1. Gonorrhea
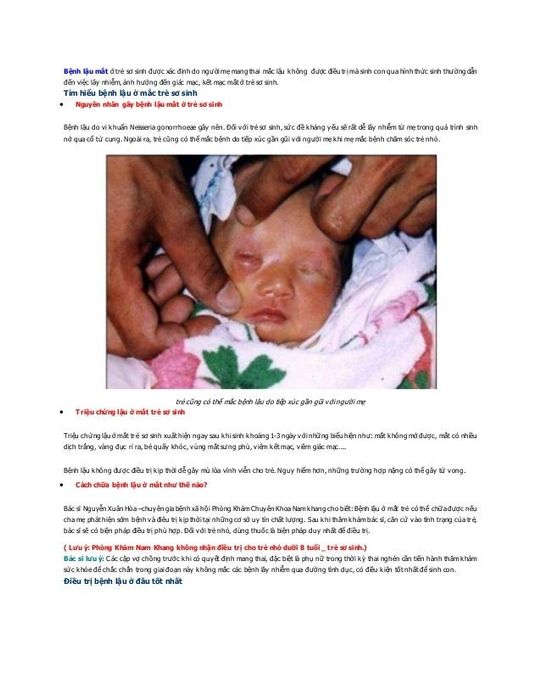
Gonorrhea can be transmitted from mother to child during childbirth. The gonococcal bacteria may infect the infant’s eyes, leading to corneal inflammation and potential corneal ulcers, which, if untreated, can cause blindness. Other complications may include malnutrition, developmental delays, joint infections, blood infections, and meningitis. A mother infected with gonorrhea can pass the bacteria to her child either during delivery or through direct contact with the baby, such as during nursing or cleaning the infant.
Advice: Mothers with gonorrhea should undergo complete treatment before pregnancy. If diagnosed during pregnancy, a cesarean section is recommended to avoid the bacteria spreading to the baby through vaginal fluids, and contact with the baby should be minimized after birth.
2. Group B Streptococcal Infection
Pregnant women carrying Group B Streptococcus in the later stages of pregnancy can pass the infection to their baby.
There are two types of Group B Streptococcal infections in newborns:
- Early onset (24-48 hours after birth): The baby may develop pneumonia, sepsis, or meningitis, especially in preterm infants.
Late onset (after 6 days of age): The baby may develop meningitis or pneumonia.
Advice:
- Mothers should be tested for Group B Streptococcus (via a swab test from the cervix and rectum) during the final stages of pregnancy (35-37 weeks), unless the mother has previously given birth to a baby infected with Group B Streptococcus, in which case the test is not required.
- If the test result is positive, the mother should receive antibiotic treatment during labor, unless a cesarean section is scheduled before labor starts or the water breaks.
- Testing positive and receiving treatment prevents early infection, but continued monitoring of the baby is necessary to detect potential late-onset infection.
3. Herpes
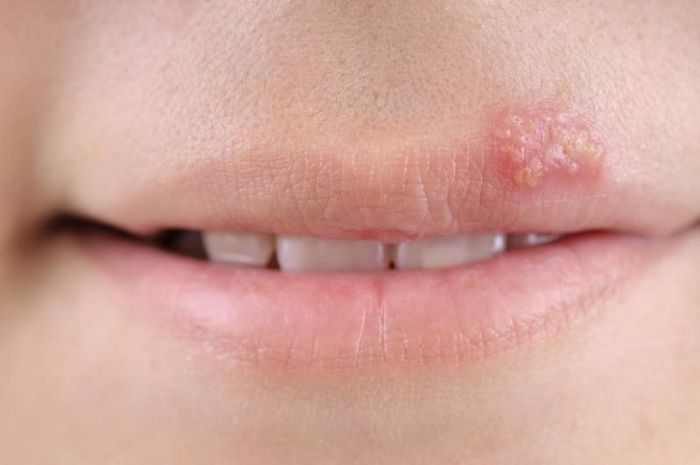
Herpes Virus can be transmitted from mother to child during pregnancy, childbirth, or after birth through contact with amniotic fluid or from fluid discharged from herpes sores (for instance, kissing the baby when the mother has a cold sore can transmit the virus to the infant).
