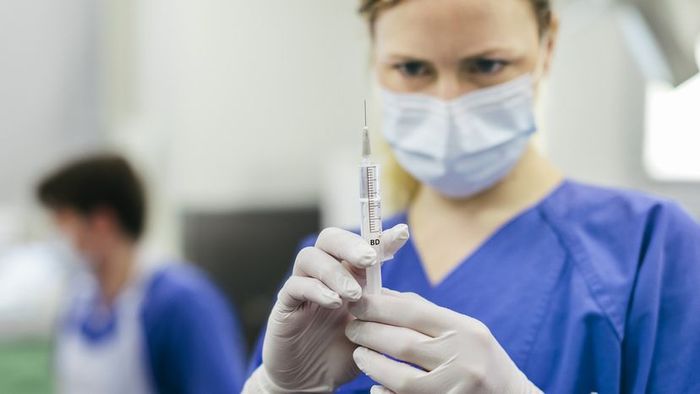
 A nurse preparing a syringe for administering local anesthesia. Hinterhaus Productions / Getty Images
A nurse preparing a syringe for administering local anesthesia. Hinterhaus Productions / Getty ImagesFor many, anesthesia remains an enigmatic concept, even for those who have experienced it. Derived from the Greek words meaning "loss of sensation," its effects extend beyond mere numbness. Anesthesia, induced by medications to create a temporary state, aims to achieve several outcomes: alleviating pain, erasing memories of invasive procedures, reducing anxiety (a common reaction to medical interventions), and immobilizing muscles.
While the idea of anesthesia might seem intimidating, its safety is ensured through precise dosage calculations and constant supervision by healthcare experts. Not all anesthesia is the same, and this article delves into its various forms, explaining how it functions, its mechanisms, and associated risks. Additionally, we’ll explore the phenomenon of anesthesia awareness and trace its historical roots, including its surprising connection to cocaine.
3 Types of Anesthesia
The type of anesthesia administered depends on various factors, such as the nature of the medical procedure and your health background. Sometimes, a combination of drugs is required to achieve the desired outcomes, and there can be overlaps between different anesthesia types.
- General anesthesia: This is the most well-known form, rendering patients completely unconscious during major surgeries or complex procedures.
- Conscious sedation: Often used for minor treatments, this method uses lighter doses of anesthetics to keep patients awake but calm and free from discomfort, with faster recovery times and fewer complications.
- Regional anesthesia: Techniques like epidurals and spinal blocks fall under this category, targeting larger body regions and requiring careful monitoring due to their impact on the central nervous system.
- Local anesthesia: This mildest form numbs a specific, small area of the body, typically through injections or topical applications like lidocaine, lasting a few hours with minimal side effects.
Continue reading to explore more about the various anesthetic drugs and their applications.
General Anesthesia
General anesthesia induces a state of complete unconsciousness and immobility, often described as being 'put under.' Once the drugs take effect, you enter a deep sleep-like state, unaware of sensations, pain, or any events occurring during the procedure.
For almost two centuries, the mechanism behind general anesthesia remained a mystery. However, a 2019 study revealed that anesthetic drugs interact with a brain region responsible for regulating various bodily functions, including sleep.
When Is General Anesthesia Required?
General anesthesia is typically used for major, time-consuming surgeries. Procedures like a knee replacement may require a few hours under anesthesia, while more complex operations, such as heart bypass surgery, can extend to six hours or more.
Key Considerations Before Undergoing Anesthesia
Before undergoing surgery with general anesthesia, you’ll usually consult with an anesthesiologist to provide your medical history. This includes details about existing health conditions, prescription medications (even those not used for pain), herbal supplements, and over-the-counter drugs you might be taking.
This step is crucial because certain medical conditions may necessitate special precautions during anesthesia. For instance, patients with low blood pressure might require ephedrine. Additionally, individuals who consume alcohol heavily or use drugs may respond differently to anesthesia. During the consultation, you’ll be advised to avoid eating for several hours before the procedure to prevent the risk of aspiration under anesthesia.
