 Getty ImagesIn the U.S., antidepressants are some of the most commonly prescribed drugs. Discover more images of medications.
Getty ImagesIn the U.S., antidepressants are some of the most commonly prescribed drugs. Discover more images of medications.Antidepressants serve as the primary treatment for depression, with annual sales reaching around $50 billion, positioning them as one of the top prescription drug categories. Pharmaceutical companies often market antidepressants directly to consumers via television and print ads, significantly influencing healthcare providers' prescribing habits. Despite their widespread use, many questions remain: What exactly are antidepressants? How do they function? And are they truly effective?
This article delves into depression, explores various forms of antidepressant treatments, explains their mechanisms, and evaluates their efficacy and potential side effects. To grasp how antidepressants operate, it’s essential to first understand depression itself.
Major Depressive Disorder (MDD), also known as unipolar depression or clinical depression, impacts approximately 15 million Americans annually. While it can manifest at any age, even in children as young as 5, it predominantly affects individuals aged 25 to 44. MDD is reported in about 20% of women and 10% of men [source: HealthyPlace.com]. This condition not only reduces productivity in work and educational settings but is also a major contributor to suicide rates.
Unlike temporary feelings of sadness, MDD represents a prolonged mood shift that disrupts family life, relationships, and self-esteem. Episodes can persist for days, months, or even years, accompanied by both physical and psychological symptoms, including:
Depressed mood (sadness)Medical DisclaimerThis article is intended for information purposes only and not as medical advice. Those seeking medical advice regarding the diagnosis and treatment of depression should consult with your primary care provider and/or pharmacist.- Loss of interest or pleasure
- Disruptions of sleep patterns
- Fatigue
- Feelings of worthlessness, discouragement, hopelessness and helplessness
- Changes in appetite, weight loss or gain
- Loss of sexual interest
- Inability to think, concentrate or make decisions
A clinical diagnosis of MDD requires that these symptoms persist consistently for at least two weeks.
Learn More
|
These symptoms might overlap with those of other conditions, such as hypertension, diabetes, heart disease, and epilepsy. This overlap suggests that a depressive episode could be a secondary symptom of another illness. Since no lab test exists for depression, physicians often conduct multiple tests to eliminate other potential diseases. If all other possibilities are excluded, the diagnosis points to MDD.
On the following page, we'll explore the underlying causes of depression.
Causes of Depression
The precise cause of MDD remains unclear, but studies emphasize the role of chemical imbalances in neurotransmitters, particularly serotonin, norepinephrine (also known as noradrenaline), and dopamine. These neurotransmitters, especially serotonin, are highly concentrated in brain regions like the limbic system and upper brainstem, which regulate mood and emotions. For further details, refer to How Your Brain Works.
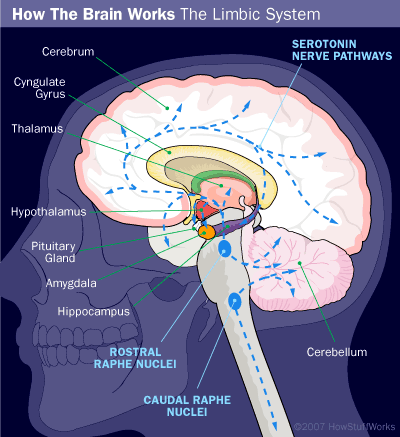
Studies show that individuals with MDD either have insufficient serotonin or norepinephrine in specific brain regions or experience an imbalance between these neurotransmitters. Antidepressants aim to boost the levels of these chemicals in the limbic system. To comprehend how antidepressants function, it’s essential to explore the concept of neurotransmission.
Note Many addictive drugs (like cocaine, methamphetamines, LSD, heroin and
marijuana) affect the same pathways and neurotransmitters as MDD does. |
The brain and nervous system consist of nerve cells, or neurons. Similar to the wiring in a home’s electrical setup, neurons connect through circuits known as neural pathways. However, unlike household wires, neurons don’t physically touch. Instead, they come close at junctions called synapses, where a small gap, the synaptic cleft, separates them. The transmitting neuron is referred to as the presynaptic cell, while the receiving neuron is the postsynaptic cell. Neurons communicate by sending chemical messengers, or neurotransmitters, across the synapse in one direction.

Next, we’ll examine this process using serotonin as an example.
