 From PET scans to chemotherapy, nuclear materials are applied in various medical treatments. JohnnyGreig / Getty Images
From PET scans to chemotherapy, nuclear materials are applied in various medical treatments. JohnnyGreig / Getty ImagesIn hospitals or featured on television, you may have observed patients receiving radiation therapy for cancer or doctors prescribing PET scans to make diagnoses. This falls under the field of nuclear medicine. It involves the use of radioactive substances to both image the body and treat illnesses. By focusing on both physiology (how the body functions) and anatomy (the body's structure), nuclear medicine plays a vital role in diagnosis and treatment.
This article aims to explain some of the key techniques and terminology used in nuclear medicine. You’ll discover how radiation enables doctors to look deeper into the human body than ever before.
Imaging Techniques in Nuclear Medicine
One of the challenges with the human body is its opacity, making it difficult to view the internal organs without causing discomfort. In the past, exploratory surgery was a common method to gain insight into the body, but now doctors have access to a wide variety of non-invasive techniques. These include X-rays, MRI scanners, CT scans, ultrasounds, and more. Each of these methods offers distinct advantages and drawbacks, making them suitable for different medical conditions and body areas.
Nuclear medicine imaging methods provide an additional means for doctors to examine the inside of the body. These methods integrate computers, detectors, and radioactive substances to produce detailed images. Some of these methods include:
- Positron Emission Tomography (PET)
- Single Photon Emission Computed Tomography (SPECT)
- Cardiovascular Imaging
- Bone Scanning
Each of these imaging methods utilizes the unique characteristics of radioactive elements to generate an image. For a deeper understanding, see 'How Radioactivity Works' for further details.
Nuclear medicine imaging is essential for identifying:
- tumors
- aneurysms (weak areas in blood vessel walls)
- abnormal or insufficient blood flow to different tissues
- disorders related to blood cells and underperformance of organs, such as issues with thyroid or lung function.
The selection of a specific test, or a combination of tests, depends on the symptoms presented by the patient and the nature of the disease being diagnosed.
Positron Emission Tomography (PET)
PET generates images of the body by detecting radiation emitted from radioactive substances. These substances are injected into the body, usually marked with a radioactive atom like Carbon-11, Fluorine-18, Oxygen-15, or Nitrogen-13, which have brief decay times. These atoms are created by bombarding regular chemicals with neutrons to produce short-lived radioactive isotopes. PET identifies the gamma rays emitted when a positron from the radioactive substance interacts with an electron in the tissue (Figure 1).
During a PET scan, a patient is injected with a radioactive substance and positioned on a flat table that moves step-by-step through a 'donut'-shaped enclosure. This enclosure houses a circular array of gamma ray detectors (Figure 2), which consists of a series of scintillation crystals, each linked to a photomultiplier tube.
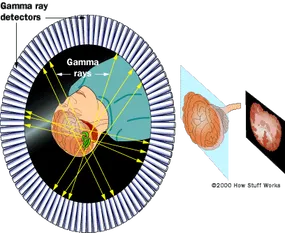 Figure 2
Figure 2The crystals transform the gamma rays emitted by the patient into photons of light, and the photomultiplier tubes then convert and amplify these photons into electrical signals. These signals are processed by a computer to create images. The table moves and the procedure is repeated, producing a sequence of thin slice images of the body in the targeted area (e.g., brain, breast, liver). These images can then be combined to form a 3D model of the patient's body.
PET provides visualizations of blood flow or other biochemical activities, depending on the type of molecule that is labeled with the radioactive substance. For example, PET can reveal glucose metabolism in the brain or rapid changes in activity in different body areas. However, there are only a limited number of PET centers across the country as they must be located near a particle accelerator, which produces the short-lived radioisotopes required for the procedure.
SPECT, Cardiovascular Imaging and Bone Scanning
SPECT is a technique similar to PET, but the radioactive substances used in SPECT (such as Xenon-133, Technetium-99, Iodine-123) have longer decay times than those in PET, and they emit single gamma rays rather than double. SPECT can provide insights into blood flow and the distribution of radioactive substances within the body. Although the images from SPECT are less sensitive and detailed compared to PET, the technique is more cost-effective. Furthermore, SPECT centers are more widespread because they do not need to be located near a particle accelerator.
Cardiovascular imaging methods use radioactive substances to track blood flow through the heart and blood vessels. A common example is the stress thallium test, where the patient is injected with a radioactive thallium compound, exercises on a treadmill, and is imaged with a gamma ray camera. After resting, the procedure is repeated without exercise. Comparing the images before and after exercise reveals changes in blood flow to the heart. These techniques are valuable for identifying blocked arteries or arterioles in the heart and other tissues.
Bone scanning detects radiation from a radioactive substance (technetium-pp methyldiphosphate), which accumulates in bone tissue due to its affinity for phosphorus compounds. This substance gathers in areas with high metabolic activity, creating images that show bright spots of high activity and dark spots of low activity. Bone scans are particularly useful in detecting tumors, which tend to have higher metabolic activity.
Treatment in Nuclear Medicine
In nuclear medicine imaging tests, the radioactive substances injected into the body do not cause harm. The radioisotopes used decay quickly, typically within minutes to hours, and they have lower radiation levels than typical X-rays or CT scans. These substances are also eliminated from the body through urine or bowel movements.
Some cells are significantly impacted by ionizing radiation, such as alpha, beta, gamma rays, and X-rays. Cells grow at various rates, and those that divide faster are more vulnerable than typical cells due to two key reasons:
- Cells possess a mechanism that can repair damaged DNA.
- If a cell detects DNA damage during division, it will undergo self-destruction.
Cells that divide rapidly have less time for the repair system to identify and correct DNA mistakes before they replicate, making them more prone to self-destruction when damaged by radiation.
Since many cancers involve cells that divide quickly, radiation therapy is sometimes used as a treatment. This involves placing radioactive wires or vials near the tumor, and for deeper or harder-to-reach tumors, high-intensity X-rays are focused on the affected area.
The challenge with this method is that healthy cells that also reproduce rapidly can be affected by radiation alongside the cancerous cells. Hair cells, cells in the stomach and intestines, skin cells, and blood cells all multiply quickly, making them vulnerable to radiation. This explains why cancer patients often experience hair loss and nausea during treatment.
Radioactive tracers, created from nuclear materials, can be injected into the bloodstream. One type of tracer travels through the blood, allowing the blood vessels' structure to be visualized. This technique helps detect clots and other abnormalities in the blood vessels. Additionally, certain organs in the body absorb specific chemicals; for instance, the thyroid gland absorbs iodine. By injecting radioactive iodine into the bloodstream, thyroid tumors can be identified. Similarly, cancerous tumors tend to absorb phosphates. Injecting the radioactive phosphorus-32 isotope into the bloodstream allows tumors to be located by their heightened radioactivity.
