Not all prescriptions end with a trip to the pharmacy. Nowadays, a doctor's note can lead you into virtual experiences or even fake surgeries. Homeless individuals might receive prescriptions for housing, and addicts could be given heroin. Even patients who visit their GPs too often might find themselves sent off to Bingo or enrolled in Bollywood dance lessons.
10. Depression – Books

In the United Kingdom, doctors now have the option to prescribe books. For patients battling depression, a prescription for 'bibliotherapy' can be provided by a physician. But this prescription isn't for any book you wish to pick up. It’s reserved for those dealing with moderate depression and can be exchanged at the library for specific titles chosen by the doctor. Forget your favorite Harry Potter book—these are self-help reads related to depression, anxiety, OCD, diet, and overall well-being.
The goal is to help patients feel less isolated and to experience catharsis that offers solutions. Bibliotherapy has been proven effective with children, especially those dealing with tough life situations like death and divorce. While it can't cure depression on its own, it might provide an additional support in managing the condition.
9. Healthier Lifestyles – Community Gardening

The National Health Service (NHS) is promoting 'green prescriptions.' And no, this doesn’t mean marijuana. Instead, the term refers to connecting with nature for its health benefits, with a specific focus on community gardening.
Engaging in community gardening can reduce feelings of loneliness, anxiety, and depression. But what makes this group of gardeners so effective together? A collaborative project fosters better habits, encouraging long-term participation. It cultivates a sense of community and motivates people to walk more, especially if the garden is within walking distance. Many community gardens also yield fresh vegetables, offering produce that’s either free or more affordable than what you'd find in stores. Furthermore, planning and caring for the garden can improve communication and problem-solving skills. A flourishing garden can even enhance the environment—growing trees helps absorb harmful carbon emissions and provides shelter for birds and wildlife.
8. Mental And Physical Health – Museum Visits

In 2018, the Francophone Association of Doctors in Canada (MfdC) proposed an intriguing question to physicians: Would they consider museum visits as part of treatment? Over 100 doctors joined the program, supporting the initiative based on research that suggests visual art can have a positive impact on overall health.
A doctor will offer a free access pass to the Montreal Museum of Fine Arts (MMFA). This prescription allows two adults and two children to visit the museum together, providing an added bonus. While patients explore the artwork, they also get to spend quality time with family or friends. Socializing in a tranquil environment helps alleviate the stress that can exacerbate many health conditions.
Introducing museum visits as a form of medical treatment is a groundbreaking move. Even more impressive, doctors can recommend it for a variety of conditions, including trauma, anxiety, depression, epilepsy, autism, and Alzheimer’s. Essentially, most mental and physical health issues could potentially benefit from this unique program.
7. Health Management – Nature

Following a successful trial period, doctors in Scotland can now officially prescribe patients to embrace the great outdoors. Since 2018, nature has been recognized as a formal treatment to either alleviate existing conditions or lower the risk of developing certain diseases, such as diabetes, cancer, hypertension, and stress. It may sound unusual, but extensive research has shown that spending time in nature has a profoundly positive impact on both the mind and body.
This program, called 'Nature Prescriptions,' allows doctors to give patients a pamphlet outlining how nature serves as a powerful therapeutic tool. The pamphlet also includes a seasonal guide, suggesting activities like lichen hunting in January, gardening in February, and walking dogs in March. Other recommendations include gazing at clouds or throwing stones into the ocean after writing down personal concerns. Patients are encouraged to tap into their creativity while outdoors, embracing the natural world to relieve stress through activities like hiking, birdwatching, or simply enjoying the breeze.
6. Mental and Heart Health – Bike Rides

In 2019, Wales launched a groundbreaking pilot program aimed at improving cardiovascular health. Two medical centers in Cardiff, the country's capital, were granted the authority to prescribe bike rides. Not only does regular cycling reduce the risk of heart disease-related death by 52%, but it also lifts the mood. Plus, bicycles are an environmentally friendly alternative to cars and buses, which contribute to pollution.
The initiative allows doctors to provide patients with a six-month subscription to a local bike-rental service. In Europe, renting a bike can cost up to £10 (around $13) per day, which could discourage those looking to cycle their way to better health. However, with this six-month pass, anyone can freely explore the city on a bike. This program is the first of its kind in the UK and may spark future expansions. If successful, the UK could add more innovative activities to supplement traditional treatments.
5. Various Conditions – Placebos and Fake Surgery

In 2011, the German Medical Association (BÄK) conducted research on the use of placebos. Their findings revealed that half of all doctors in Germany prescribe placebos, with the rate soaring to 88% in Bavaria. Surprisingly, BÄK didn’t react negatively to these findings, despite the unconventional nature of placebo treatments.
The placebos included vitamin supplements, homeopathic remedies, and even simulated surgeries. The study discovered that in some cases, these fake treatments worked. Not only did they alleviate symptoms like mood swings and physical discomfort, but when combined with real medications, the effectiveness of the actual drugs increased. Interestingly, the success of the placebo depended on its appearance and cost. The cheaper the placebo, the less effective it was. Patients also had preferences regarding the size and color of pills, with injections being the most well-received form of placebo.
Although the exact reason for the success of placebos remains unclear, it might be linked to trust. When patients felt that their doctor truly listened and understood their concerns, the placebo treatments were more effective. However, BÄK made it clear that genuine medical treatments should never be withheld if a patient’s health could be compromised. The association also emphasized the importance of educating doctors about placebos and suggested the creation of international guidelines to regulate their use.
4. Bothering GPs – Bollywood Dancing