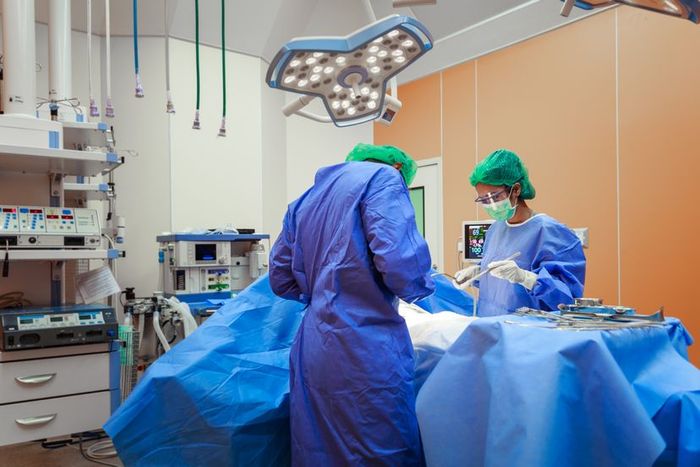 Doctors and anesthesiologists maintain close supervision of patients under general anesthesia, monitoring vital signs and brain activity throughout the procedure.
TwilightShow / Getty Images
Doctors and anesthesiologists maintain close supervision of patients under general anesthesia, monitoring vital signs and brain activity throughout the procedure.
TwilightShow / Getty ImagesMonitoring Patients Under General Anesthesia
Under general anesthesia, a breathing mask or tube is essential because the muscles relax to the point where they can’t keep the airways open. Multiple vital signs are monitored continuously, including blood oxygen levels, heart rate, blood pressure, breathing rate, carbon dioxide levels, body temperature, anesthetic concentration, and brain activity. An alarm system is in place to alert medical staff if oxygen levels fall too low.
The 4 Stages of General Anesthesia
- The first stage, induction, involves administering medication. Patients may begin to feel its effects but remain conscious.
- In the second stage, excitement, patients may experience twitching, irregular breathing, or heart rate fluctuations. Despite these signs, they remain unconscious and have no memory of this phase, which quickly transitions to the next stage.
- Stage three is characterized by muscle relaxation, regular breathing, and full anesthesia.
- Stage four is an abnormal phase caused by drug overdose, potentially leading to cardiac or respiratory arrest, brain damage, or death if not addressed immediately.
Anesthesia Awareness
Anesthesia awareness occurs when patients regain some level of consciousness during surgery and can recall events, such as feeling pain, pressure, or being aware of their surroundings. This rare phenomenon can result from insufficient drug administration, inadequate monitoring, or equipment malfunction during the procedure.
In the most severe instances, patients have described being fully paralyzed yet experiencing the full pain of their surgery, leading to significant emotional distress. Although anesthesia awareness is a terrifying concept, it is considered extremely rare, occurring in only one or two out of 1,000 surgeries, and should not deter individuals from undergoing necessary procedures [source: Mayo Clinic].
Conscious Sedation, aka Twilight Anesthesia
Conscious sedation, often referred to as twilight anesthesia, is a form of anesthesia you might have experienced without realizing it. For instance, if you’ve had your wisdom teeth removed, you’ve likely undergone this type of sedation, as it’s commonly used for brief, less invasive procedures. Beyond dental work, it’s also employed for tasks like setting fractures, LASIK surgery, and minor cosmetic operations.
During conscious sedation, you remain awake and able to respond to questions or instructions, though you may feel drowsy and relaxed. Most patients don’t recall the procedure or the immediate aftermath. Some medications used in this process can induce feelings of euphoria or giddiness. While higher doses can cause sleep, paralysis, and cardiovascular effects, lower doses are used to relax patients and alleviate anxiety.
 A doctor holds a mask to administer anesthesia in gaseous form.
Jupiterimages / Getty Images
A doctor holds a mask to administer anesthesia in gaseous form.
Jupiterimages / Getty ImagesConscious Sedation vs. General Anesthesia
Conscious sedation shares many similarities with general anesthesia, as it employs the same types of drugs but in significantly lower doses. Typically, sedatives like ketamine or nitrous oxide are used to suppress the central nervous system. Alternatively, dissociative drugs such as diazepam (Valium) or midazolam may be administered to block nerve signals from reaching the brain.
For conscious sedation, an anesthesiologist often combines sedatives with pain-relieving analgesics like fentanyl. These drugs can be inhaled, taken orally, injected, or used in combination. For instance, a patient might inhale nitrous oxide while a certified registered nurse anesthetist (CRNA) administers ketamine or Valium intravenously.
How Long Does Conscious Sedation Last?
The duration of conscious sedation varies based on the drugs used, ranging from as little as five to 10 minutes to up to an hour. Recovery is typically quick, and side effects like nausea, vomiting, or dizziness, commonly associated with general anesthesia, are rare but possible. Patients must still be closely monitored to prevent unintended deeper sedation.
Regional Anesthesia
The terms "local anesthesia" and "regional anesthesia" are sometimes used interchangeably. In this context, "regional anesthesia" refers to anesthesia applied to a broader area of the body.
