1. Mastitis
Mastitis refers to the inflammation and pain in a woman's breast tissue. This condition is most common among breastfeeding women, typically occurring within the first three months after childbirth.
Blocked milk in the breast is the primary cause of mastitis. Other contributing factors include:
- Blocked milk ducts: If the breast isn't fully emptied after feeding, milk ducts may become blocked. The blockage can cause milk to flow backward, leading to breast infection.
- Bacterial invasion: Bacteria from the baby's skin or mouth may enter the milk ducts through cracked nipples or the milk duct openings. Milk buildup provides a favorable environment for bacterial growth.
- Chronic mastitis and a rare type of breast cancer called inflammatory breast cancer: Chronic mastitis occurs in women who are not breastfeeding. In postmenopausal women, breast infections may relate to chronic inflammation of the ducts under the nipple. Hormonal changes can cause the milk ducts to become blocked, allowing the infection to spread.
- Infections often recur after antibiotic treatment.
- Breast infections are most likely to occur one to three months postpartum, but they can also affect women who aren't breastfeeding and those after menopause.
In breastfeeding women, mastitis is often caused by milk accumulation within the breast, known as milk stasis. Milk stasis can occur for several reasons, including:
- Incorrect breastfeeding positioning or latch
Baby's sucking issues
Infrequent feedings or insufficient nutrition - In some cases, this milk accumulation can lead to a bacterial infection, known as infectious mastitis.
In non-breastfeeding women, mastitis often results from an infection caused by nipple damage, such as cracked or sore nipples.
In healthy women, mastitis is rare. However, those with diabetes, chronic conditions, AIDS, or weakened immune systems are at a higher risk.
Minimize the risk of mastitis by following these tips:
- Completely empty the breast when breastfeeding.
- Allow the baby to fully empty one breast before switching to the other.
- Vary breastfeeding positions during different feedings.
- Ensure proper latch while nursing.
- If the mother smokes, ask the doctor about quitting smoking.
Mastitis is usually treatable, and most women recover quickly and fully.
Recommended measures include:
- Rest and drink plenty of fluids.
- Use over-the-counter pain relievers, such as paracetamol or ibuprofen, to reduce pain or fever.
- Avoid wearing tight clothing, including bras, until symptoms improve.
- If breastfeeding, continue to nurse and ensure the baby is latched properly.
- Breastfeeding during mastitis, even with an infection, is safe for the baby and can help relieve the mother's symptoms.
- The mother should breastfeed more frequently, express any remaining milk after feeding, and pump between feedings.
- For non-breastfeeding women with mastitis or breastfeeding women with suspected infection, an antibiotic regimen is typically prescribed to manage the infection.


2. Breast Abscess
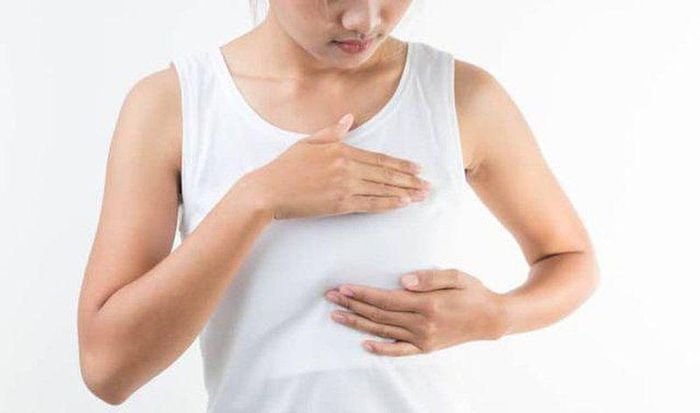
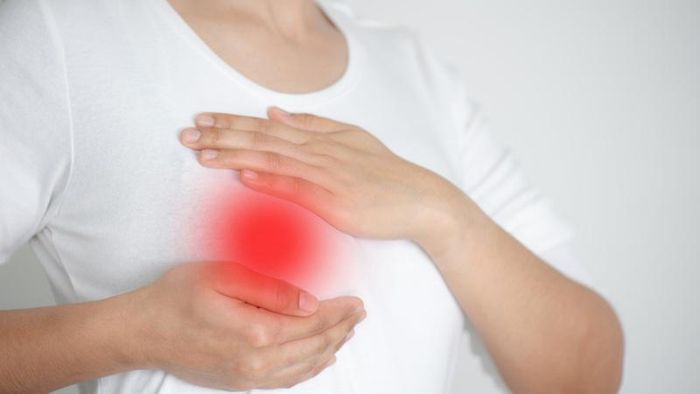
Breast Abscess is a type of bacterial infection that leads to swelling, redness, palpable lumps that are tender, and possibly a foul odor in the breast. Diagnosis can be made based on common signs of a breast abscess such as:
- High fever, chills.