Nerve Communication
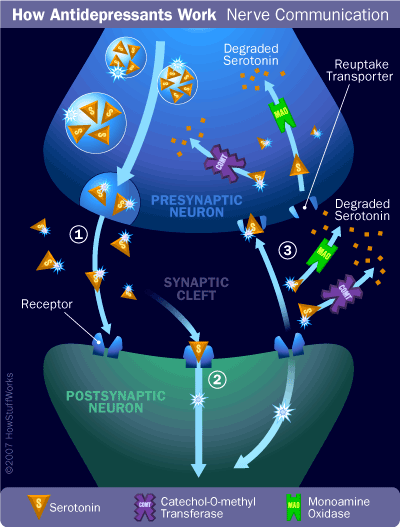
- The presynaptic cell (sender) produces serotonin (5-hydroxytryptamine, 5HT) from the amino acid tryptophan and stores it in vesicles at its terminals.
- An electrochemical signal travels through the presynaptic cell to its terminals.
- The signal triggers the vesicles to merge with the cell membrane, releasing serotonin into the synaptic cleft.
- Serotonin crosses the cleft, binds to receptors on the postsynaptic cell (receiver), and initiates a new electrochemical signal (which can either activate or inhibit the cell). Serotonin and its receptor interact like a lock and key.
- Excess serotonin in the cleft and receptors is broken down by enzymes (MAO and COMT). Some serotonin is reabsorbed by the presynaptic cell via reuptake transporters, where it is also degraded by MAO and COMT, effectively turning the signal "off."
A comparable process occurs with norepinephrine, which also influences mood, emotions, and MDD. Serotonin, norepinephrine, and dopamine are chemically alike and belong to the monoamine neurotransmitter class. Their structural similarity allows them to be recognized and broken down by the enzymes MAO and COMT.
Next, we’ll explore how antidepressants function.
SSRI and Tricyclic Antidepressants
 Getty ImagesProzac ranks among the most widely prescribed antidepressants.
Getty ImagesProzac ranks among the most widely prescribed antidepressants.Antidepressants work by targeting specific stages of synaptic transmission in neurons that contain serotonin, norepinephrine, and dopamine within the brain. This action boosts the levels of these neurotransmitters, helping to stabilize mood and emotions, potentially restoring them to normal. However, since neurotransmitters like norepinephrine are also present in neural pathways outside the mood-regulating areas, some antidepressants may cause side effects such as changes in blood pressure or saliva production. Additionally, because MDD-related pathways are located in the lower brain and brainstem, antidepressants can impact other functions like appetite, sleep, and sexual activity.
Antidepressants are categorized based on the neurotransmitters they influence and their mechanisms of action. Let’s explore the various types of antidepressants.
Selective Serotonin Reuptake Inhibitors (SSRI)SSRIs, the most commonly prescribed antidepressants, emerged in the mid-1980s. They function by preventing serotonin from being reabsorbed into the presynaptic cell, thereby raising serotonin levels in the synaptic cleft and enhancing postsynaptic cell stimulation. Common SSRIs include:
- fluoxetine (Prozac)
- paroxetine (Paxil)
- sertraline (Zoloft)
- fluvoxamine (Luvox)
- citalopram (Celexa)
- escitalopram (Lexapro)
All SSRIs are equally effective and generally well-tolerated, though individual responses vary. Some patients may experience more side effects with certain SSRIs than others. Most SSRIs require multiple doses daily, but fluoxetine, with its longer half-life, allows for once-daily dosing, reducing the risk of missed doses. At higher doses, paroxetine and sertraline can affect both dopamine and serotonin neurotransmission.
To reduce side effects that might lead to discontinuation, healthcare providers typically start SSRIs at low doses, gradually increasing to the target dose over four to six weeks. Common side effects include nausea, dizziness, vertigo, vomiting, insomnia, loss of appetite, anxiety, and sexual dysfunction.
Tricyclic Antidepressants and Selective Norepinephrine Reuptake InhibitorsTricyclic antidepressants, introduced in the late 1950s and early 1960s, work similarly to SSRIs by blocking norepinephrine reuptake, increasing its presence in the synaptic cleft. Examples of tricyclic antidepressants include:
- nortryptiline (Pamelor)
- maprotiline (Ludiomil)
- desipramine (Norpramine)
- amitryptiline (Elavil)
- clomipramine (Anafranil)
- imipramine (Trofranil)
Tricyclic antidepressants influence heart rate and blood pressure since norepinephrine is also involved in autonomic nerve functions. Side effects include postural hypotension (a sudden drop in blood pressure when standing), tachycardia (fast heart rate), dry mouth, urinary retention, and blurry vision. Due to their toxicity and overdose risk, tricyclics are less commonly prescribed. However, they remain effective for patients who cannot tolerate SSRIs or other antidepressants, requiring close medical supervision to manage potential toxic effects.
Tricyclic antidepressants are nonselective in inhibiting norepinephrine reuptake because their chemical structure resembles norepinephrine. Reboxetine (Edronax) is a more targeted reuptake inhibitor, binding more effectively to the transporter, but it is not available in the United States.
