They usher us into life, manage our health, and don their prestigious white coats. While doctors lead the charge in medical research, they occasionally become the focus themselves. Recently, studies have revealed that doctors' DNA can undergo alarming changes, and that pharmaceutical sales representatives have an outsized influence on their decisions. Even the operating room can be unsettling, with incidents like fires igniting on patients while others joke through brain surgeries.
10. Nurses Keep Their Hands Cleaner

Each year, hospitals become breeding grounds for infections. Ironically, it’s the very hands of the medical staff that spread harmful germs between wards. This threat to lives led New South Wales to launch a year-long campaign aimed at educating public hospital workers. Once the campaign wrapped up in 2007, the University of New South Wales (UNSW) and the NSW Clinical Excellence Commission wondered if any meaningful change had occurred.
The researchers conducted four studies to track how often staff washed their hands after visiting patients. Although there were some improvements, the numbers remained worryingly low. Doctors' hygiene habits improved from 26% to 38%, while nurses went from 54% to 65%. Interestingly, allied health workers surpassed doctors, rising from 40% to 48%.
9. Incas Surpassed Civil War Surgeons in Skill

Brain surgery dates back thousands of years, with the Inca civilization particularly excelling in trepanation—removing sections of the skull from living patients. A study in 2018 analyzed 800 Incan skulls, revealing that this practice evolved from rudimentary methods to highly refined techniques over time. By 1500 A.D., up to 83% of Inca skulls showed signs of healing. More strikingly, their survival rate outpaced that of soldiers undergoing head surgery during the American Civil War, nearly half of whom perished.
Although experts remain uncertain about the reasons behind the Inca's brain surgeries, it is unlikely that their methods resembled the chaotic, understaffed conditions of the Civil War's field hospitals, which contributed to its staggering death toll. Inca healers, however, understood the importance of infection control and addressed it effectively—something Civil War doctors failed to do. During the war, surgical instruments and hands were rarely sterilized before removing shrapnel from wounded soldiers.
8. Pharmaceutical Marketing Influences Prescriptions
The ethics of pharmaceutical marketing have long been a controversial issue. When does marketing cross the line from providing valuable solutions to doctors and patients to prioritizing sales and profit over medical integrity? In 2010, a research team from nine institutions conducted an in-depth review of the available literature on this topic, which helped shed light on the extent of the problem.
Pharmaceutical promotions have a negative impact. Doctors who accept these promotions tend to prescribe more medication, often with lower quality compared to their peers who do not. The review suggested that medical professionals avoid these sales tactics and instead consult independent sources. Given the immense revenue generated by drug promotions, pharmaceutical companies are unlikely to support the review’s recommendation that an external organization should manage their financial and promotional activities.
7. Doctors Aren't as Brilliant as You Might Believe

Becoming a doctor is a long and challenging journey, and most people associate this path with exceptional intelligence. The road to MD status begins with a competitive pre-med college track, followed by success on the MCAT, medical school, board exams, and a 3-7 year residency before achieving board certification and becoming an attending physician. While this may seem daunting, intelligence alone isn't enough to succeed—it’s more about perseverance and determination.
Medical school is often compared to drinking from a fire hydrant. The material isn't inherently difficult, but the sheer volume and speed of learning is overwhelming. Success in this environment is less about raw intelligence and more about having the right work ethic. Students must dedicate themselves to relentless repetition and active learning, often using tools like Anki cards to reinforce their knowledge.
In certain highly competitive specialties, success often depends more on test-taking skills, research productivity, and rapport with mentors rather than raw intelligence. Remember, the student who graduates last in medical school is still referred to as 'Doctor!'
6. Doctors Can Be Unkind

In 2012, Dr. Lucian Leape published research that resonated with many patients. He observed that too many of his colleagues were unkind, and that patients often dreaded visiting the hospital not just because of their illness, but because of negative past experiences with doctors who belittled them. Leape’s findings highlighted the troubling range of unprofessional behavior, from explosive emotional outbursts and bullying of staff to apathy or burnout. The most common issue was the dismissive treatment of patients, where they were ignored or treated poorly.
Leape discovered that many people leave the emergency room feeling treated like nothing more than a file or a problem to be dealt with, rather than as human beings. He suggested that medical school instills a sense of entitlement in doctors due to their special role in society. While this might be true, both Leape and many patients feel that some doctors let this elevated status go to their heads.
5. The Controversial Dutch Euthanasia Case

Since 2002, the Netherlands has permitted doctors to perform euthanasia when a patient’s suffering becomes unbearable and they provide irrefutable consent. Recently, a Dutch physician faced criminal charges for performing the first euthanasia case to go to trial. The prosecution argued that the patient, a 74-year-old woman with severe Alzheimer's, was incapable of giving proper consent. However, four years prior, the woman had written a statement expressing her wish to be euthanized rather than live in a care facility.
The time arrived when the physician made the call. Two other doctors reviewed the case and concurred. A date was chosen, and the doctor, the patient, her husband, and daughter gathered for coffee. The 74-year-old woman’s beverage was mixed with a sedative, but it didn’t have the desired effect. Another dose was administered via injection. She dozed off, but just as the doctor was about to deliver the second and lethal dose, the woman stirred and stood up. Her family held her down, and the drug was given. The court ultimately cleared the doctor, ruling that the patient’s severely diminished mental state made it impossible for her to confirm her death wish that day, while her written declaration was considered valid.
4. Laughter During Brain Surgery