- Breast swelling - warmth - redness - pain, with soft lumps that are indentable when pressed. Tender lymph nodes in the armpits, milk mixed with yellow pus.
- Ultrasound shows multiple fluid-filled cavities in the breast.
- Blood tests show increased white blood cell count (neutrophils).
- CRP (C-reactive protein) levels rise.
Pus aspirated from the abscess, with bacterial culture and antibiotic susceptibility testing. - In some cases, a breast abscess may be an indicator of breast cancer.
For effective treatment of a breast abscess, consider the following advice:
- Rest as much as possible and avoid breastfeeding from the affected breast.
- Consume soft, easy-to-digest foods to ensure sufficient nutrition for quick recovery.
- Feed from the unaffected breast or pump milk for the baby to prevent infection transfer.
- Gently massage, apply warm compresses, and express milk to assist in milk duct clearance.
- Take prescribed antibiotics, anti-inflammatory drugs, painkillers, and antipyretics as directed by the doctor.
- If medication does not fully resolve the infection, the abscess may need to be drained. For superficial abscesses, a simple incision to drain the pus is sufficient. For deeper abscesses, drainage is performed near the surface, avoiding the nipple by 2-3 cm. After drainage, a drainage tube is inserted, and the abscess cavity is flushed with antiseptic solution daily, along with systemic antibiotics.
Prevention of breast abscess:
- Breast abscesses mainly occur in women after childbirth and breastfeeding. To prevent this condition, nursing mothers should pay attention to the following:
- After childbirth, gently massage the breast to help clear milk ducts and initiate breastfeeding promptly, ensuring frequent and correct positioning.
- Ensure proper hygiene of the nipple before and after breastfeeding.
Make sure the baby fully drains the breast and alternate between sides, or express excess milk after each feed. - If there is milk duct blockage, treat it promptly to clear the ducts. To prevent blockage, massage, apply warm compresses, use infrared light, or pump milk.
- Avoid cracking or injury to the nipple as it provides a good entry point for bacteria that can cause mastitis. Also, avoid dry or cracked skin. Wear a properly fitting bra to prevent breast damage.
Avoid early weaning; if weaning, gradually reduce the number of feeds over time.
In conclusion, we answer the question “Is a breast abscess dangerous?” At the first signs of pain, tenderness, swelling, or cracked nipples, cease breastfeeding temporarily and seek immediate medical attention to ensure timely treatment and protect your health.
3. Insufficient Milk
After giving birth, mothers often wish for an abundant supply of milk for their babies. However, sometimes this essential source of nutrition is not as plentiful, especially after six months, when breast milk tends to decrease. As a result, many women are left wondering how to deal with diminishing milk supply.
Below are some methods to help improve the situation of reduced milk supply:
- Change the mother's diet
- Daily meal plan
To combat the issue of decreasing milk supply, mothers should consume a variety of foods and increase their intake compared to usual, ensuring sufficient energy and nutrition for both mother and child. A balanced meal should include the following four food groups:
- Protein: Found in meat, fish, eggs, milk, and legumes...