Regional Anesthetic Types and Techniques
While local anesthesia numbs a small area, regional anesthesia can numb an entire limb. This is called peripheral regional anesthesia, as it targets a single nerve or a specific nerve group. Central regional anesthesia, on the other hand, involves injections into the cerebrospinal fluid or the epidural space near the spinal canal.
Regional anesthesia, often referred to as a nerve block, involves higher doses of the same drugs used in local anesthesia, producing a more pronounced effect on the central nervous system. Patients may stay awake during procedures under regional anesthesia, though sedation can be provided during the block administration, the procedure itself, or both, depending on the patient’s preference and the nature of the surgery.
Many women who have experienced birth are likely familiar with epidurals, a central anesthetic technique. During this procedure, an anesthesiologist places a catheter into the epidural space, usually in the lower back, to deliver medications like lidocaine or clonidine. This results in pain relief and numbness from the waist down.
Spinal blocks, injected into the cerebrospinal fluid, are commonly used for procedures below the waist, such as Cesarean sections or hernia repairs. They often cause more extensive paralysis than epidurals. While patients typically remain awake during C-sections with spinal blocks, sedation may be used for other surgeries.
Administration and Monitoring
Regional anesthetics can be administered through a single injection, intravenously, or continuously via a catheter. One method, known as a Bier block, involves using a tourniquet to restrict blood flow to a limb before injecting the drug into a vein. This technique is suitable only for shorter procedures.
Due to the heightened engagement of the central nervous system, patients undergoing regional anesthesia require close observation as it poses greater risks, including seizures and heart attacks, compared to local anesthetics. In cases where regional anesthesia does not adequately alleviate pain or induce paralysis, a transition to general anesthesia may be essential.
Local Anesthesia
You've probably encountered this type of anesthesia in the past. For instance, dentists often administer a local anesthetic alongside procedural sedation for extensive dental procedures. By injecting the gum, they numb a specific area. Local anesthesia renders a tiny section of the body, like a small skin area, unresponsive to pain. It achieves both pain relief and paralysis by interrupting nerve signals, preventing them from reaching the brain, though patients might still sense pressure and touch.
 Before commencing a dental procedure, a dentist will administer a local anesthetic injection into your gum to desensitize the area.
Drs Producoes / Getty Images
Before commencing a dental procedure, a dentist will administer a local anesthetic injection into your gum to desensitize the area.
Drs Producoes / Getty ImagesHistorical and Contemporary Use of Local Anesthetics
Local anesthetics can be applied topically, targeting only the surface area. These often come in the form of gels, creams, or sprays. They are frequently used on the skin prior to injecting a deeper-acting local anesthetic to minimize discomfort from the needle or the medication itself, such as penicillin, which can cause pain during injection.
Topical anesthetics have applications beyond medical settings — if you've ever applied a pain-relieving product for conditions like rashes or hemorrhoids, you've experienced their effects. Local anesthetic drugs typically end with the suffix "-aine" (e.g., lidocaine, novocaine, or tetracaine) due to their chemical similarity to cocaine, the first known local anesthetic. However, cocaine's addictive nature and strong cardiovascular stimulation led scientists to create synthetic alternatives.
Some of these synthetic drugs come with their own drawbacks, such as allergic reactions, which have reduced their popularity. This explains why lidocaine has largely replaced novocaine in modern dentistry. Additionally, these drugs act as vasodilators, expanding blood vessels and potentially causing excessive bleeding, though this can be mitigated with the use of epinephrine.
Duration of Local Anesthesia Effects
The effects of local anesthesia typically subside within four to five hours. Often, the pain relief extends beyond the duration of the procedure itself. While side effects are rare, patients should exercise caution in the numbed area — for instance, leaving the dentist with half your face numb could lead to accidentally biting your cheek. Although uncommon, improperly administered local anesthetics can result in nerve damage, but they are generally safe for healthy individuals when used correctly.
Administration, Side Effects and Recovery
How does someone become unconscious under general anesthesia? A Certified Registered Nurse Anesthetist (CRNA) or another anesthesia team member may deliver it through gas, an IV, or a mix of both. Typically, an IV injection is used first to induce unconsciousness, followed by gas to sustain the effect. (Certain injected anesthetics can maintain the desired anesthesia level without gas.) Commonly used gases include isoflurane or desflurane, often combined with nitrous oxide.
