1. Causes of Coronary Artery Disease
The most common cause of coronary artery disease is atherosclerotic plaques that block the coronary arteries. Key risk factors that contribute to atherosclerosis include:
- High blood pressure
- Diabetes
- Cholesterol imbalances
- Smoking
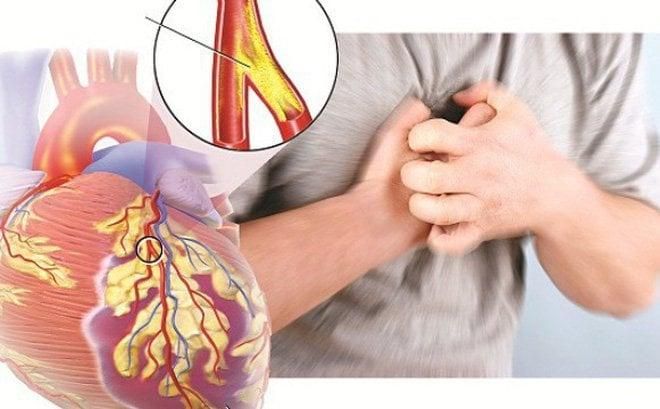
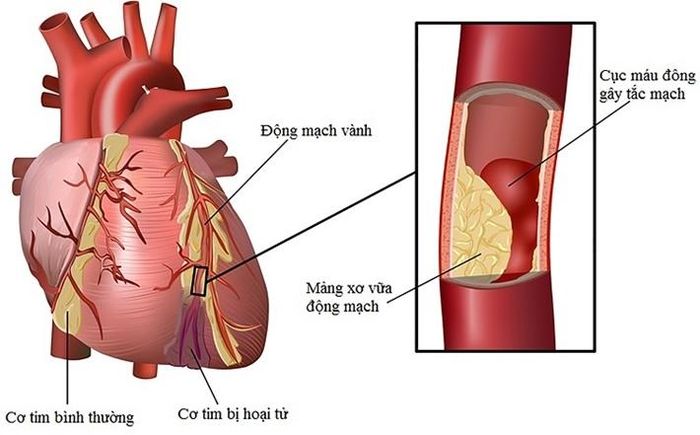
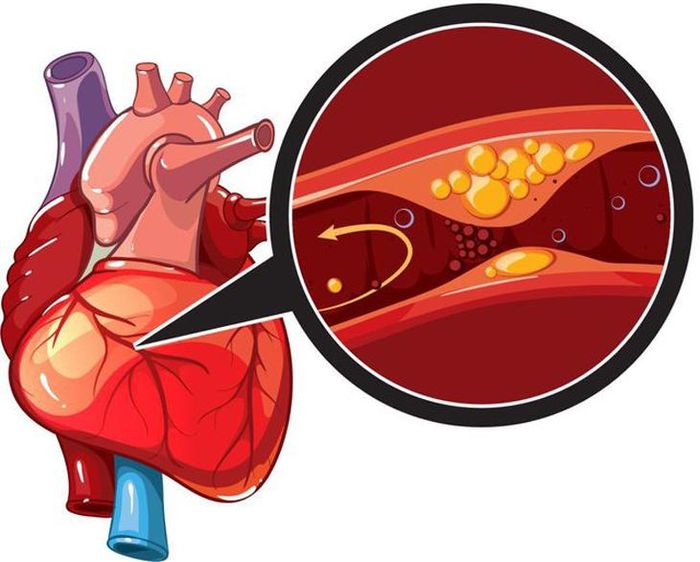
Once the inner walls of the coronary arteries are damaged, fatty deposits (plaque) made from cholesterol and other cellular waste materials begin to accumulate at the site of injury. This process is known as atherosclerosis. If the plaque surface ruptures, blood cells called platelets will gather at the site to attempt repair, forming a clot that completely obstructs the coronary artery, leading to a heart attack.
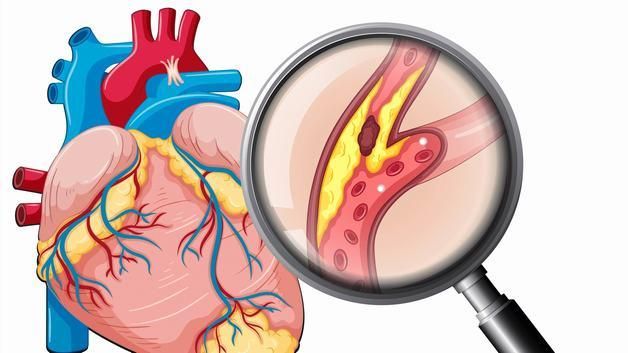
2. Who is at Risk for Coronary Artery Disease?
Age-related factors and family history are causes of coronary artery disease that cannot be altered. Those at higher risk for coronary artery disease are men over 50 and women over 55 years of age.