Newborns infected with the herpes virus may show symptoms ranging from mild (cold sores on the lips, genitals, etc.) to severe, with the virus affecting deeper organs like the brain, presenting as symptoms such as constant drowsiness, difficulty breathing, or seizures. Infected infants may also have poor feeding habits and irritability.
Advice:
- A cesarean section may be considered to prevent the baby from coming into contact with genital herpes sores.
- If the mother has a cold sore, she should avoid kissing the baby or allowing the virus to spread to the infant’s clothing or skin.
4. Genital Warts
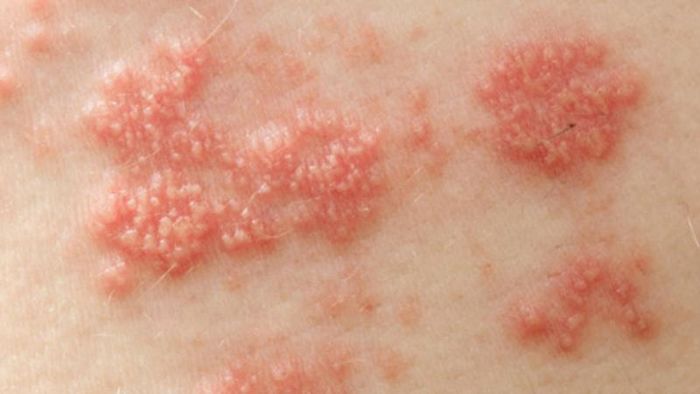
Genital warts can be transmitted from mother to baby either during pregnancy or childbirth, meaning that a cesarean section does not necessarily prevent transmission. A baby may develop warts in the throat, respiratory tract, or genital area, which could disappear on their own or reappear later.
Advice: It is advisable for a pregnant woman to receive complete treatment for genital warts (such as cryotherapy) to prevent rapid spread of the disease. Due to higher estrogen levels during pregnancy, the condition can worsen quickly and pose a risk to the unborn child.
5. Vaginal Fungal Infections
If a mother has a vaginal fungal infection during childbirth, the infection can be passed to the baby, which may result in the baby developing oral thrush, with white patches on the tongue. The infant may also experience discomfort and itching due to the infection.
Advice: To prevent transmission, mothers can use antifungal treatments (such as vaginal suppositories). It is best to consult with a specialized healthcare provider for proper diagnosis and treatment.
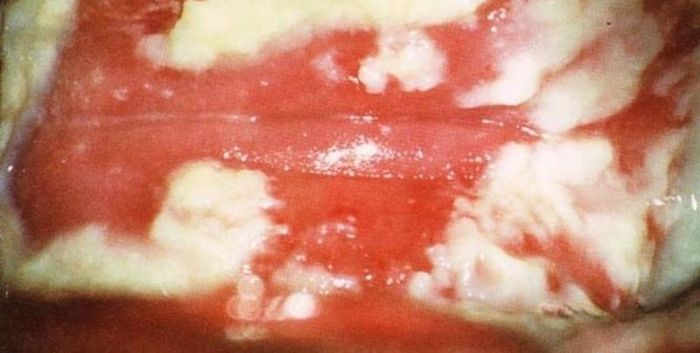
6. Syphilis
If a pregnant woman has syphilis and it is left untreated, the syphilis bacteria can be transmitted from mother to child through the placenta, leading to stillbirth, miscarriage, premature birth, and birth defects in the infant. Infants born with syphilis may show signs such as smaller bones, wrinkled skin, jaundice, bloated abdomen, enlarged liver and spleen, rapid weight loss, or even sudden death.