- Healthy fats: Found in oils, fats, and butter
- Carbohydrates: Mainly from rice, noodles, and potatoes...
- Vitamins and minerals: Fresh vegetables and fruits are highly recommended
Regarding food quantity, mothers should aim to eat 5 to 6 times a day, especially before breastfeeding to stimulate milk production. Below is a suggested meal plan for mothers to follow:
- 200 grams of meat or fish
- 1 egg
- 1 liter of fresh milk or formula
- 200 to 300 grams of fruits
- 500 to 600 grams of vegetables
Additionally, mothers can try traditional foods that are known to enhance milk production, such as pig's feet stew with green papaya, peanut porridge, or black sesame dessert. There are not many foods that breastfeeding mothers need to avoid, but it is advisable to limit spicy ingredients like garlic, chili, and onions to prevent affecting the taste of breast milk.
Drink plenty of water: Water also helps stimulate milk production, so mothers should aim to drink 2.5 to 3 liters per day. The best times to drink water are when feeling thirsty, before and after breastfeeding, and at night before going to bed to encourage milk flow. Recommended drinks include:
- Mother's nutritional milk
- Fruit juices
- Broth
- Plain water
- Herbal teas or herbal infusions
- However, women should also keep in mind that consuming more food and drinks doesn't necessarily result in more milk. On the contrary, an unbalanced diet can disrupt the mother's digestive system and even lead to constipation in the baby.
Green papaya stew with pig's feet and peanuts is considered a very effective dish for boosting milk supply.
Breastfeeding habits
Baby's breastfeeding position: Although mothers may have two full breasts, improper breastfeeding techniques can cause the milk supply to decrease after six months or sooner. It is important for mothers to pay attention to the baby's sucking action and ensure proper breastfeeding through the following signs:
- The baby's body is close to and facing the mother
- The baby's chin touches the mother's breast
- The baby's mouth is wide open, and they latch onto most of the areola, not just the nipple
- The baby's lower lip is turned outward
- The mother should be able to see the baby sucking slowly and firmly, and hear the swallowing sounds
Breastfeeding tips: Even if the milk supply is decreasing, mothers should continue breastfeeding regularly, as the baby's sucking will stimulate milk production. This action helps boost milk flow and return to normal. Mothers should remember these tips:
Do's:
- Each breastfeeding session should last around 20 to 30 minutes or until the baby stops on their own
- Choose a quiet place, just the mother and baby, to help the baby focus on breastfeeding
- Ensure the baby finishes one breast before moving to the other, making sure to fully utilize the rich milk at the end of the breast and stimulate milk production evenly
- Relax and enjoy time after feeding, allowing the baby to digest easily and the mother to feel less discomfort
Don'ts:
- Don't remove the breast when the baby falls asleep, as they will naturally release the nipple when full
- Don't wait for the baby to cry before breastfeeding; follow a regular schedule
- Don't leave milk in the breasts, as this can hinder new milk production
Psychological factors: The decrease in milk supply after six months or the delayed milk flow can be attributed to various factors, including cesarean delivery, postpartum medications, and psychological stress during the breastfeeding period.
To ensure enough milk for breastfeeding, mothers should maintain a balanced diet and rest. They should avoid feeling discouraged or worried if milk supply decreases. Psychological factors play a crucial role in milk production, so mothers need to stay calm and trust that they can still produce enough milk for their babies. Doctors suggest that mothers continue to nurse their babies, as this action signals the body to produce more milk. If mothers become too stressed or stop breastfeeding, milk production may halt completely.
Additionally, mothers can try massaging the breast, gently rubbing the breast and nipple area to facilitate milk flow. Taking advantage of a steady water stream during a shower can also be an effective method.