SNRI, MAOI and NaSSA Antidepressants
Serotonin-Norepinephrine Reuptake Inhibitors (SNRI)Introduced in the mid-1990s, SNRIs prevent the reabsorption of both serotonin and norepinephrine by binding to their transporters on the presynaptic cell. Examples of SNRIs include:
- bupropion (Wellbutrin) -- also inhibits dopamine and norepinephrine reuptake
- duloxetine (Cymbalta)
- venlafaxine (Effexor)
These medications have side effects similar to SSRIs but are generally milder. Bupropion and duloxetine, in particular, are associated with fewer issues related to sexual dysfunction and weight gain.
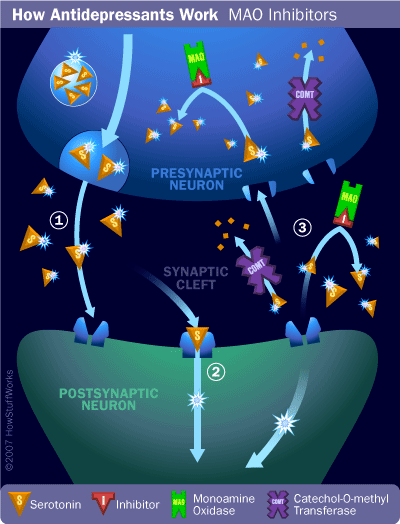
Monoamine Oxidase Inhibitors (MAOI)Monoamine oxidase, an enzyme, can break down serotonin and norepinephrine in the synaptic cleft and presynaptic cell. MAOIs prevent this breakdown, increasing neurotransmitter levels. Examples of MAOIs include:
- phenelzine (Nardil)
- tranylcypromine (Parnate)
- selegiline (Eldepryl)
- isocarboxazid (Marplan)
- moclebemice (Manerix)
Since these medications can affect norepinephrine, they may lead to cardiovascular side effects. Patients are often advised to avoid foods high in tyramine, as the interaction between the drugs and tyramine can cause hypertension (elevated blood pressure). Tyramine-rich foods include soy sauce, sauerkraut, chicken and beef livers, aged cheeses, sausages, cured meats and fish, yogurt, raisins, figs, and sour cream. Additionally, patients must avoid alcohol while taking these antidepressants. Due to these potential interactions, MAOIs are less commonly prescribed compared to other antidepressant classes.
Noradrenergic and Specific Serotonin Antidepressants (NaSSA)Some NaSSAs were introduced in the mid-1980s, with others being more recent. These drugs inhibit the negative feedback mechanisms that regulate norepinephrine and serotonin release from the presynaptic cell, thereby increasing their levels in the synaptic cleft. They also block certain serotonin receptors on the postsynaptic cell, enhancing serotonin neurotransmission. Examples of NaSSAs include:
- Mirtazipine (Remeron)
- Trazodone (Desyrel)
- Nefazodone (Serzone)
- Mianserin (Bolvidion)
Common side effects include drowsiness, dry mouth, increased appetite, and weight gain. It’s important to note that all available antidepressants are similarly effective in treating MDD. The choice of medication depends on factors like the patient’s age, family history, tolerance, side effects, and previous responses to antidepressants.
On the next page, we’ll explore the role of antidepressants in treating MDD.
Depression Treatment
MDD has no cure, so treatment focuses on alleviating symptoms, enhancing quality of life, and reducing suicide risks. Effective management typically involves a combination of psychotherapy, medication, and patient education. MDD treatment is divided into three phases: acute, continuation, and maintenance [source: Mann].
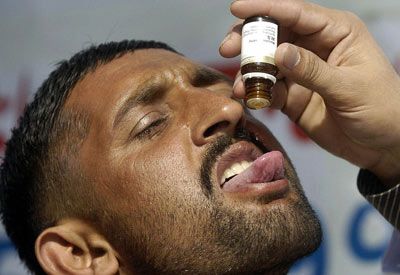 Getty ImagesA survivor of the 2005 Kashmir earthquake receives antidepressant medication at a healthcare facility.
Getty ImagesA survivor of the 2005 Kashmir earthquake receives antidepressant medication at a healthcare facility.Acute phaseThe primary objective is to achieve remission, where symptoms are significantly reduced. This phase typically starts with antidepressant treatment, often SSRIs, due to their lower dosage requirements and fewer side effects, making them suitable for children and elderly patients. It generally takes four to six weeks for antidepressants to take effect.
