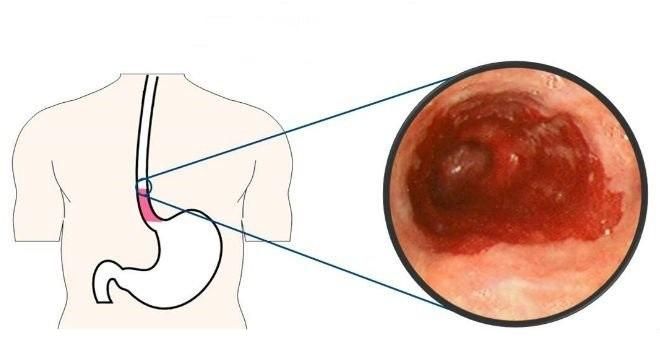
1. Esophageal Ulcers
Esophagitis, also known as esophageal ulcers, can result from bacterial infections, accidental ingestion of acidic substances, or medication overdose causing esophageal damage. Vomiting blood may produce dark red or bright red blood, sometimes mixed with food. Common symptoms include chest pain that worsens with eating or drinking and eases when fasting, along with a sensation of choking while swallowing.
The esophagus connects the throat to the stomach, and esophageal ulcers are a type of digestive system injury. This condition causes pain in the esophageal lining, located between the esophagus and stomach. Patients may experience pain, difficulty eating, weakness, and internal bleeding leading to severe blood loss. Untreated, it can lead to dangerous complications, negatively impacting health and quality of life.
Esophageal ulcers significantly affect health and daily life. Without proper diagnosis and treatment, they can cause severe complications, impairing esophageal function and structure.
When the esophagus is ulcerated, cells and epithelial tissues lose their protective abilities. Without timely treatment, the condition can worsen, leading to stomach ulcers or even esophageal cancer. In some cases, unexplained internal bleeding from esophageal ulcers can cause significant blood loss, weakness, and life-threatening conditions.
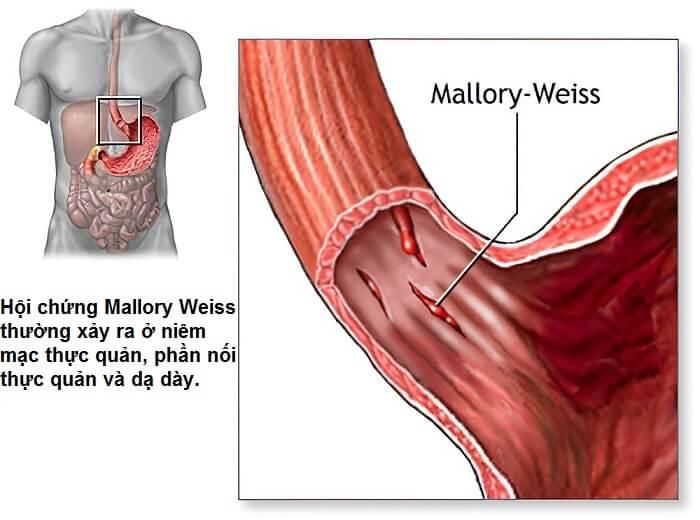
2. Mallory-Weiss Syndrome
Mallory-Weiss Syndrome refers to upper gastrointestinal bleeding caused by tears in the mucous membrane between the esophagus and stomach. This condition often results from excessive alcohol consumption or repeated vomiting, where blood may accompany vomited food. While bleeding from Mallory-Weiss Syndrome can sometimes stop on its own, severe cases may lead to significant blood loss, requiring emergency intervention.
Mallory-Weiss Syndrome involves tears in the esophageal lining, typically occurring at the junction of the esophagus and stomach. These tears are non-contagious and often heal within about 10 days without special treatment. However, complications like uncontrollable bleeding can arise, potentially leading to fatal outcomes if not addressed promptly.
Gastroesophageal tears can cause gastrointestinal bleeding, manifesting as vomiting fresh blood or passing black stools due to sudden abdominal pressure. Typical symptoms include vomiting fresh blood or dark brown fluid after repeated vomiting. Most cases involve mild to moderate bleeding, with severe gastrointestinal hemorrhage being rare. Bleeding usually stops spontaneously without treatment, and recurrence is uncommon. However, some patients may experience significant blood loss, necessitating blood transfusions or leading to shock. There is also a risk of ischemic heart disease, which can cause heart attacks.