As we age and our body weakens, the likelihood of developing coronary artery disease increases. Typically, men are at greater risk for coronary artery disease than women, but postmenopausal women actually have a higher risk than men.
Additionally, individuals with a family history of coronary artery disease are at greater risk, especially if a close relative developed the condition before the age of 55 for men and 65 for women. The condition is also more common in people with conditions such as high blood pressure, diabetes, obesity, and lipid disorders.
3. Is Coronary Artery Disease Dangerous?
Coronary artery disease can lead to serious complications such as:
- Heart attack: This occurs when atherosclerotic plaques rupture, causing blood clots that completely block the coronary arteries, stopping blood flow. Without prompt medical intervention, the patient can die quickly.
- Sudden death: Around 30% – 50% of patients with acute heart attacks experience sudden death before reaching the hospital.
- Heart failure: Over time, lack of blood flow to the heart weakens its pumping ability. As the heart becomes progressively weaker, it eventually leads to heart failure.
- Severe valve regurgitation: This results from ruptured heart valve cords, valve prolapse, dilated valve rings, or abnormal contraction of the left ventricle. Ultimately, this causes the heart to enlarge, leading to worsening heart failure.
- Arrhythmia: Coronary artery disease deprives the heart of oxygen, disrupting its electrical system. This can cause dangerously rapid, slow, or irregular heartbeats. In some cases, arrhythmias can pose a life-threatening risk to the patient.
4. Diagnosing Coronary Artery Disease
To diagnose coronary artery disease, the doctor will begin by taking a detailed medical history, reviewing the main risk factors for the condition, conducting a physical examination, listening to the heart and lungs, and performing specific diagnostic tests to confirm the diagnosis.
The essential diagnostic tests for evaluating and diagnosing coronary artery disease include:
- Electrocardiogram (ECG)
- Chest X-ray
- Color Doppler echocardiogram
- Stress testing: treadmill ECG (for patients who can walk) or dobutamine stress echocardiogram (for elderly patients who cannot walk on the treadmill)
- Coronary CT angiography: helps assess the degree of blockage and calcification in the coronary arteries.
- Cardiac catheterization and coronary angiography: typically performed when stress test results are positive or coronary CT angiography shows narrowing. This procedure involves inserting a small tube into a blood vessel, usually in the arm or thigh, and advancing it to the heart. A contrast dye is injected to visualize any blockages. This is considered the gold standard for diagnosis, though it is invasive and should only be used when necessary to minimize risks.

5. Treatment of Coronary Artery Disease
The treatment for coronary artery disease depends on the severity of the condition. All treatment methods aim to enhance blood supply to the heart, alleviate symptoms, and extend the patient's lifespan. These include:
- The basic treatment in all stages of the disease involves lifestyle changes and medication.
- Interventional treatments include angioplasty, coronary stent placement, and coronary artery bypass surgery.
Specifically:
Lifestyle changes: Patients should quit smoking, exercise regularly throughout the week, lose weight if overweight or obese, follow a heart-healthy diet, and limit alcohol consumption.
Medication treatment: Patients need to take medications consistently and long-term, with lifelong use of antiplatelet drugs, especially for those who have had a heart attack, stent placement, or coronary artery bypass surgery.
- Antiplatelet medications: aspirin, clopidogrel, ticagrelor, prasugrel
- Lipid-lowering drugs to reduce atherosclerosis: statins (atorvastatin, rosuvastatin, simvastatin, pravastatin, etc.)
- Treatment for related conditions such as hypertension and diabetes
- Anti-anginal medications: such as beta-blockers, calcium channel blockers, nitrates, nicorandil, ranolazine, trimetazidine, etc.
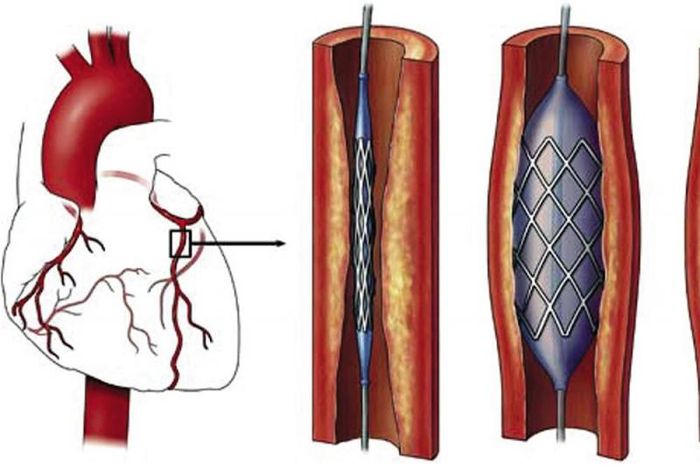
Percutaneous coronary intervention and stent placement: A coronary stent is a small mesh metal framework inserted into the coronary artery to widen the narrowed artery and prevent it from closing again.
