 Seeking immediate dental care can halt the progression of early gum disease and prevent it from advancing.
Hemera/Thinkstock
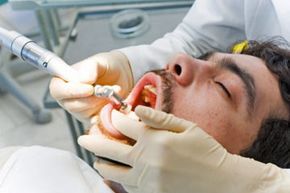
Seeking immediate dental care can halt the progression of early gum disease and prevent it from advancing.
Hemera/ThinkstockNoticing blood on your toothbrush after brushing is alarming, and persistent bad breath shortly after cleaning your teeth is equally troubling. Symptoms like soreness, sensitivity, and loose teeth are also concerning. These are clear indicators of gingivitis or periodontitis, two forms of gum disease. Whether these signs appeared recently or have been present for a while, it's crucial to take both preventive and corrective measures. Teeth and gums rely on each other for health, and any disruption to their bond can lead to serious consequences, including tooth loss.
Gum disease is a condition where the gum tissues fail to function as intended, leading to deterioration. Healthy gums are typically pink, smooth, and moist, with a firm attachment to the teeth. Blood vessels and nerves supply essential nutrients and sensations, ensuring the gums stay firmly connected to the teeth, keeping them stable and functional for chewing and digestion.
When gums are neglected or attacked by plaque buildup, illness, or hormonal shifts, gingivitis begins to take hold. This early stage of gum disease disrupts the bond between teeth and gums. Essentially, gingivitis is inflammation of the gums, while periodontitis is a severe form of gum disease that affects the entire tooth structure, potentially destroying gums, supporting tissues, and even underlying bones [source: NIH].
While both gingivitis and periodontitis are forms of gum disease, they differ in severity. Advanced gum disease results in heightened bacteria, toxins, and infections, prompting the immune system to respond. However, this defense mechanism can backfire, as the body destroys gum tissues and bone in its attempt to combat the infection. This collateral damage weakens the support structure, often leading to tooth loss [source: NIH].
How can you identify when your gums, teeth, and immune system are in conflict, and disease has taken hold? Sometimes it’s not obvious, but we’ll explore some clear signs of this breakdown next.
Gum Disease Symptoms
In its initial stages, mild gum disease, or gingivitis, often goes unnoticed. By the time symptoms become visible, the gums have likely been deteriorating for some time. Noticing blood on your toothbrush during or after brushing, or even randomly, is a significant warning sign. Other symptoms of gum disease include:
- Tender, inflamed, and reddish gums
- Persistent bad breath, or halitosis, that returns shortly after brushing
- Swelling around the gum base
- Gaps or loose sections in the gum line where teeth and gums are pulling apart
- Yellowish or white pus between the gums and teeth
- Pain or discomfort at the tooth roots while eating, brushing, or flossing
- An intermittent unpleasant taste in the mouth throughout the day
- Loose teeth or a sensation that your bite is changing [source: Mayo Clinic]
Sometimes, even without obvious symptoms, you might notice a buildup or rough ridge where the teeth and gums meet, or areas where floss gets stuck. These deposits are hardened plaque, or tartar, which clings to teeth and irritates gum tissue, causing inflammation. (The suffix "-itis" in gingivitis and periodontitis refers to inflammation.)
When everything seems fine and our teeth appear healthy, it’s tempting to skip dental visits. Why schedule a checkup every six months if your mouth feels fine? The primary reason is to prevent tartar buildup from lingering too long and causing gum inflammation and irritation.
If you notice any signs of gingivitis, such as visible, tactile, or taste-related issues, visiting a dentist immediately can halt early gum disease and prevent it from progressing. The good news is that gingivitis is reversible, allowing gums to return to their healthy state. While periodontitis isn’t reversible, it can still be managed effectively.
Next, we’ll explore the causes of gum disease and how to prevent it before it begins.