Overall, a decrease in milk supply after six months is quite common. In some cases, women may experience a sudden loss of milk just a few weeks after birth. In these situations, ensuring adequate milk supply for breastfeeding when milk decreases involves a nutritious diet, rest, and maintaining a relaxed mental state. The key is that despite reduced milk supply, mothers should continue breastfeeding as usual for the best chance of increasing milk production again. Mothers should avoid using formula or introducing solids too early, as this may hinder the baby's development.


4. Engorged breasts
Breast engorgement after childbirth occurs as a result of increased blood flow to the breasts in the days following delivery. While this increase in blood flow helps your breasts produce more milk, it can also lead to pain and discomfort.
Milk production may not begin until 3-5 days after childbirth. Engorgement can happen for the first time within the first one or two weeks postpartum. It may also reoccur at any time if you continue breastfeeding.
Additionally, certain conditions or behaviors can make you more likely to experience swelling, which is often associated with breast engorgement.
The following factors may contribute:
- Your baby skipping a feeding
- Missing a pumping session
- Producing excess milk for the baby to consume
- Introducing too much formula between feedings, which could reduce breast milk intake
- Weaning too quickly
- Nursing a sick child
- Difficulty with latch and breastfeeding
- Not pumping after birth because you’re not planning to breastfeed
Regardless of the cause, engorgement can be painful. Below are some home remedies you can try:
- Feed your baby frequently: Aim for at least 1 to 3 hours between feeds, day and night.
- Let your baby nurse as long as they want, but for at least 20 minutes per session.
- If your baby is sleepy, try waking them to feed.
- Consider hand expression or pumping a little before each feed to reduce engorgement, soften your breasts, and help your baby latch more easily.
- Massage your breasts while nursing to help encourage more milk flow for your baby.
- After feeding, apply a cold compress to your breasts to alleviate pain and swelling.
- Change breastfeeding positions to help your baby drain milk from different areas of the breast.
- Consult with your doctor about using over-the-counter pain relievers such as Tylenol or Motrin to ease discomfort and inflammation.
- Feed from one breast per session to fully empty that side before moving to the other breast.
- Avoid giving your baby formula or water between feedings, as this can reduce their intake of breast milk and increase your risk of engorgement.
- Take a warm shower or use warm compresses right before breastfeeding. However, avoid using heat between feedings, as this can worsen swelling.
- Rest as much as possible.
- Watch for signs of leaking milk, blocked milk ducts, or breast infection.
- If you are weaning, try doing so gradually. A slow weaning process can help you avoid engorgement altogether.


5. Blocked Milk Ducts
Blocked Milk Ducts are a common issue for new mothers, especially those who are breastfeeding for the first time. Blocked ducts occur when milk gets trapped in the milk ducts within the breast. This condition can make breastfeeding or pumping milk for storage painful and challenging.
Although blocked milk ducts do not pose a life-threatening risk, if left untreated, they can lead to more serious health issues for the mother, such as mastitis, which can cause infections or even an abscess, a potentially dangerous situation. If the blockage persists, it may lead to fibrosis or the formation of a lump in the breast tissue. Additionally, blocked ducts can interfere with milk production, eventually causing a loss of milk supply and forcing the mother to stop breastfeeding in favor of formula feeding.
A few days after childbirth, the mother may feel her breasts become warm, heavy, and hard. Milk will begin to flow in streams through the milk ducts, creating lumps despite milk still being produced. This is usually a sign of breast engorgement that occurs around the 2nd or 3rd day postpartum. Without prompt intervention, blocked ducts may lead to infection, fever, or even postpartum depression.
Treatment:
- For blocked ducts, it's essential to try to express milk to unblock the duct (either by hand or with a breast pump). Once the duct is cleared, the fever should subside, and the risk of inflammation or abscess can be avoided without needing antibiotics. In cases where the blockage has progressed into an infection or abscess, antibiotics will be required, and if the condition doesn't improve, drainage may be necessary after antibiotic treatment.