Vomiting blood is the most common symptom of Mallory-Weiss tears. Initial vomit may not contain blood, but subsequent episodes may include it. While early vomiting of blood might not directly indicate Mallory-Weiss Syndrome, it can contribute to the formation of tears. Typically, the blood appears bright red as it hasn't mixed with stomach enzymes and acids.

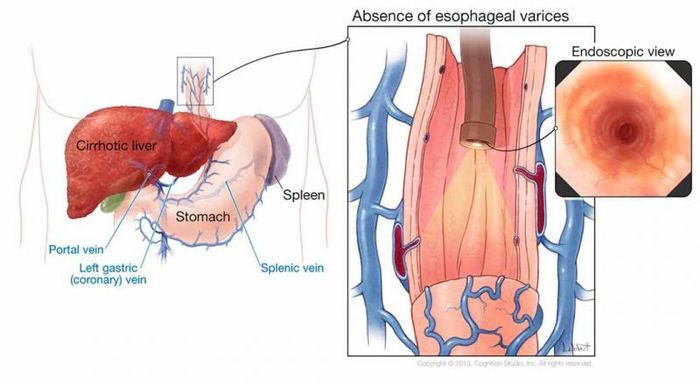
3. Esophageal Varices
The condition arises due to the sudden dilation of veins in the lower esophagus, often associated with liver disease. Hemorrhaging and vomiting blood result from the stretching and swelling of the esophagus. Bleeding from esophageal varices is typically sudden and may include food, often appearing dark. The mortality rate for esophageal varices is approximately 5-7%.
The primary cause of esophageal varices is cirrhosis. Scarring in the liver obstructs blood flow in the portal vein, the main vein carrying blood from the stomach and intestines to the liver. This increases pressure in the portal vein and nearby veins, a condition known as portal hypertension. As a result, blood seeks alternative pathways through smaller veins, such as those in the lower esophagus, which have thin walls and may rupture under pressure, causing bleeding.
Esophageal varices occur when veins in the esophagus dilate, commonly in individuals with severe liver disease. This condition develops when normal blood flow to the liver is blocked by a clot or scarring. To bypass the blockage, blood flows into smaller vessels not designed for high volumes, leading to leaks or ruptures, which can cause life-threatening bleeding. Once bleeding occurs, the risk of recurrence increases, and significant blood loss can lead to shock and death.
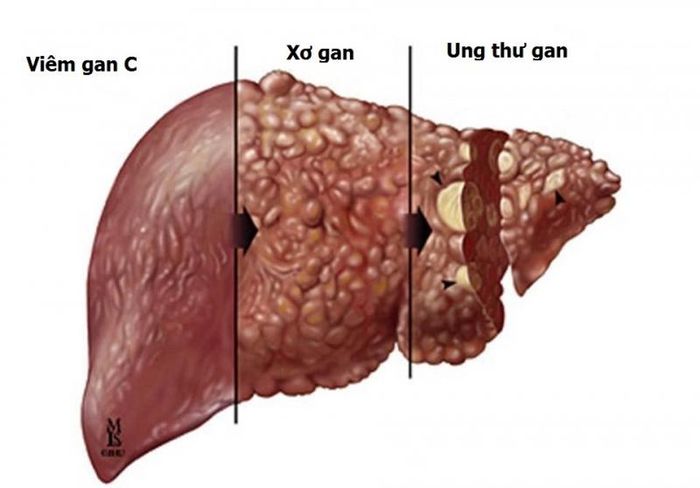
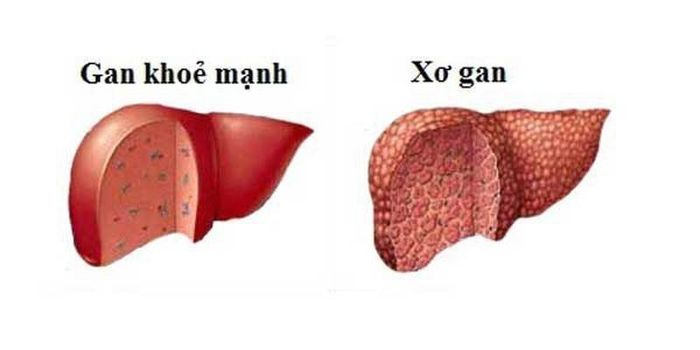
4. Cirrhosis
Cirrhosis results from chronic liver diseases that cause abnormal structural changes in the liver, replacing healthy tissue with scar tissue, which impairs liver function. Cirrhosis is the stage closest to liver cancer, where liver cells are severely damaged. It increases pressure within the liver and on esophageal veins, leading to vomiting blood when these veins rupture due to excessive dilation.