Prior to surgery, medications like ketamine, sedatives (e.g., Valium), and depressants such as Sodium Pentothal may be administered through a pre-inserted IV. Additionally, a muscle relaxant might be given to ensure complete paralysis, particularly for surgeries involving major organs.
Post-Surgery
Once the surgery concludes, the administration of anesthetic gases is halted, and the IV anesthetic is stopped. Patients are then transferred to a PACU (post-anesthesia care unit), also known as a recovery room, for close monitoring. To address dehydration caused by anesthesia and shivering from temperature changes, warm IV fluids are often provided. As the pain-relieving effects of the anesthetic fade, pain management measures, such as oral medications or morphine, are administered based on the surgery's intensity. Recovery times vary, with some patients waking within an hour and others taking longer to fully regain consciousness.
Side Effects and Risks
Upon waking, you might experience side effects like nausea, vomiting, and numbness around the surgical site. Disorientation is common, and you may need help moving around during the initial recovery phase.
It's crucial to note that general anesthesia carries significant risks, such as suffocation, allergic reactions, organ failure, stroke, and even death. These potential complications should be thoroughly discussed with your doctor prior to surgery.
Who Administers Anesthesia?
Anesthesia administration isn't always handled by an anesthesiologist — it varies based on the situation and the type of anesthesia required. For instance, if you sustain a deep head injury and the ER doctor needs to numb the area for stitches, they can administer a local anesthetic without involving an anesthesiologist.
An anesthesiologist is essential for procedures requiring regional or general anesthesia. These specialists focus on administering anesthesia, managing pain, and overseeing patient care before, during, and after surgery. Becoming an anesthesiologist involves completing medical school, an internship, and a three-year residency in anesthesiology. They often work with an anesthesia care team (ACT), which includes nurse anesthetists and anesthesiologist assistants.
The Shadowy History of Anesthesia
 A nurse adjusts the flow of anesthetic during a surgical procedure at a London hospital in October 1938.
Felix Man/Picture Post/Getty Images
A nurse adjusts the flow of anesthetic during a surgical procedure at a London hospital in October 1938.
Felix Man/Picture Post/Getty ImagesThe concept of anesthesia, though not always by that name, has existed as long as surgery itself, regardless of how rudimentary. Early anesthetics included soporifics (substances that dull the senses and induce sleep) and narcotics like opium, mandrake, jimsonweed, marijuana, alcohol, and belladonna. While these substances offered varying degrees of pain relief, sedation, or amnesia, their effectiveness was inconsistent. Nonmedical methods such as hypnosis, ice for numbing, and acupuncture were also historically used.
In the mid-1840s, opium and alcohol were the primary anesthetic agents used in industrialized nations. Both substances had significant drawbacks, including addiction and incomplete pain relief. Administering doses strong enough to be effective often risked causing death. In some cases, patients were rendered unconscious by a blow to the head. Without effective anesthesia, surgeries were frequently accompanied by the agonized cries of patients.
A major breakthrough occurred in 1846 when Dr. William Morton, a dentist, demonstrated the use of ether at Massachusetts General Hospital. He removed a tumor from a patient's jaw after using an ether-soaked sponge to induce unconsciousness. The patient reported no memory of the procedure or any pain. Although initially met with skepticism, Morton was eventually celebrated as a pioneer in pain management.
However, Morton wasn't the first to claim the discovery of modern surgical anesthesia. Years after Morton's work was published, Dr. Crawford Long revealed he had used ether in surgeries as early as 1841, inspired by its effects on recreational users. Additionally, Dr. Charles Jackson asserted that his research influenced Morton. Jackson even sought recognition from Congress, supported by Oliver Wendell Holmes, who is credited with coining the term "anesthesia."
Dr. Horace Wells, a dentist, was recognized by the American Medical Association and the American Dental Association as the first to use nitrous oxide for tooth extractions in 1845. Around the same time, Dr. James Simpson introduced chloroform as an anesthetic. Due to its high toxicity, chloroform lost favor, while ether gained prominence in the early 20th century.
Today, a wide range of anesthetics is available, including derivatives of early substances like morphine, "-aine" drugs related to cocaine, and nitrous oxide. Anesthesia continues to advance, becoming safer and enabling life-saving surgeries. The next time you undergo anesthesia, you'll have a deeper appreciation for its history and evolution.
Administering anesthesia requires precise training to determine the correct dosage and type. Factors like body size and health conditions influence the amount needed, as some individuals may not tolerate specific drugs well. Interestingly, even hair color can play a role. Studies in the early 2000s revealed that redheads might experience heightened pain sensitivity but also exhibit greater resistance to both local and general anesthetics.
