 Individuals with hyperhidrosis may sweat four to five times more than the average person. Explore stunning skin care visuals for more insights.
Noa/Photonica/Getty Images
Individuals with hyperhidrosis may sweat four to five times more than the average person. Explore stunning skin care visuals for more insights.
Noa/Photonica/Getty ImagesPicture preparing for work and needing to change outfits before stepping out due to excessive sweating. After padding your shirt's armpits to minimize sweat, you pack extra clothes for later. Breakfast becomes a struggle as your mug slips from sweaty hands, and holding a fork feels impossible. You're thankful you declined your colleagues' breakfast invite -- enduring this in public is too much.
Sweaty palms make gripping the steering wheel tough, forcing you to drive with extra care. Upon reaching work, your socks and shoes are drenched. Sitting at your desk, you brace yourself for another challenging day.
This is a snapshot of life with hyperhidrosis. Sweating occurs constantly, without typical triggers like exercise, heat, or anxiety.
Hyperhidrosis, also known as diaphoresis, is characterized by excessive sweating. Those affected may produce sweat at levels four to five times higher than average, far exceeding the body's typical cooling needs.
This condition manifests in various forms and differs in intensity among individuals. Let's delve deeper into who is affected by hyperhidrosis and its implications.
On a brighter note, sweat plays a role in protecting the body from infections by washing away bacteria and harmful microbes from the skin's surface. It also contains lysozyme, an enzyme that can break down the cell walls of certain pathogens, enhancing this protective function.
Hyperhidrosis Focal Areas
Hyperhidrosis is categorized into two primary types: secondary and primary. Secondary hyperhidrosis occurs due to an underlying medical condition or medication, leading to excessive sweating. In contrast, primary hyperhidrosis is the condition itself, where excessive sweating is the main issue. Individuals with secondary hyperhidrosis often sweat all over their bodies, regardless of whether they are awake or asleep. Those with primary hyperhidrosis, however, tend to sweat in specific focal areas, primarily while awake.
The primary focal areas include:
- Armpits (axillary hyperhidrosis)
- Hands (palmar hyperhidrosis)
- Feet (plantar hyperhidrosis)
- Face and other parts of the head (facial hyperhidrosis)
While the exact cause of excessive sweating remains unclear, researchers have identified a genetic connection in some instances. Approximately 40 to 60 percent of cases involve multiple family members. For the remaining cases, ongoing clinical studies aim to uncover why the brain triggers such an intense sweating response.
It is estimated that hyperhidrosis impacts 1 to 3 percent of the population. Many individuals first notice symptoms during adolescence, though the condition can begin in childhood. While rare, some cases of hyperhidrosis do emerge in adulthood.
What exactly occurs in the body of someone with hyperhidrosis, and how does it differ from regular sweating? Continue reading to discover more.
Anhidrosis, also known as anhydrosis, is a condition where little to no sweat is produced. This can be dangerous, even life-threatening, especially in hot climates. Anhidrosis can also affect specific areas of the body, reducing its severity. Potential causes include disorders like Guillain-Barre syndrome or ectodermal dysplasia, as well as burns, skin injuries, or diseases. Drug side effects and dehydration are other possible triggers. Congenital insensitivity to pain with anhidrosis (CIPA) is another disorder where sweating is absent. For more details, explore How CIPA Works.
Hyperhidrosis Causes
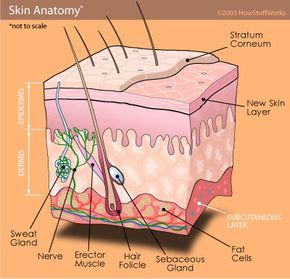 Sweat glands are coiled just beneath the skin's surface.
Mytour 2005
Sweat glands are coiled just beneath the skin's surface.
Mytour 2005For most individuals, low-level sweating is a continuous process, with much of the sweat reabsorbed by the body. High-level sweating, however, is triggered by factors like exercise, heat, or emotional stimuli such as anxiety or fear. To understand more about sweat gland functionality, read How Sweat Works.
The nerves responding to stress are guided by the sympathetic nervous system, a component of the autonomic nervous system. This system prepares the body to handle danger or stress by increasing sweat production. It achieves this by releasing acetylcholine, a neurotransmitter stored in small sacs between nerves and sweat glands. When released, acetylcholine activates the sweat glands, which continue to function until the chemical is depleted. If the threat persists, more acetylcholine is released to sustain the response.
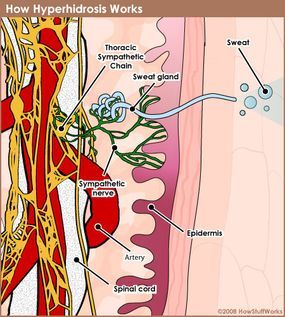 In individuals with hyperhidrosis, the nervous system overstimulates the sweat glands.
Mytour 2008
In individuals with hyperhidrosis, the nervous system overstimulates the sweat glands.
Mytour 2008For those with hyperhidrosis, the nerves connected to sweat glands in specific areas occasionally overreact, producing sweat without any apparent cause. The intensity, frequency, and duration of these episodes vary. While the exact reason for this overactivity remains unclear, the nerves flood the sweat glands with excessive acetylcholine, creating a challenging situation for those affected.