Cirrhosis is a chronic liver condition characterized by the replacement of liver tissue with fibrous scar tissue and the formation of regenerative nodules. Over time, untreated fibrosis spreads throughout the liver, severely impairing its function and potentially becoming life-threatening.
In its early stages, cirrhosis often shows no symptoms. As it progresses, symptoms may include fatigue, loss of appetite, jaundice, darkening of the skin, nosebleeds, gum bleeding, swelling, itching, abdominal fluid buildup, and sexual dysfunction. Severe complications may involve vomiting blood or black stools due to ruptured esophageal veins, hepatic coma, kidney failure, infections, or liver cancer.
Complications such as gastrointestinal bleeding, hepatic encephalopathy, or portal hypertension can arise. If these signs are not detected, patients may not qualify for liver transplants. The average survival time for patients with advanced cirrhosis is approximately 12 months.
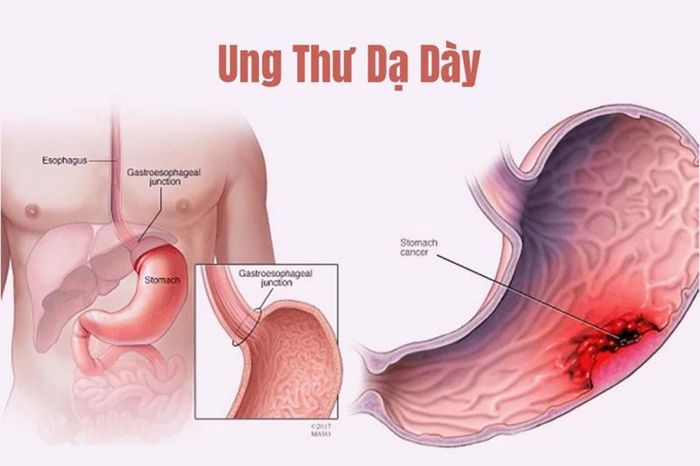
5. Stomach Cancer
This is a highly dangerous malignant disease of the digestive system. Initial symptoms include fatigue, indigestion, loss of appetite, and weight loss, which closely resemble gastritis. The danger lies in its late detection, as its symptoms mimic many other conditions. Stomach cancer causes ulcers and leads to vomiting blood.
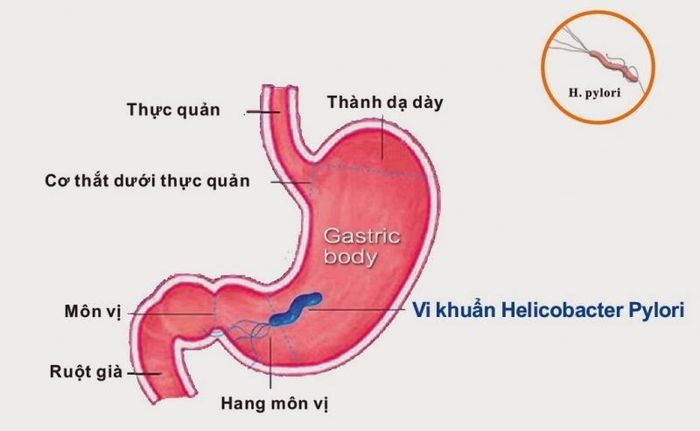
Some causes of stomach cancer include frequent consumption of nitrate-rich foods, genetic factors like atrophic gastritis, adenomatous polyps, stomach ulcers, Helicobacter pylori infection, and reduced stomach acid levels.
Late-stage stomach cancer patients may experience epigastric pain, loss of appetite, weight loss, fatigue, vomiting, bloody stools, or black stools, leading to significant blood loss and anemia. As the tumor grows, abdominal pain becomes frequent and severe, often unresponsive to painkillers. Complications like stomach perforation, hemorrhage, or necrosis may occur. Long-term patients may develop gastrointestinal bleeding, manifesting as vomiting blood, black stools, or blood in stool tests.
