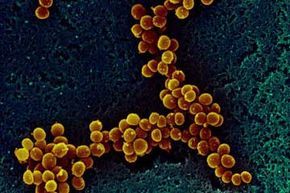
 Once confined to hospitals, staph bacteria can now be encountered almost anywhere, making infections more widespread. S. Lowry/Univ Ulster/Getty Images
Once confined to hospitals, staph bacteria can now be encountered almost anywhere, making infections more widespread. S. Lowry/Univ Ulster/Getty ImagesHospital stays often highlight the extensive measures taken to prevent infections, with staph infections being among the most severe. These infections, caused by Staphylococcus bacteria, can affect various parts of the body, including the skin, lungs, urinary tract, heart, and bloodstream. To grasp their impact today, it’s essential to explore their historical evolution over the past few centuries.
In 1881, Scottish surgeon Sir Alexander Ogston identified and named Staphylococcus as the primary culprit behind wound infections. Before this discovery, the cause of such infections was unknown. The breakthrough came in 1928 with the discovery of penicillin, which was first used in 1941 to treat a British policeman infected with Staphylococcus. While penicillin was effective initially, overuse led to bacterial resistance. By 1959, methicillin, a penicillin derivative, offered a new solution, but resistance emerged again by 1961, giving rise to methicillin-resistant Staphylococcus aureus (MRSA). This strain prompted changes in infection control practices, yet MRSA remains a significant threat today [source: Orent].
MRSA is often regarded as the most daunting form of staph infection due to its resistance, but it’s not the only one. Staph bacteria can thrive on both people and objects unnoticed, with many individuals carrying the bacteria without developing infections. Over 30 types of staph bacteria exist, leading to a wide range of symptoms we’ll explore later. The most prevalent type, Staphylococcus aureus, can cause skin infections like cellulitis, impetigo, and boils, as well as systemic conditions such as toxic shock syndrome and food poisoning. Without proper treatment, staph infections can lead to severe illness or even death.
Until the 1990s, staph infections were primarily associated with hospitals [source: Borlaug]. However, as we’ll discuss in the next section, they have since spread beyond healthcare settings.
Causes of Staph Infections
Staph bacteria can survive in nearly any environment, making the routes to infection numerous. It can thrive in poorly sanitized medical tools, hot climates, salty foods, and even withstand high cooking temperatures. Food poisoning occurs when contaminated food is consumed, often due to improper handling by a staph carrier or prolonged exposure at unsafe temperatures.
Staph bacteria infect the body similarly to other infections, typically entering through open wounds. Once inside, they can spread to the bloodstream, causing blood poisoning, or the digestive system, leading to food poisoning—even in healthy individuals. The resulting infection can vary from minor skin issues like boils to life-threatening conditions such as heart failure, depending on the entry point and spread within the body. We’ll delve deeper into symptoms in the next section.
Hospitals are a common breeding ground for staph bacteria. With patients entering and exiting with various wounds and compromised immune systems, and the frequent use of invasive devices like feeding tubes, catheters, or dialysis, the bacteria find ample opportunities to invade through open wounds. Poor hygiene practices, such as inadequate handwashing and unsterilized surfaces, can facilitate the spread of staph in hospitals, especially since carriers may not even realize they have the bacteria.
Staph infections can also spread through direct skin contact, making group living environments like dormitories particularly vulnerable. Similarly, contact sports such as football and wrestling are notorious for staph transmission. For instance, between 2005 and 2008, six Cleveland Browns players contracted staph infections. Even high-profile athletes like Peyton Manning and Tom Brady were affected in 2008 [source: Gregory].
A low white blood cell count increases susceptibility to infections, including staph. Since white blood cells are crucial for fighting infections, a reduced count makes it easier for staph to invade the body.
While anyone can be at risk for staph infections, the experience of having one varies. We’ll explore what it’s like to contract a staph infection in the next section.
Symptoms of Staph Infections
Given the diverse forms of staph bacteria, it’s no wonder they can trigger a broad spectrum of health issues. While skin infections are the most commonly linked to staph, these bacteria can also lead to a variety of other complications.
Skin infections caused by staph can vary from mildly irritating to severely painful. Boils, the most frequent symptom, are characterized by pus-filled pockets in hair follicles that eventually rupture, releasing pus and blood. Infants and young children often experience impetigo and scalded skin syndrome, both accompanied by rashes, with impetigo also causing blisters near the mouth. In older individuals, staph infections may present as cellulitis, leading to redness and itching on the legs [source: Hirch].
Staph-induced food poisoning strikes rapidly and typically lasts one to two days. Symptoms include cramps, vomiting, and diarrhea, and it occurs when staph bacteria are transferred to food or hands through skin contact, coughing, or sneezing.
Toxic shock syndrome, often associated with specific tampon use, results in fever, vomiting, confusion, seizures, headaches, and rashes. It is thought to arise from fibers irritating the skin or superabsorbent tampons being left in too long, creating an environment for bacterial growth. Without treatment, it can progress to kidney failure and potentially death [source: Mayo Clinic].
Blood poisoning, or bacteremia, occurs when staph bacteria enter the bloodstream, causing high fever. These infections can also affect organs such as the heart and lungs.
Septic arthritis is another serious condition caused by staph bacteria. In this case, the bacteria invade the joints, leading to swelling, pain, fever, and chills. Like other staph infections, it typically occurs when an open wound is exposed to the bacteria.
MRSA, as previously mentioned, acts similarly to other staph infections but stands out due to its resistance to antibiotics. Its symptoms mirror common skin infections, including cellulitis, boils, abscesses, carbuncles, and impetigo.
Due to the staph bacteria's ability to mutate and adapt, antibiotics are not always effective in treatment. As we’ll explore in the next section, managing the infection is possible, but preventing its spread is the most effective strategy.
Antibiotics are effective only against bacterial infections and have no impact on infections caused by viruses.
Treatment and Prevention of Staph Infections
Staph infections present a unique challenge because the very treatments used against them have contributed to their resilience. Overuse of antibiotics has allowed the bacteria to adapt, creating superbugs like MRSA. If you suspect a staph infection, seek medical attention immediately.
During your visit to the doctor, a tissue or nasal secretion sample will be taken to determine if your infection is caused by staph bacteria.
If the doctor identifies staph as the culprit, they will assess whether antibiotics are needed. As previously noted, many staph strains resist common antibiotics such as penicillin and methicillin. For skin infections, the doctor may drain the affected area before considering antibiotics, which helps clear the infection even if bacteria remain.
The most effective approach to staph infections is prevention. Simple hygiene practices, reminiscent of advice from your grandmother, can go a long way:
- Isolation. In hospitals, infected patients may be isolated, and healthcare workers may wear protective gear to prevent the spread of staph.
- Avoid sharing personal items. Remind teens and athletes not to share towels or athletic gear to minimize the risk of transmission.
- Cover wounds. Keep any infected areas covered with sterile bandages, as staph bacteria thrive in pus.
- Wash hands frequently. Scrub your hands with warm water and soap for at least 30 seconds. Humming "Row, Row, Row Your Boat" twice can help time it. Use hand sanitizer when soap and water aren’t available.
- Change tampons regularly. Replace tampons every four to eight hours to reduce the risk of toxic shock syndrome.
- Avoid touching your nose. Since staph bacteria are commonly found around the nose and mouth, keep your hands away from these areas.
[source: CDC]
For more detailed information on staph infections, proceed to the next page.