What does living with hyperhidrosis feel like? Is it as simple as applying extra deodorant before leaving home? Continue reading to learn more about the daily experiences of those with hyperhidrosis.
Living with Hyperhidrosis
 Hyperhidrosis impacts both physical and mental well-being.
Paul Burns/Blend Images/Getty Images
Hyperhidrosis impacts both physical and mental well-being.
Paul Burns/Blend Images/Getty ImagesWhile hyperhidrosis isn't fatal, it can profoundly influence every facet of a person's life, often causing significant emotional distress. The unpredictability of the condition is particularly challenging, as it doesn't require specific triggers like spicy food or heat. Sweating can occur suddenly and without warning.
Individuals with hyperhidrosis frequently experience depression, social anxiety, low self-esteem, difficulties in forming relationships, frustration with daily activities, and reduced productivity at work. The embarrassment and anxiety caused by excessive sweating can exacerbate the condition, creating a relentless cycle that's hard to escape.
Hyperhidrosis also carries a financial burden. Those affected often spend more on:
- Shoes, socks, shirts, and moisture-wicking clothing
- Dry cleaning and stain-removal products
- Toiletries and antiperspirants, including both over-the-counter and prescription options
- Pads, towels, handkerchiefs, and other sweat-absorbing items
Frequent visits to the doctor for treatments (discussed later) may be necessary, and some health insurance plans might not cover these costs. However, financial aid could be available if the treatment is deemed a medical necessity.
There is hope, though. Next, we'll explore various treatment options for those dealing with severe sweating.
Excessive sweating -- not always hyperhidrosis -- has appeared in TV shows and movies like "Twin Peaks," "Seinfeld," and "Broadcast News."
Noninvasive Treatments for Hyperhidrosis
Individuals with hyperhidrosis can try various treatments to find one that suits their needs and lifestyle. Doctors usually recommend starting with the least invasive methods and progressing as necessary.
The simplest approach to managing sweating is using antiperspirants, available in various strengths, both over-the-counter and prescription. These products block sweat gland ducts, preventing sweat from reaching the skin's surface. Their active components are metallic salts, often aluminum-based compounds like aluminum chloride hexahydrate, commonly found in prescription antiperspirants. Many individuals with hyperhidrosis apply antiperspirants to areas beyond the armpits, such as the feet, to reduce sweating (though this may cause skin irritation). For more details, read What is in an antiperspirant that stops sweat?
When antiperspirants fail, iontophoresis is often the next option. This treatment is effective for palmar, plantar, and axillary hyperhidrosis, though its exact mechanism remains unclear. For many users—up to 80 percent—it delivers significant results, often reducing or temporarily halting sweating [Source: International Hyperhidrosis Society].
Iontophoresis, reportedly used as early as 1740 for arthritis, is a straightforward procedure [Source: International Hyperhidrosis Society]. It involves placing hands or feet in shallow water trays charged with a mild electrical current. This ionizes the water particles, allowing them to penetrate the skin. Treatments can be done by a dermatologist or at home using specialized machines.
Several theories explain how ionized particles disrupt sweating. Some suggest they block sweat glands or interfere with nerve signals, but no definitive explanation exists.
Iontophoresis sessions last 20 to 40 minutes and require frequent initial treatments. Over time, maintenance may only be needed weekly or monthly. Padded electrodes can also target underarm sweating.
For those seeking a less frequent but costlier solution, Botox injections can halt underarm sweating. Approved in both the U.S. and U.K. for axillary hyperhidrosis, Botox can also be used on hands, feet, and the face. This purified botulinum toxin protein blocks nerve signals that overactivate sweat glands. Results typically last between three to 16 months, with potential follow-up injections to address missed areas.
Additional treatments include astringents and topical or oral medications.
For severe cases requiring long-term solutions, more invasive treatments are available. We'll explore these next.
The human body contains two to four million sweat glands, primarily concentrated on the feet, hands, armpits, and face.
Surgical Options for Hyperhidrosis
In the most severe cases of hyperhidrosis, surgery may be considered, though it carries the highest risk. Endoscopic Thoracic Sympathectomy (also known as Endoscopic Transthoracic Sympathectomy or ETS) involves cutting or clamping nerves that trigger sweating in specific upper body areas. ETS is most effective for severe palmar hyperhidrosis. For lower body sweating, a similar procedure called lumbar sympathectomy can be used to address plantar hyperhidrosis.
Various treatments target excessive sweating through different mechanisms.
Other surgical methods include localized procedures such as removing sweat glands through cutting, scraping, or suctioning, or a combination of these techniques. These approaches, like the ones mentioned earlier, come with potential side effects, so consulting a skilled doctor is essential.
A common and frustrating side effect of surgery is compensatory sweating. Since the body is accustomed to excessive sweating, it compensates by producing sweat in new areas post-surgery. For instance, after ETS, a patient might find their hands dry but experience excessive sweating on their back or stomach. Researchers are working to refine these treatments to minimize compensatory sweating and other adverse effects.
There are two types of sweat glands: eccrine and apocrine. Eccrine sweat, composed of water, potassium, chloride, and sodium, is odorless. The unpleasant smell associated with sweating comes from apocrine glands, which produce sweat containing proteins and fatty acids. Bacteria on the skin break these down, creating body odor. Most apocrine glands are in the armpits, which is why deodorants are so effective.