Certain brain surgeries require the patient to remain awake. This helps doctors monitor the functioning of critical areas, such as those involved with language. Understandably, some patients panic upon realizing they are conscious during the procedure—especially with their head locked in place, part of their skull removed, and their brain exposed. Some patients have been known to try to remove their brain or struggle with the restraints.
In 2018, a patient with epilepsy underwent this procedure. Normally, sedation and other methods keep patients calm, but this time, the doctors chose a more playful approach. It didn’t start well. When the woman woke up, she was so distressed that she began crying. Something had to be done before she became too agitated. The solution was to make her laugh. Rather than relying on humor, the doctors stimulated a set of brain cells called the cingulum bundle, which was thought to control the muscles used for laughter, though it wasn’t linked to emotions. Contrary to expectations, the woman laughed throughout the procedure, proving that the brain's response to laughter was more complex than previously thought.
3. Their DNA Reveals Faster Aging

In 2019, DNA samples were collected from 250 doctors at the start of their internship, followed by a second test at the conclusion of their first year of work. The results were alarming. The DNA of these new doctors showed significant signs of aging within just 12 months on the job. In comparison, other individuals typically required six years for their DNA to undergo the same level of deterioration.
The scientists made an unexpected discovery when examining telomeres, the protective caps at the ends of chromosomes. While telomeres naturally shorten as we age, it appeared that the stress from work accelerated the process in these interns. Doctors who worked the longest hours or had neurotic traits, as well as those dealing with stressful family situations, showed the most significant signs of accelerated aging. Why does this matter? The shrinking of telomeres is concerning as it increases the risks of cancer, heart disease, and cognitive decline. The researchers hope that their findings will lead to reforms in the grueling hours that doctors face during their training and careers.
2. Fires During Surgery
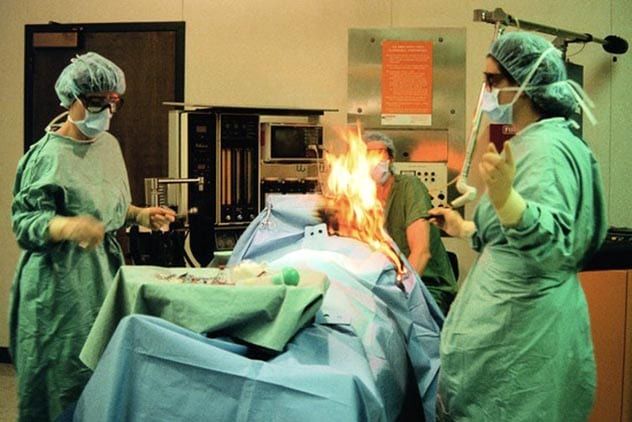
In 2019, an Australian patient underwent an emergency surgery intended to repair a tear in his aorta, but it unexpectedly resulted in a fire near his chest cavity. The heart surgery started without issue, but complications arose due to the patient’s health. The man had an enlarged lung, and when doctors accidentally punctured it, they had to address the resulting air leak. To compensate, they increased the oxygen levels in the anesthetic.
As the patient inhaled the anesthetic, both the oxygen and sevoflurane sedative escaped through the punctured lung. The surgical team quickly noticed the smell of this volatile mixture in the air. A spark from the electrocautery device ignited a dry surgical pack on the patient's chest, and in the oxygen-rich environment, it caught fire. Fortunately, the fire was quickly extinguished, and the surgery continued successfully. This was not a unique occurrence. It marked the eighth chest cavity fire during surgery, and like the Australian case, all had involved lungs, electrocautery devices, increased oxygen, and surgical packs—yet none resulted in harm to the patients.
1. Doctors Swallowed Legos on Purpose

In 2018, six pediatricians from the United Kingdom and Australia decided to investigate how long it would take for a Lego piece to travel through the human digestive system. They each swallowed the heads of Lego figures, taking this rather strange step in their scientific exploration. As part of their study, each doctor had to sift through their own feces to retrieve the Lego head. To make the process more entertaining, they devised unique rating systems for their findings.
In the days leading up to and during the retrieval phase, they assessed stool consistency using the SHAT (Stool Hardness and Transit) scale. Every time someone found a Lego head, it was noted with a FART (Find and Retrieval Time) score. The results showed that it took between 27 hours to three days for the Lego heads to pass through the digestive system without any complications. Additionally, SHAT scores revealed that stool consistency remained unaffected. This curious experiment now adds to the limited studies that explore the impacts of swallowed toys. However, one question remains unanswered: why did one of the pediatricians never find his Lego head?
