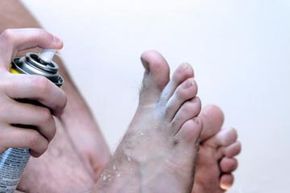
 Explore the Skin Problems Image Gallery to learn about athlete's foot, a prevalent fungal condition that affects certain individuals more frequently. View detailed images of various skin issues.
©iStockphoto.com/Jitalia17
Explore the Skin Problems Image Gallery to learn about athlete's foot, a prevalent fungal condition that affects certain individuals more frequently. View detailed images of various skin issues.
©iStockphoto.com/Jitalia17It’s like a scene from a horror film. Your toes itch uncontrollably, and a burning sensation engulfs your feet. Scratching brings no relief. Blisters form, the skin between your toes cracks, and the soles begin to peel. Lotions fail to soothe, and you notice discoloration in your toenails. The relentless itch and burning seem to spread. What’s happening? Is this an alien invasion?
The reality is far simpler. You’re dealing with athlete's foot, medically termed Tinea pedis. While it may feel like an extraterrestrial attack, it’s actually a common infection caused by stubborn, earthly microorganisms.
Athlete's foot belongs to a group of related skin conditions with similar names, such as Tinea corporis, Tinea capitis (scalp ringworm), and Tinea cruris (jock itch). Despite its less intimidating name, athlete's foot can be just as bothersome and challenging to treat as its counterparts [source: Mayo Clinic].
Athlete's foot, along with other Tinea infections, is caused by fungi, earning it the informal name "foot fungus." Fungi thrive in warm, humid environments, much like how bread molds quickly in summer heat. For many, the soles of the feet and the spaces between the toes provide the ideal warm, moist conditions for fungal growth.
To combat a fungal infection, read on to discover the causes of this irritating condition and effective strategies to overcome athlete's foot.
Causes of Athlete's Foot
Athlete's foot isn't caused by a single type of fungus. Instead, it results from various dermatophytes. These fungi grow on the skin, infecting the outer layer and prompting the deeper skin layer to overproduce cells. This buildup leads to the scaly appearance characteristic of athlete's foot [source: Mayo Clinic].
Athlete's foot typically appears on the soles of the feet and between the toes [source: WebMD]. However, since it is caused by various fungi and each foot is unique, its appearance, location, and treatment response can vary significantly.
To contract athlete's foot, you must first encounter the fungi responsible. This can happen through direct contact with an infected person or by touching contaminated surfaces or objects, such as floors, bath mats, bathtubs, or shoes. High-risk areas include public pools, bathrooms, and locker rooms, where people often walk barefoot [source: Mayo Clinic].
After exposure, the fungus requires a warm, moist environment to thrive, such as sweaty feet or cramped toes.
If the thought of foot fungi unsettles you, don’t worry. Keep reading to discover effective ways to prevent athlete's foot.
Individuals vary in susceptibility. While some never experience athlete's foot, others face recurring bouts. Health experts remain uncertain about why some are more prone to it. If you’ve had it before, your likelihood of recurrence is higher compared to those who haven’t [source: WebMD].
Preventing Athlete's Foot
The simplest and most effective way to prevent athlete's foot is to avoid contact with the fungus altogether [source: Family Doctor, TeensHealth]. Take proactive steps to minimize exposure. Wear waterproof sandals in locker rooms, public showers, or pools. Parents, equip your college-bound teens with inexpensive flip-flops. Athletes, be cautious—this condition is named for a reason, as sports often involve prolonged exposure to damp environments like locker rooms and showers.
Fungi thrive in warm, humid, and dark environments, but you can take steps to make your skin less inviting to these organisms.
- Maintain clean and dry feet.
- Swap out damp socks during the day.
- Remove shoes at home to let your feet breathe.
- Rotate shoes to allow them 24 hours to dry, especially if your feet sweat excessively.
- Avoid tight shoes that cramp your toes, as they create an ideal fungal habitat.
Opt for shoes made of natural materials to improve airflow and avoid plastic or vinyl footwear. Moisture-wicking socks, such as those made of cotton or specialized fabrics, can also help keep your feet dry [source: University of Michigan Health System].
To prevent athlete's foot from recurring, apply an antifungal powder daily. These powders help keep your feet dry and prevent fungal growth [sources: Mayo Clinic, WebMD].
When dealing with athlete's foot, adopt the habit of drying yourself from head to toe, saving your feet for last. This prevents spreading the fungus to other body parts. If it reaches the groin, it can cause jock itch, an uncomfortable and itchy condition [source: WebMD]. Always wash your towel after use to avoid spreading the infection.
Athlete's Foot Treatments
If preventive measures fail, mild cases of athlete's foot can be treated at home using over-the-counter antifungal medications. These products, available as sprays, creams, powders, or ointments, often contain clotrimazole, miconazole, terbinafine, or tolnaftate [sources: BlueCross BlueShield, Mayo Clinic]. Consistent use as directed, along with keeping your feet clean and dry, typically resolves the issue within a few weeks.
For persistent athlete's foot, consult a doctor. They may prescribe stronger topical treatments containing naftifine, butenafine, miconazole, or clotrimazole [source: WebMD]. If symptoms persist, oral medications like itraconazole, fluconazole, or terbinafine may be recommended [source: Mayo Clinic]. Due to potential side effects, these are usually reserved for severe or treatment-resistant cases.
Regardless of the treatment method, adopting preventive measures is crucial to stop the fungus from spreading to others at home, the gym, your sports team, or elsewhere until the condition is fully resolved.
Some individuals have found relief using alternative or natural remedies for athlete's foot, particularly in mild cases when combined with proper hygiene and foot care. Tea tree oil, derived from the Melaleuca alternifolia tree, is popular for its mild antifungal and antibacterial properties, which can alleviate symptoms. Garlic, containing the natural antifungal compound ajoene, is also used [source: CIGNA].