Coronary artery bypass surgery: This involves using a segment of an artery or vein to create a bypass around the damaged part of the coronary artery, allowing blood to reach the deprived areas of the heart muscle. After stent placement or bypass surgery, patients need to continue taking medications regularly and make lifestyle changes to prevent restenosis or blockage in the stent or bypass graft.
6. What Should Patients with Coronary Artery Disease Eat?
Antioxidant-rich foods: These foods include:
- Colorful fresh fruits, dark leafy vegetables such as broccoli, kale, spinach, oranges, watermelon, tangerines, strawberries, carrots, and more.
- Whole grains: brown rice, oats, etc.
- Use vegetable oils such as peanut oil, sunflower oil, etc.
- Nuts: almonds, cashews, walnuts, etc.
- Omega-3 from fatty fish like salmon, mackerel, tuna, and herring.
These foods are not only packed with antioxidants but also have strong anti-inflammatory properties that help reduce the progression of coronary artery disease.
Foods that promote blood circulation: Good blood circulation is crucial for patients with coronary artery disease, making these foods essential in daily meals.
- Spices: ginger, garlic, turmeric, onions, licorice, cinnamon, etc.
- Fruits: blueberries, fresh grapes, raisins, strawberries, etc.
These foods are rich in salicylates, which improve blood flow by preventing blood clots. Additionally, these spices enhance the flavor of your meals, so be sure to include them in your daily diet.
Foods that help lower cholesterol: One of the key foods for lowering blood cholesterol is soluble fiber, as it helps reduce fat absorption in the intestines and increases its removal from the bloodstream. Soluble fiber is found in foods such as:
- Whole grains, brown rice, whole wheat bread.
- High-viscosity vegetables: Malabar spinach, jute leaves.
- Legumes: peas, red beans, etc.
- Fruits: guava, oranges, apples, papaya, pears, etc.
Additionally, how you prepare your food is crucial for ensuring optimal nutrient absorption. Opt for steamed, boiled, or raw vegetables instead of stir-frying or deep-frying in excess oil. Those with high cholesterol should also limit the use of butter, mayonnaise, or animal fats in cooking.
For fried foods, replace them with vegetable oils containing healthy fats, such as peanut oil or coconut oil. Many people tend to reuse cooking oil, which is unhealthy and should be avoided.
Excessive salt intake raises blood pressure and worsens coronary artery disease. Therefore, it is important to reduce the amount of salt or seasoning powder used in food preparation. Health experts recommend the Mediterranean diet, which includes a variety of foods like fish, green vegetables, sesame oil, olive oil, and nuts, as an effective way to manage the condition.

7. Preventive measures for coronary artery disease
Adhering to a healthy lifestyle: This is the most effective measure to prevent cardiovascular diseases, including coronary artery disease.
- Quit smoking, avoid secondhand smoke
- Exercise regularly, at least 30–45 minutes each day, all week long. Activities can include walking, running, cycling, swimming, playing badminton, table tennis, golf, practicing yoga, aerobic exercises, meditation, etc., depending on individual health conditions; avoid stress in life and work.
- Lose weight if overweight or obese (when BMI > 23): aim for a 5% to 7% weight loss every 6 months until reaching an ideal weight (BMI between 18–22)
- Heart-healthy diet:
- Eat less fat, fatty meats, carbohydrates, processed foods, fast food, limit salt, reduce alcohol consumption.
- Include fish, poultry; eat plenty of fruits, vegetables, nuts, fresh, organic foods.
Proper management of related health conditions
- Control blood sugar levels if you have diabetes
- Maintain stable blood pressure and cholesterol levels


8. What is coronary artery disease?
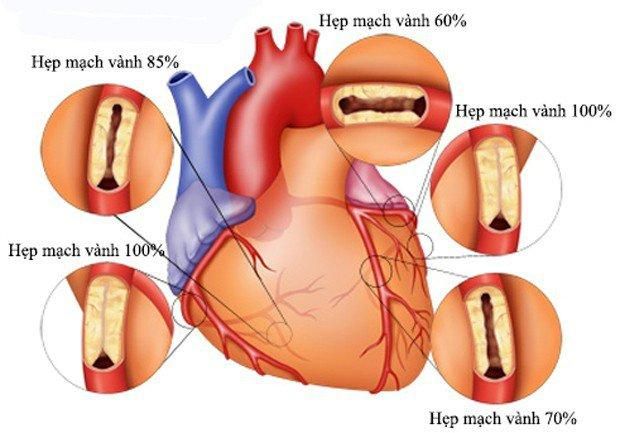
Coronary artery disease occurs when one or more branches of the coronary arteries become narrowed or obstructed due to the buildup of plaque inside. The arteries in our body are normally soft and elastic, but they become narrower and stiffer over time due to plaque deposits such as cholesterol and other substances, leading to a condition known as atherosclerosis.