Stomach cancer involves abnormal, uncontrolled cell growth in the stomach, forming tumors. In advanced stages, malignant tumors can spread to nearby and distant organs, severely impacting health and potentially leading to death. Stomach cancer is a prevalent malignancy today due to unhealthy lifestyles and poor dietary habits. It is prone to metastasis and has a high mortality rate due to vague and nonspecific early symptoms. Early recognition of warning signs is crucial for effective treatment plans and improving survival rates.

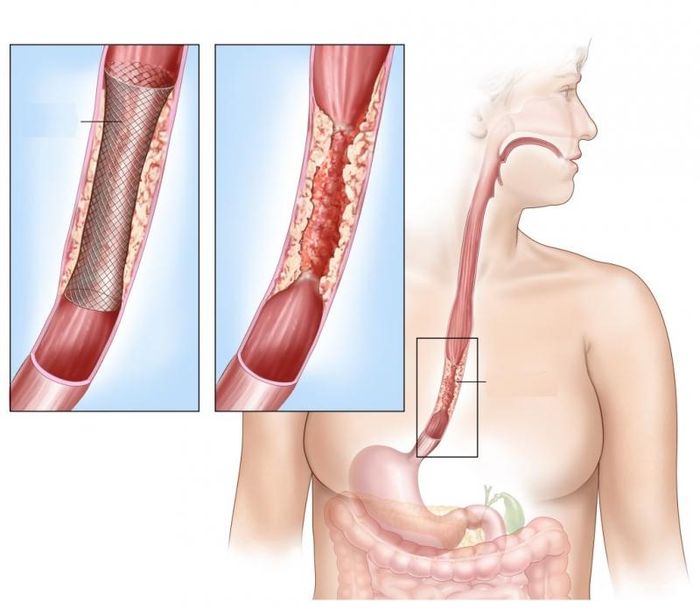
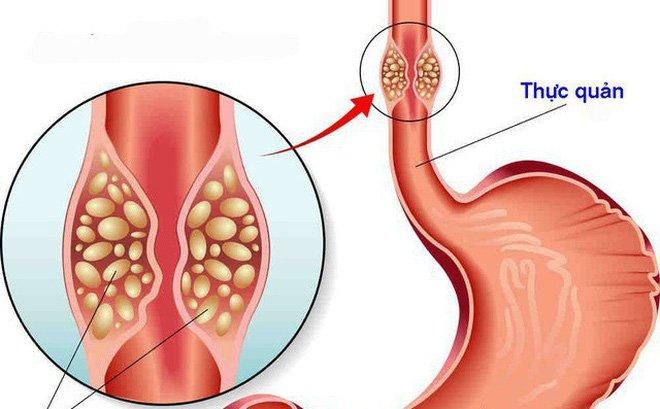
6. Esophageal Cancer
Like other gastrointestinal cancers, esophageal cancer shows few symptoms in its early stages, often resembling other esophageal conditions such as difficulty swallowing, pain, and bad breath. Additionally, esophageal cancer can cause vomiting blood when it invades blood vessels.
Esophageal cancer occurs when malignant tumors form from the epithelial cells of the esophagus, causing uncontrolled cell division and tumor growth. It is one of the most common cancers of the digestive tract. Due to varying symptoms across stages, it is often detected late, making treatment challenging.
The exact cause of esophageal cancer is unclear. It arises when cells in the esophagus develop DNA mutations, leading to uncontrolled growth and division. These abnormal cells accumulate, forming tumors that can invade nearby structures and spread to other parts of the body.
Loss of appetite, difficulty swallowing, weight loss, and weakness are common issues for esophageal cancer patients. These symptoms may be exacerbated by cancer treatments and the need for liquid diets, tube feeding, or intravenous nutrition. Esophageal bleeding is another complication, which can occur gradually or suddenly and may require surgical or endoscopic intervention.
7. Trauma
Many abdominal injuries can cause vomiting of blood, though it is rarely sudden. Trauma such as gunshot wounds, blunt force, or stabbings in the abdominal area can rupture blood vessels or tear the stomach, leading to blood in vomit. The blood may appear dark red, bright red, or mixed with food.
