While polio has been nearly eradicated globally, a recent case has emerged in the U.S. for the first time in nearly a decade. The infected individual, who was unvaccinated, contracted a strain known as 'vaccine-derived' polio. This term can be confusing, but it’s crucial to understand that it doesn’t imply the polio vaccine should be avoided.
What exactly is polio?
Poliomyelitis is a viral infection that often presents no symptoms or mild flu-like effects in most individuals. However, in rare cases, it can invade the nervous system, leading to paralysis or even fatal outcomes.
Two vaccines were created to combat polio: an injectable version containing inactivated virus in the 1950s, followed by an oral version with a weakened live virus in the 1960s. (These are commonly referred to as the Salk and Sabin vaccines, respectively.) A worldwide effort to eliminate polio began in 1988, and by 2021, only six cases of wild polio infections were reported globally.
Eradicating polio involves vaccinating populations worldwide, particularly in regions where the virus still exists. Since humans are the sole carriers of polio, the strategy is to immunize everyone, leaving the virus without hosts and causing it to disappear. Of the three wild polio types, two have already been eradicated.
How do the vaccines work?
There are two polio vaccines, each used in different regions due to their unique risks and benefits.
The inactivated polio vaccine (IPV) has been the sole polio vaccine used in the U.S. since 2000 and is now part of the standard immunization schedule for infants. It’s the safest option for recipients, as the virus is inactivated and cannot cause illness. Additionally, the vaccine virus cannot spread to others.
The drawback is that even after vaccination, if you contract the polio virus, you may not fall ill but could still transmit it to others.
Given these advantages and disadvantages, this vaccine is most suitable for areas where polio is rare. While it ensures personal protection if polio appears in your vicinity, regions with active outbreaks benefit more from a vaccine that also halts transmission.
The oral polio vaccine (OPV) is utilized in regions where polio remains prevalent. It effectively stops both transmission and infection.
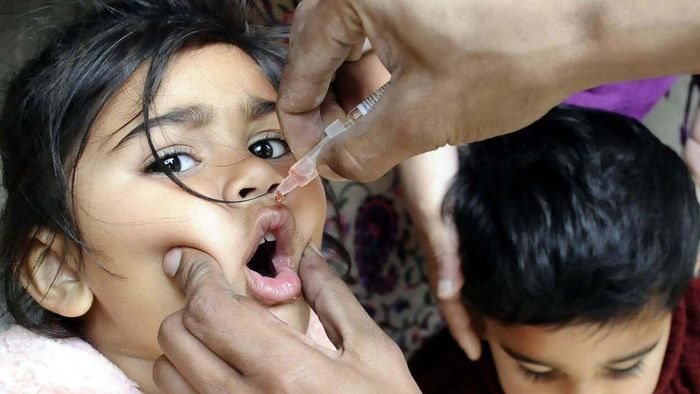
It also offers an added benefit: your body can spread the vaccine virus to others, effectively immunizing them too. This occurs because the vaccine contains a live but weakened virus. Additionally, it’s simple to administer—no need for a trained healthcare professional to give injections. A few drops in a child’s mouth or on a sugar cube are all that’s required.
Since this vaccine uses a live, weakened virus, it poses risks for individuals who are immunocompromised. Its ability to spread also makes it unsuitable for people in their household.
However, OPV carries additional significant risks, which is why it’s not used in areas free of endemic polio. One such risk is that, in extremely rare instances, the vaccine virus can lead to paralysis (known as VAPP, or vaccine-associated paralytic poliomyelitis). This occurs in approximately one case per 2.4 million doses administered, or 0.00004% of the time.
Another rare risk is that the vaccine virus can mutate and regain the ability to cause illness. This is referred to as “vaccine-derived polio.” While vaccinated individuals remain protected, the mutated virus can spread to those who are unvaccinated.
How can you protect yourself from vaccine-derived polio?
The solution is straightforward: Get vaccinated against polio.
Keep in mind, individuals vaccinated against polio are fully protected. Completing the three-dose series of IPV, the vaccine used in the U.S., provides 99% to 100% effectiveness.
You are only at risk of contracting vaccine-derived polio if you are unvaccinated and exposed to the virus. For instance, if you visit a region where OPV is widely used, it’s essential to ensure you’re vaccinated. Even without traveling, you might encounter someone carrying a vaccine-derived polio strain (perhaps from a place where this vaccine is used), who could transmit the virus to you.
This scenario likely explains the recent case reported in New York. The patient, who was unvaccinated, experienced paralysis and was diagnosed with a vaccine-derived polio strain. In response, the Rockland County and New York State health departments released a statement urging vaccination for “unvaccinated individuals, including pregnant women, those who haven’t completed their polio vaccine series, or anyone concerned about potential exposure.”