As coronary artery disease progresses, blood flow through the arteries becomes more difficult. As a result, the heart muscle may not receive enough blood and oxygen, leading to chest pain or a heart attack. Most heart attacks happen when a blood clot suddenly moves to a narrowed part of a blood vessel, blocking the flow of blood to the heart, causing permanent damage to the heart muscle.
9. Types of coronary artery disease
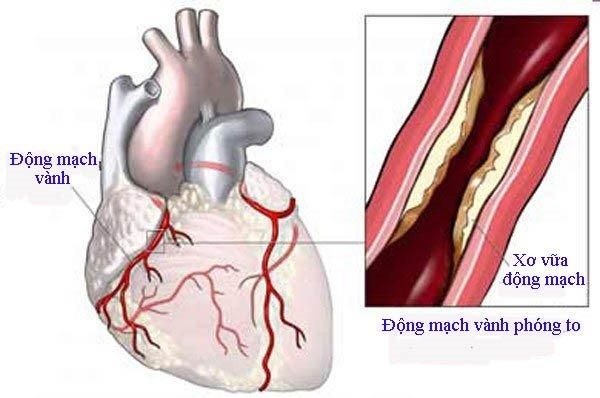
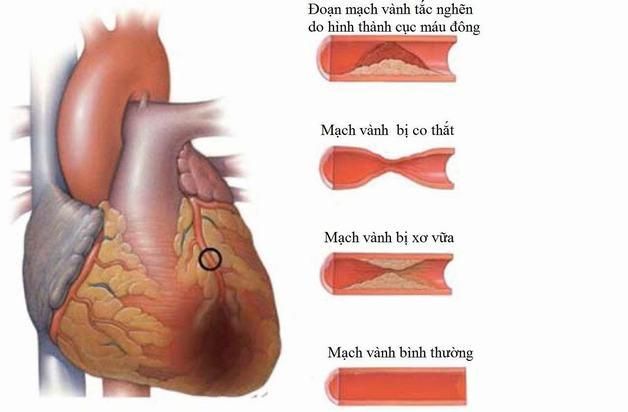
Most cases of coronary artery disease involve atherosclerosis, while some may experience narrowing of the blood vessels. Based on this, experts classify coronary artery disease into three types:
- Atherosclerotic coronary artery disease: Atherosclerotic plaques can be either soft or hard, formed from triglycerides, cholesterol, calcium, and inflammatory cells on the walls of the coronary arteries. Hard plaques are less likely to rupture and cause blood clots because they are more stable, while soft plaques are prone to rupture and form clots that may lead to stroke or heart attack.
- Spontaneous coronary artery dissection: This condition occurs when the layers of the coronary artery wall suddenly tear, allowing blood to leak into the layers, slowing down or blocking blood flow to the heart. This can lead to arrhythmias, chest pain, and even death.
- Coronary artery spasm: This condition is triggered by stimulants, prolonged stress, exposure to cold air, smoking, etc., which can cause one or more coronary arteries to temporarily narrow.
10. Signs of coronary artery disease
Chest pain or shortness of breath during physical activity is the most common symptom of coronary artery disease. Patients often experience a heavy, tight, or constricting sensation in the chest, typically on the left side or behind the breastbone. This condition arises during exertion, such as walking uphill, stress, or anxiety. The pain usually lasts for a few minutes (3 – 5 minutes), often less than 15 minutes, and rarely lasts only a few seconds. The pain can radiate to the neck, jaw, shoulders, left arm, or the back. Notably, the pain diminishes when resting or taking nitrate medication.
Other signs that may indicate coronary artery dysfunction include:
- Shortness of breath
- Breathlessness
- Dizziness
- Irregular heartbeats
- Near fainting...
Among these symptoms, women often experience milder manifestations than men. In addition to chest pain, nausea, shortness of breath, fatigue, and sweating may also occur.
However, by the time these symptoms are noticeable, the condition may have already progressed. Therefore, to prevent and address coronary artery disease early, it is essential to regularly monitor your health, especially if you are at risk for coronary artery disease. If you notice mild symptoms, seeking medical attention promptly is recommended.