Abdominal trauma refers to injuries affecting the abdominal region, which can be either blunt or penetrating and may damage internal organs. Common symptoms include abdominal pain, tenderness, rigidity, and bruising. Severe blood loss and infection are potential risks. Diagnosis often involves ultrasound, CT scans, or peritoneal lavage, and surgery may be required. Injuries to the lower chest can also cause spleen or liver rupture.
Symptoms may not appear immediately and can develop days after the initial injury. Victims of motor vehicle accidents may exhibit a "seatbelt sign," bruising along the belt's path, indicating potential internal organ damage.
Seatbelts can cause abrasions and hematomas, with 30% of those showing such signs suffering internal injuries. Early signs of abdominal trauma include nausea, vomiting, blood in urine, and fever. Injuries may cause abdominal pain, tenderness, distension, rigidity, or loss of bowel sounds. Abdominal trauma and wounds are common emergencies, with blunt trauma being more frequent in peacetime. Mortality rates depend on the injury's nature, severity, and the medical facility's capabilities.
8. Duodenal Ulcer
Duodenal ulcers are among the leading causes of vomiting blood, primarily due to Helicobacter pylori infection. Symptoms include vomiting blood and epigastric pain, often worsening on an empty stomach and easing after eating. Severe cases may erode blood vessels, leading to significant bleeding.
Dietary factors such as consuming spicy, acidic, or overly hot foods, alcohol, coffee, and fatty meals, along with smoking, irregular eating habits, and stress, contribute to the condition. Prolonged use of anti-inflammatory drugs like corticosteroids and NSAIDs can also reduce protective mucus, increasing ulcer risk. Family history of the disease is another significant risk factor.
Duodenal ulcers can lead to life-threatening complications like gastrointestinal bleeding, which may occur suddenly or after consuming irritants such as alcohol or anti-inflammatory drugs. Symptoms include vomiting fresh blood, black tarry stools, fatigue, and low blood pressure, requiring immediate medical attention.
Some individuals may experience mild or no symptoms, but the most common sign is a burning pain in the upper abdomen related to meals. Early diagnosis and treatment are crucial to prevent severe complications like perforation or hemorrhage, which can be fatal if untreated.
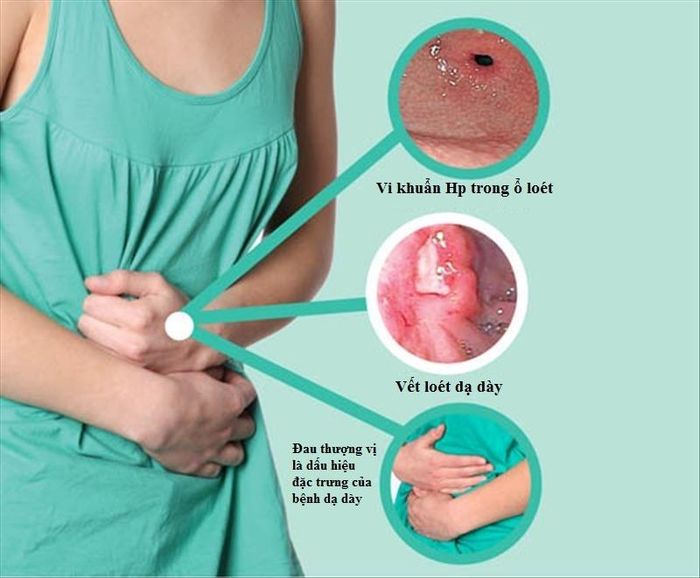
9. Gastritis
Gastritis, like duodenal ulcers, is often caused by Helicobacter pylori infection, elevated eosinophils, medications, chemicals, or certain foods. Bleeding and congestion can occur if the stomach lining is irritated by hard substances. Consuming spicy, hard-to-chew foods or inadequate chewing can lead to vomiting blood in gastritis patients.
Modern industrial lifestyles, characterized by rushed and irregular eating habits, have made gastritis increasingly common. However, many patients only seek medical attention when the condition has worsened, risking progression to gastric ulcers or even stomach cancer.
Gastritis occurs when excess stomach acid or bacterial infection damages the stomach lining, causing inflammation. It can be acute (sudden) or chronic (long-term). Damaged stomach linings make digestion difficult, leading to bloating, indigestion, nausea, and vomiting, especially when overeating. Patients may also experience the urge to vomit without actually doing so, causing significant discomfort.