Syphilis can be passed from mother to baby between the 4th and 5th month of pregnancy, as the placenta allows blood exchange between mother and child during this period. This provides an opportunity for the syphilis bacteria to enter the fetal bloodstream through the umbilical cord.
Advice:
- If a mother suspects syphilis transmission due to sexual activity during pregnancy, she should undergo necessary tests to detect and prevent transmission to the baby.
- If detected early, following a proper treatment regimen prescribed by a doctor can ensure better outcomes for the baby and prevent undesirable consequences.
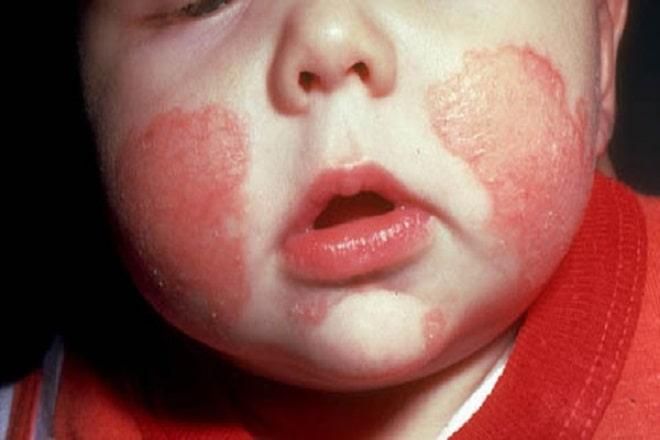
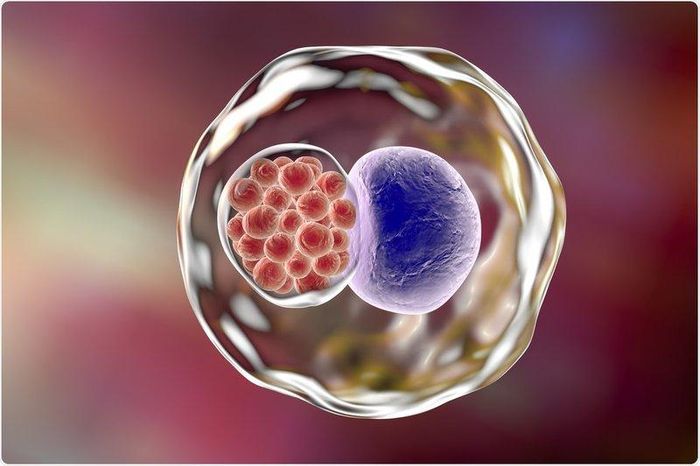
7. Chlamydia Infection
Chlamydia trachomatis is the bacteria responsible for this infection. 60-70% of women may not show noticeable symptoms, but they may experience discomfort during urination, pelvic pain, or unusual bleeding in the genital area. Gonorrhea and chlamydia often occur together.
Due to the subtle symptoms, this infection can cause more severe complications than gonorrhea, as people may underestimate its severity or delay treatment. Chlamydia is also commonly transmitted from mother to child during childbirth, potentially causing eye infections, pneumonia, and ear infections in newborns. Eye infections usually appear about two weeks after birth, but they rarely lead to blindness. However, if left untreated, chlamydia can become chronic, recurrent, and may lead to corneal scarring.
Advice:
- The most reliable way to prevent Chlamydia transmission is by abstaining from sexual activity or maintaining a long-term monogamous relationship with someone who has been tested and is confirmed to be disease-free.
- For men, using condoms correctly and consistently can significantly reduce the risk of Chlamydia transmission.
8. Hepatitis B
Hepatitis B is primarily transmitted from mother to child during pregnancy or childbirth.
Transmission rates from mother to child:
- If the mother contracts the disease in the first trimester, the transmission rate is 1%. In the second trimester, it is 10%, and in the third trimester, the transmission rate is 60-70%.