In dental and medical fields, a professional's specialty is often revealed in their title. Discussing gum disease involves understanding both the roots of teeth and the origins of words. For instance, "dent-" refers to teeth, "perio-" means around or surrounding, "endo-" signifies within or inner, and "odont" also means tooth. A dentist primarily focuses on teeth, a periodontist specializes in the structures supporting teeth—like gums—and an endodontist deals with the inner parts, or roots, of teeth. According to Merriam-Webster, hygiene means promoting health through cleanliness, and a dental hygienist collaborates with other dental professionals and patients to maintain healthy, clean teeth and gums.
Gum Disease Causes
Inconsistent or poor dental hygiene is the leading cause of gingivitis and its progression to more severe gum disease. Neglecting brushing, flossing, and regular dental visits allows plaque to accumulate and harden into tartar on teeth and below the gum line. This buildup creates a barrier, making it difficult for gums to adhere to tooth surfaces. As the gap between teeth and gums widens, bacteria multiply beneath the gum line. Every time food particles and debris remain in the mouth, bacteria thrive, spreading rapidly and infiltrating the spaces between teeth and gums. These pockets expand as gums detach from teeth, and untreated gingivitis can lead to irreversible tissue breakdown and advanced gum disease.
Even with excellent oral hygiene, gingivitis can sometimes persist, requiring more aggressive measures. Life stages like puberty, pregnancy, and menopause bring hormonal shifts that disrupt balance. For example, increased progesterone during pregnancy boosts blood flow to the mouth, causing gums to swell and become tender. This makes gum tissues more susceptible to bacteria as they pull away from teeth, and brushing may even cause pain. Known as pregnancy gingivitis, this condition not only causes discomfort and potential long-term gum damage but may also contribute to low birth weight or premature delivery.
Research suggests a connection, though not definitive, between a mother's oral health and a healthy, full-term pregnancy, as well as the baby's birth weight. Pregnancy gingivitis is widespread, so additional preventive measures against gum disease are essential. Women also experience hormonal changes affecting gum health during menopause, often due to dry mouth, as well as from taking oral contraceptives [sources: AAP; ADA; March of Dimes].
Gingivitis and periodontitis can affect individuals of any age due to illness or disease. Short-term viral infections can spike bacteria levels in the mouth, while chronic conditions maintain this imbalance over years. Diabetics, for instance, face a higher risk of infections and must combat bacteria in both their bodies and mouths. Similarly, those with heart disease are more susceptible to infections entering the bloodstream, and while links between gum disease and heart issues are noted, they remain inconclusive.
People with weakened immune systems, such as those with malnutrition or HIV, are at greater risk for gum disease due to reduced resistance to harmful microbes and infections. Genetics also play a role, as some individuals are naturally prone to gum issues. Even those in good health but with poor diets lacking essential vitamins and nutrients face increased risks of gum disease [source: AAP]. Smoking further elevates the likelihood of gum disease and complicates treatment [source: NIH].
Just learning about these risk factors might make your mouth ache a bit, so let’s explore some treatment and relief options next.
Gum Disease Treatment
 Periodontal probes feature grooves that measure the depth of pockets between gums and teeth. Dentists gently insert the probe into the gum line and note where it stops to assess the progression of gum disease.
iStockphoto.com/Rich Legg
Periodontal probes feature grooves that measure the depth of pockets between gums and teeth. Dentists gently insert the probe into the gum line and note where it stops to assess the progression of gum disease.
iStockphoto.com/Rich LeggBefore diving into the details of treating periodontitis, or advanced gum disease, let’s reiterate the excellent news about gingivitis: it’s both treatable and reversible. If you notice the symptoms discussed earlier, it’s crucial to visit a dentist promptly to address the issue. Once plaque hardens, whether above or below the gum line, professional cleaning is necessary to remove it.
Dentists and hygienists use ultrasonic tools and traditional dental instruments to remove tartar buildup, restoring teeth to their smooth state. As inflammation decreases, gums can reattach to tooth surfaces. With proper follow-up care, the likelihood of gingivitis recurring diminishes until plaque accumulates again.