While gastritis is relatively treatable, it should not be underestimated, as it can quickly lead to severe complications like gastric bleeding, characterized by vomiting blood or bloody stools. Such cases require immediate medical attention.
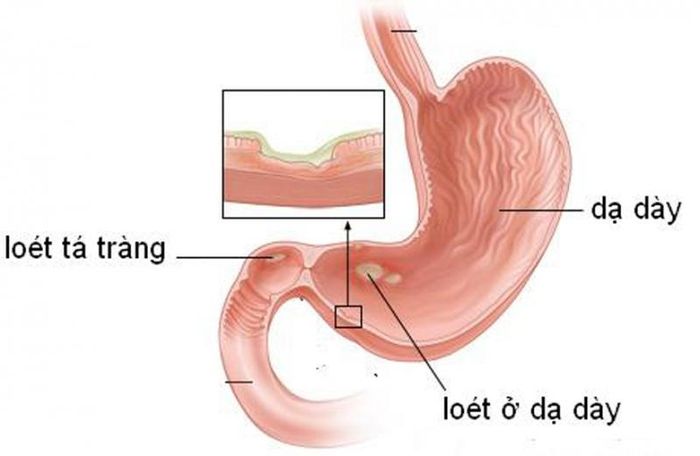
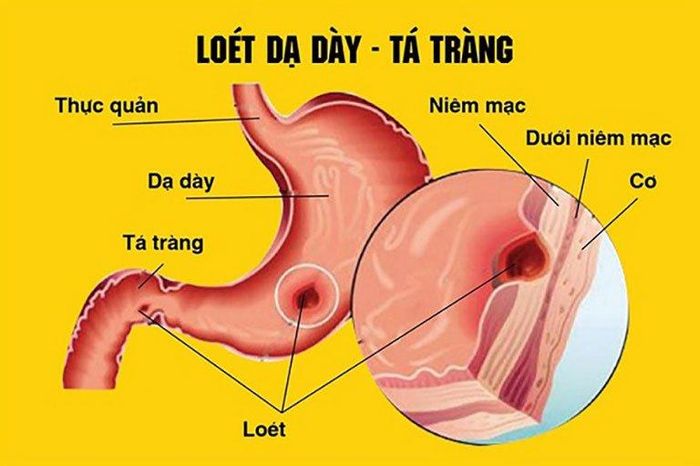
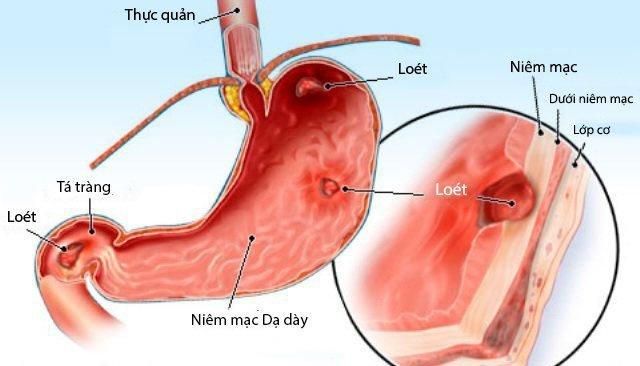
10. Gastric Ulcer
Similar to duodenal ulcers, gastric ulcers also cause vomiting of blood, accounting for up to 20% of cases. Causes include Helicobacter pylori infection, stress, and poor dietary habits. Symptoms include epigastric pain that worsens after eating and eases with antacids. If the ulcer erodes blood vessels, it can lead to vomiting blood and black stools.
Gastric ulcers, or peptic ulcers, are sores that develop on the stomach lining or the duodenum (the first part of the small intestine). These occur when the protective lining is compromised, exposing underlying tissues. Gastric ulcers are four times more common than duodenal ulcers. They are prevalent across all ages but more frequent in older adults. Reducing risk factors can help prevent the condition.
Gastric ulcers involve inflammation and sores on the stomach lining, often resulting from the erosion of the protective mucosal layer. Severe ulcers can cause gastrointestinal bleeding, which, if untreated, may lead to fatal blood loss.
Early detection and treatment of gastric ulcers improve outcomes. If left untreated, chronic ulcers can complicate treatment and increase the risk of severe complications like gastrointestinal bleeding and stomach cancer. Patients experiencing symptoms should seek medical attention promptly for effective management.