- The transmission rate also depends on the level of the virus in the mother's body: If the virus is actively growing and reproducing, the rate can range from 50% to 90%. If the virus is dormant, the rate is less than 10%.
Transmission route: The virus is passed from mother to child during labor, whether through vaginal delivery or cesarean section.
Advice for mothers:
For mothers (depending on the severity of the infection):
- If the mother has a mild form and no symptoms, no immediate intervention is needed, and treatment can begin after delivery.
- If the mother has advanced liver disease, cirrhosis, or complications, pregnancy should be avoided. If already pregnant, the mother should get vaccinated against hepatitis B, preferably avoiding vaccination in the first trimester.
- If treatment is required during pregnancy, consult a specialist for guidance.
For the baby:
- To reduce the risk of transmission, the newborn should receive the hepatitis B vaccine within the first 12-24 hours of birth. This gives the baby more than a 95% chance of not contracting hepatitis B later in life. Without the vaccine, the baby faces a higher risk of infection.
- Specifically: If the mother is HBsAg positive (indicating active infection) and HBeAg negative (indicating the virus is dormant), the baby should receive one dose of immunoglobulin and the hepatitis B vaccine immediately after birth, with follow-up doses at 2 and 4 months. If both HBsAg and HBeAg are positive, the baby will receive two doses of immunoglobulin and the hepatitis B vaccine, with follow-up doses at 2 and 4 months as well.
Additionally, mothers infected with the hepatitis B virus can safely breastfeed unless the nipple is cracked or bleeding.

9. HIV/AIDS
In Vietnam, the rate of HIV infection among pregnant women is 0.4%, with around 6,000 babies exposed to HIV each year from a total of 1.5 to 2 million newborns. Without any preventive measures, the transmission rate from mother to child is approximately 36% (ranging from 25-40%).
Transmission routes:
- Transmission during pregnancy via the placenta: This accounts for 20-30% of cases, and the risk increases as the pregnancy progresses, especially in the later stages when the disease advances.
- Transmission during labor: The risk rises to 50-60%, with the likelihood increasing if labor is prolonged, difficult, or if the mother experiences trauma such as tearing or if the baby is distressed. The risk is especially high if the time between the rupture of membranes and delivery exceeds four hours.
- Transmission through breastfeeding: If the mother has cracked nipples or the baby develops mouth ulcers, the virus can be transmitted through breast milk.
Advice:
- Pre-birth intervention: If the mother is HIV positive, routine screening and clinical evaluation should be conducted. Antiretroviral therapy (ARV) should be started and continued until delivery, with continuous monitoring of the disease's progression.
- During labor: Avoid invasive procedures such as artificial rupture of membranes or episiotomy. A cesarean section may be considered, and rapid removal of amniotic fluid is recommended.
- Post-birth intervention: Mothers should be advised to use formula milk instead of breastfeeding. If breastfeeding is necessary, it should only be done in the early months, after which complementary feeding should be introduced.

Rubella is a contagious disease exclusively transmitted by humans, spreading through bodily fluids that carry the virus. Therefore, if a pregnant woman comes into contact with an infected person (typically one week before or two weeks after the onset of symptoms), she risks contracting rubella and passing it on to her baby.
The rubella virus can multiply in the placenta, making it possible for the virus to pass from mother to fetus during pregnancy. The risk of transmission is 90% when the pregnancy is under 12 weeks, 54% between 13 and 14 weeks, 35% between 13 and 16 weeks, 10% after 16 weeks, and insignificant after 20 weeks. This virus slows fetal development, potentially causing severe birth defects such as heart defects, microcephaly, brain damage, cataracts leading to blindness, and more. If the mother contracts the disease in the first trimester, it can lead to miscarriage or stillbirth.
Advice: Women should get vaccinated for rubella at least three months before trying to conceive. If a mother contracts rubella in the first trimester, termination may be recommended due to the high risk of severe birth defects affecting the brain, heart, eyes, ears, and liver.