General practitioners often face an unusual challenge: patients booking appointments for issues that have nothing to do with medicine, such as loneliness, financial struggles, or housing problems. In London, nearly a third of GP visits are non-medical. This has placed an overwhelming burden on doctors, leading to long hours, burnout, and difficulties in recruiting new staff due to the heavy workload.
In response, Parchmore Medical Center in London introduced a program called 'community prescribing.' Launched in Croydon, it allowed doctors to prescribe activities designed to get people out of their homes and involved in their community. Each prescription was tailored to address the patient's specific issue. For example, those suffering from loneliness might be prescribed bingo or Bollywood dance lessons, while people with welfare concerns were directed to debt and housing meetings hosted in church halls.
During the 18-month trial, 112 different activities were offered, and approximately 30,000 social sessions were provided to patients. The results were encouraging. Participants became more socially active and more deeply involved with their communities. General practitioners (GPs) returned to regular hours, and outpatient referrals to Parchmore reduced by 20 percent in 2018.
3. Addiction – Heroin
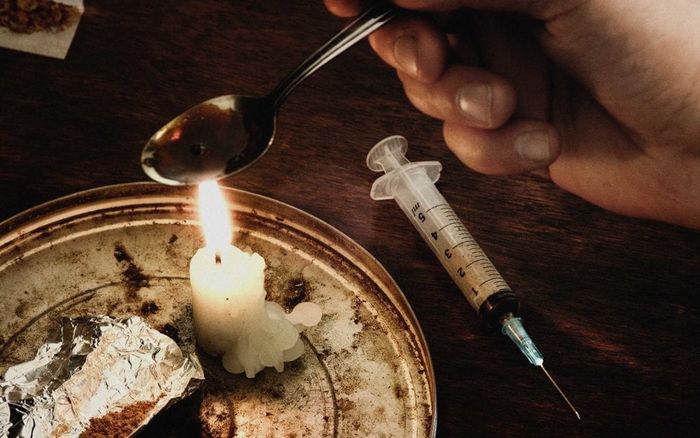
In 2016, the Canadian government passed a groundbreaking law that allows heroin addicts to legally access their drug. Access to diacetylmorphine, a medical-grade form of heroin, is strictly regulated. To qualify, patients must have failed all other treatment methods. A doctor must then submit an application to the health department on behalf of the patient. Each case is evaluated individually, and if approved, the department provides the diacetylmorphine.
This approach offers two main advantages. First, methadone is typically used to help people detox from heroin, but studies have shown that diacetylmorphine is more effective in helping people break their addiction. Those on methadone were more likely to turn to other substances. Second, the patient is supervised by medical staff during the injection, providing a safer, controlled environment that prevents overdose. The growing rate of overdose deaths in Canada was one of the main factors behind the adoption of this new treatment. This method is not unique to Canada; doctors in Denmark, the Netherlands, Germany, and Switzerland can also prescribe diacetylmorphine.
2. Burn Wounds – Virtual Reality

Shriners Hospital for Children is renowned as one of the leading burn care centers in the United States. The facility treats children who suffer from severe burn injuries, some of which cover up to 70 percent of their bodies or even their faces. Despite the hospital's exceptional care, even the strongest pain medications often fall short. As Hunter Hoffman puts it, the level of pain the children experience is “astronomically high.”
Hunter Hoffman, a cognitive psychologist and the director of the Washington-based Virtual Reality Research Center, alongside his team, devised a groundbreaking solution. The human attention span is finite, and pain demands a lot of focus. The concept was simple: if individuals could immerse themselves in a virtual world, their perception of pain could diminish as the brain's attention shifted to the simulated environment.
Incredibly, the idea proved successful. Since the children's injuries prevented them from wearing standard VR equipment, Hoffman used a robotic arm to position goggles near their faces. The game, titled 'SnowCanyon,' featured adorable Arctic creatures that players could hit with snowballs. The children were so engrossed in the igloos and the floating adventure along the canyon that nurses were able to tend to their wounds while the children played. As a result, their pain levels dropped by 50 percent.
1. Homelessness – A House

Hawaii receives a yearly Medicaid allocation of $2 billion, but a small segment of the population contributes disproportionately to the strain on this resource. Homeless individuals frequently visit emergency rooms for injuries, infections, mental health issues, and complications related to substance abuse. While Medicaid covers their treatment, the costs skyrocket as many of these individuals return within a week with renewed health problems. This cycle is exacerbated by their lack of proper shelter and the unsanitary conditions in which they live.
On average, Medicaid spends $120,000 per individual annually. In stark contrast, providing someone with housing costs only $18,000, making the choice clear. In 2017, a groundbreaking bill was introduced proposing that if homelessness were recognized as a medical condition, doctors could prescribe a house. Previous studies have shown that healthcare expenses decreased by 43% when the homeless were provided with stable housing. Despite the potential savings and improved well-being for the homeless, not everyone supports the bill. The Department of Human Resources Development is concerned it might be exploited to gain free housing, and there are worries the financial burden could still overwhelm the healthcare system.
