 We’ve all experienced the prune-like wrinkles on our skin after soaking in a hot bath for too long. This phenomenon is scientifically referred to as skin maceration.
Stockbyte/Stockbyte/Thinkstock
We’ve all experienced the prune-like wrinkles on our skin after soaking in a hot bath for too long. This phenomenon is scientifically referred to as skin maceration.
Stockbyte/Stockbyte/ThinkstockIt’s the shriveled fingers and toes we notice after spending too much time in a hot bath. It’s also the overly tender skin that forms when a bandage is left on too tightly for hours. This condition is known as skin maceration, and while it’s generally harmless, it’s important to understand how to manage it.
Skin maceration happens when the skin remains wet for prolonged periods, and chances are, you’ve encountered it multiple times. It often occurs when bandages are applied to minor cuts or more serious wounds needing medical attention. You might also have observed it after wearing non-breathable gloves made of plastic or latex, which lock moisture against the skin.
Maceration frequently happens during wound care as the skin beneath the bandage gets damp from sweat, urine, or other bodily fluids. This surplus moisture is often referred to as hyperhydration.
The initial indicator of over-hydrated skin is the appearance of wrinkles. Additionally, macerated skin turns exceptionally soft and develops a whitish hue. However, this white skin should not be mistaken for the pale, whitish look of new epithelial tissue forming in a healing wound.
While most cases of maceration resolve quickly once the skin is exposed to air and allowed to dry, prolonged maceration can make the skin prone to fungal and bacterial infections. As opportunistic organisms invade the area, it may become itchy or emit an unpleasant odor.
Furthermore, because the skin becomes much softer, it is also more prone to damage from rubbing or friction. Continue reading to learn how to prevent skin maceration and avoid it escalating into more serious issues.
Preventing Skin Maceration
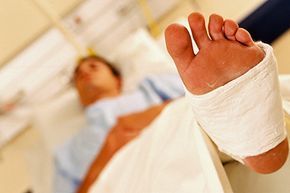 Bandages frequently trap too much moisture against the skin, leading to maceration.
Pixland/Pixland/Thinkstock
Bandages frequently trap too much moisture against the skin, leading to maceration.
Pixland/Pixland/ThinkstockMaceration is often seen as an early warning sign of more severe issues. In elderly or immobile individuals, if not managed properly, it can indicate the onset of pressure sores or friction-related injuries.
Maceration has also been associated with delayed wound healing. Proper wound care and careful bandage application can significantly minimize maceration and prevent further complications.
You’ve likely observed how your macerated skin gradually returns to its normal state after a long bath, even without any special treatment.
However, resolving this condition can be more challenging in certain cases. Maceration is common among elderly, bedridden individuals dealing with incontinence. Bedding retains moisture against the skin, and prolonged immobility leads to maceration, making the skin vulnerable to bed sores and infections. Therefore, it’s crucial to reduce and monitor moisture levels.
If maceration is happening near a bandaged wound, reassessing your bandaging approach may be necessary. Since healing wounds release fluid (known as exudate), the area can remain damp. In severe wounds, exudate may saturate the bandage faster than it can evaporate, even with air exposure.
In such scenarios, maceration can worsen and lead to complications. More frequent bandage changes may be required to maintain minimal moisture levels.
If the bandage covers a large area, it can also cause heat buildup, prompting the body to sweat as a cooling mechanism. This sweat can get trapped under an overly tight bandage. Switching to a smaller or more breathable bandage might help.
Lowering moisture levels also minimizes bacterial growth, significantly reducing the risk of infection in the macerated area. This leads to faster wound healing and prevents additional skin damage.
To explore more fascinating medical topics, proceed to the next page.
