. believed he was still a 19-year-old man, continuing his service in the military. When shown his reflection, he would become confused and upset. If someone were to leave and return a few minutes later, Jimmie would greet them as though they had never met. When asked where he thought he was, he would respond that it looked like a hospital, and he feared he had been admitted because he was ill, though he couldn’t remember why.
Further testing revealed that Jimmie was suffering from Korsakoff’s syndrome, a condition often seen in individuals who have consumed large amounts of alcohol. (Indeed, Jimmie had been an alcoholic in his younger years). His memory impairment was due to brain damage caused by a deficiency in thiamine (vitamin B1), commonly seen in chronic alcoholics. In its more advanced stages, as in Jimmie G.’s case, Korsakoff’s syndrome results in severe memory loss.