Augmenting Antidepressants Sometimes
MDD patients show other symptoms (changes in mood, delusions,
hallucinations, changes in energy metabolism) partially due to
antidepressant side effects or to other types of depression (like
bipolar disorder -- periods of happiness interspersed by periods of
severe depression). So, primary care providers may add other
medications to antidepressant therapy.
|
Initially, the physician and patient assess the severity of symptoms to set a baseline. Over the first four to six weeks of treatment, patients may engage in psychotherapy and be monitored for side effects. The physician then reevaluates symptom severity against the baseline. If symptoms improve by less than 25% after eight weeks, the current antidepressant is deemed ineffective. The doctor may adjust the dosage, switch medication classes, or combine antidepressants. If effective, the acute phase typically lasts six to 10 weeks.
Continuation phaseOnce remission is achieved, the focus shifts to eliminating residual symptoms, restoring pre-MDD functionality, and preventing relapse. During this phase, the same levels of antidepressant therapy and psychotherapy are maintained. If no relapse occurs after six months, medication may be gradually tapered off. This phase can last six to 12 months.
Maintenance phaseThis phase is crucial for patients with recurring depressive episodes. Regular monitoring is essential, and antidepressant therapy may need to be restarted. Psychotherapy and patient education play a key role. The maintenance phase can extend from one to three years.
Special populations and depression therapyCertain clinically depressed patients require tailored treatment approaches, taking into account their unique needs and circumstances.
- Bipolar disorder -- Patients experience severe mood swings, alternating between extreme highs and deep depressive lows. Treatment often combines antidepressants with mood stabilizers.
- Children/adolescents -- Fluoxetine, an SSRI, is the only approved antidepressant for this age group. Concerns have been raised about increased suicide risk in children on antidepressants, though conclusive evidence is lacking. Doctors must balance the risks of treatment against those of untreated depression, as untreated depression often poses a greater suicide risk.
- Pregnant/postpartum women -- Depression is common during pregnancy and postpartum, often resolving on its own. However, severe cases (about 10%) require treatment. Antidepressants can affect the fetus and pass into breast milk, with unknown long-term effects. Physicians must carefully weigh the risks and benefits of treatment.
Depression treatment is a long-term commitment aimed at achieving remission and maintaining stability. Combining medication, psychotherapy, and patient education yields the best results. Close collaboration with a physician or psychiatrist ensures optimal treatment strategies.
Next, we’ll explore how direct-to-consumer marketing by pharmaceutical companies has significantly influenced patient choices in recent years.
Direct-to-Consumer Advertising
Saint-John's Wort Saint-John’s-wort
is an herb that has been used since ancient times for treating
depression. It is available over the counter without a prescription,
but its clinical effectiveness for treating depression has been
controversial. Studies in Europe
have indicated that it is about as good as tricyclic antidepressants in
treating mild depression. However, studies in the United States have
indicated that this herbal supplement is not effective and should not
be used for treating severe depression. Because Saint-John’s-wort is an
herb, it is not governed by the FDA, but studies have shown that it
interferes with Âliver enzymes that are critical for the metabolism and actions of other drugs (like HIV medications, cyclosporine and oral contraceptives). Therefore, the FDA has warned consumers not to take Saint-John’s-wort when taking other medications. |
Historically, pharmaceutical companies communicated only with healthcare providers, a process known as physician detailing. In 1996, the FDA eased restrictions on direct-to-consumer advertising for prescription drugs, a practice permitted only in the United States and New Zealand. Advocates argue that such ads educate patients about conditions and treatments, improving doctor-patient communication. Today, ads for prescription drugs, including antidepressants, are common in print and on television [source: Frosch]. Consumers are exposed to up to 16 hours of these ads annually. Spending on DTCA surged from $11 billion in 1996 to $30 billion in 2005.
 James Keyser/Time & Life Pictures/Getty Images
James Keyser/Time & Life Pictures/Getty ImagesDirect-to-consumer advertising (DTCA) has sparked debate. While pharmaceutical companies argue it educates patients, critics contend that:
- Patients gain insufficient knowledge, especially from brief TV ads.
- Doctors, pressured by patient requests, often prescribe costly brand-name drugs over generics or alternative treatments.
- The FDA has not strictly regulated the accuracy of prescription drug ads, particularly in television commercials.
This leads to increased healthcare costs without a corresponding improvement in patient care quality.
A study involved actors simulating MDD symptoms to visit over 150 healthcare providers in Sacramento, San Francisco, and Rochester [source: Kravitz et al]. In some visits, actors requested specific antidepressants, while in others, they made no brand requests. Researchers found that doctors were more inclined to prescribe brand-name drugs when patients requested them or mentioned antidepressants in general, compared to when no requests were made. This suggests that patient requests significantly influence prescribing habits for antidepressants. However, another study indicated that physician detailing had a greater impact on brand-name prescriptions than DTCA [source: Donohue et al], keeping the debate over DTCA's influence unresolved.