If gingivitis goes untreated and periodontitis progresses, a dentist may begin by assessing the severity of the issue. Periodontal probes, though often dreaded, are essential for evaluating gum damage and determining the necessary treatment. These probes have grooves that measure pocket depths between gums and teeth. By gently inserting the probe and noting its stopping point, dentists can gauge the extent of gum disease. Healthy gums typically have 1 to 3 millimeters of space, while deeper pockets indicate diseased tissues and the need for thorough cleaning [source: NIH].
Treating gum disease involves addressing the entire mouth, not just the gums. Since gingivitis begins with plaque and tartar buildup on teeth, which irritates gum tissues and prevents them from adhering tightly to teeth, cleaning the teeth is a critical part of treatment. Combating toxins and infections within the pockets is also vital. When deep pockets form, the dentist or periodontist may perform one or more procedures:
- Scaling -- Eliminating tartar buildup from teeth both above and below the gum line
- Root planing -- Removing residual buildup and smoothing rough areas along the sides of teeth and roots
- Killing bacteria -- Applying topical medications like rinses and gels or prescribing oral antibiotics to eliminate and control bacteria in the mouth and/or body
- Surgery and grafts -- Retracting gums to access and clean thoroughly, and grafting new tissues or bones to restore receded areas. Some procedures aim to stimulate bone regeneration.
Dental professionals use probes and visual exams to evaluate damage and create a treatment plan. X-rays help detect bone loss between roots, gums, and jawbones. In cases of severe damage or bone loss, teeth may need extraction, but dentists prioritize saving teeth. Gum disease treatments often involve aggressive measures to eliminate bacteria, repair tissues, and restore root and bone health to preserve teeth. While not reversible, gum disease is highly manageable [sources: NIH; Mayo Clinic; AAP].
Toxins, root cleaning, antibiotics, and surgery—can all this be avoided? In most cases, yes. Let’s explore ways to improve your oral care and gum health next.
Gum Disease Prevention
If your gums are healthy, pink, and firmly attached to your teeth, that’s excellent—still, visit a dentist regularly. Routine checkups every six months, as advised by your dentist, can prevent and eliminate gingivitis. By stopping gingivitis early, you can avoid periodontitis. If your gums are sore, red, or unhealthy, see a dentist immediately. It’s often less severe than you imagine and can save you significant costs and time in the future.
Whether you’re symptom-free or experiencing multiple issues, starting with clean teeth can help you regain control of your daily oral hygiene. Before leaving the dentist’s office, consider revisiting the basics of oral care. Many of us learned to brush and floss at such a young age that we might have missed key details. Regardless of your age, having a hygienist or dentist demonstrate proper brushing and flossing techniques, and recommend products tailored to your needs, can uncover surprising mistakes or areas for improvement.
Brushing at least twice daily—or after every meal—and flossing once a day are the foundational steps. Avoid brushing too aggressively, as this can harm gums and cause them to recede. A diet rich in vitamins also supports overall tissue health. Consulting a dentist at the first sign of redness or discomfort can prevent infections from spreading. While factors like illness, medications, or genetics may make gum disease unavoidable, working closely with a dental professional and maintaining diligent care can prevent symptoms from worsening and protect against tissue and bone loss. If tooth loss has already occurred, maintaining gum health is crucial for supporting dentures or other restorations.
Spending a few minutes twice a day on brushing, a couple more on daily flossing, and attending biannual tartar removal appointments can help maintain a strong bond between your teeth and gums, often for a lifetime.
Is gum disease contagious? Research suggests that casual contact or sharing drinks and utensils is unlikely to spread gum disease. However, the bacteria responsible for gum disease can transfer between long-term partners who frequently exchange saliva. If you have periodontitis, consult your dentist or periodontist on how to minimize the risk of spreading infections until the condition is managed [source: UMMC].