- If a mother with a blocked duct has a high fever, it may cause the baby to experience digestive upset (such as green, foamy stools or even diarrhea if milk contains pus). In such cases, it’s best to avoid nursing from the affected breast until it is healed and instead express the milk. Preventing inflammation and abscesses is key to preventing blocked ducts. If the nipple cracks or becomes sore, treatment should be applied immediately.
- If the blocked duct feels hard or uncomfortable, it is advisable to breastfeed frequently to express some milk or gently massage the area, combined with warm compresses to help clear the duct. Massaging the breast while breastfeeding or pumping may also help, and experts recommend ensuring ample rest and hydration to maintain milk flow.
- If the blockage persists after a few days and hard lumps remain, it may help to press the breast against the chest wall or use two hands to apply pressure. Gentle circular massage around the hardened areas can help break up the blockage. Do this slowly, gradually increasing the pressure for about 20 rounds, and then reverse the motion. Combining this with warm compresses and using a breast pump can also aid in clearing the ducts.
- If none of the above measures work, it's important to visit a healthcare provider for prompt treatment to avoid complications like breast abscess. Many hospitals now offer chiropractic treatments to address blocked ducts without the need for medications. This technique involves using gentle finger pressure on the spine to help open up the milk ducts and soften the breast. In urgent cases, it's crucial to seek medical care for timely intervention and to avoid further complications.


6. Nipple Pain and Cracks
Cracked or Bleeding Nipples can cause significant pain during breastfeeding. If you experience this condition, it's important not to endure the pain, but instead seek medical advice at the nearest healthcare facility to determine the cause and receive proper treatment to prevent potential complications.
Typically, bleeding nipples are not a major concern and are often caused by injuries or friction, such as from a bra or a rough shirt. It is quite common to notice some blood or unusual discharge from the nipples, even while breastfeeding. Around 5% of women need to seek treatment for nipple discharge.
For first-time mothers, breastfeeding may take some time to master. In the first few days, your nipples may become sore or cracked, and you might notice blood or cracks around the nipple or areola.
However, breastfeeding itself shouldn't cause pain or bleeding. If bleeding continues over the first few days or weeks of breastfeeding, it could indicate improper latch.
Other signs of poor latching include:
- Flat or wedge-shaped nipples, or white tips after feeding
- Severe pain with each feeding
- The baby seems still hungry after breastfeeding
- The lower part of the areola doesn't fit into the baby's mouth
If you’ve been breastfeeding for a few months and suddenly experience pain, this could be a sign of infection. To address this, you can try the following solutions:
- Check the baby’s latch: The ideal latch is asymmetrical, with the baby’s mouth covering most of the areola below the nipple. To achieve this, guide the baby’s nose towards the nipple, ensuring their lower gums are further from the base of the nipple when they open their mouth. Once the baby opens their mouth, quickly latch them on.
- Try different breastfeeding positions. Certain positions, like holding the baby lying in your arms or lying beside you, might make it easier for your baby to latch comfortably and correctly.
- Feed from the less damaged side first. Babies tend to latch more gently on the non-damaged side when they are less hungry. You could also limit the feeding time on the affected side to less than 10 minutes.
- Apply a cold compress to numb the sore nipple before breastfeeding. Cold can help alleviate pain, especially when the pain is most intense at the beginning of a feeding session.
- Breastfeed more frequently. Nursing every two to three hours can help prevent engorgement and relieve pressure on the breasts.
- Express milk before feeding. If engorgement causes your nipple to become flattened, you can express milk for a minute or two before breastfeeding to make it easier for your baby to latch on properly.
- Limit the duration of feeding sessions. Some babies continue sucking even after they're done feeding, which can cause irritation to the skin. Listen for the baby swallowing, and when they stop, gently remove them from the breast. You can also consider limiting each feeding session to 10-15 minutes on each side. If you shorten feeding times, consider expressing milk by hand or using a pump to maintain your milk supply.


