1. Causes of Pancreatic Cancer
Pancreatic cancer generally has a poor prognosis, even when detected early. However, this disease is rarely diagnosed in its early stages, and it spreads quickly, which makes it highly fatal. One preventive measure against pancreatic cancer is understanding the causes of the disease and whether you belong to a high-risk group, so you can screen for the disease early.
To date, the exact causes of pancreatic cancer are still unknown. However, several risk factors make some individuals more likely to develop this cancer than others. These risk factors include:
- Smoking: Smokers are at the highest risk of developing pancreatic cancer, with their likelihood of getting the disease being nearly double compared to non-smokers. Around 20 - 30% of pancreatic cancer cases are believed to be caused by smoking.
- Overweight and Obesity: Individuals who are overweight or obese have a 20% increased chance of developing pancreatic cancer.
- Age: The risk of pancreatic cancer increases with age. Most patients diagnosed with this cancer are over 45 years old, and the average age at diagnosis is 71.
- Diabetes: Although science has not definitively linked pancreatic cancer with diabetes, it is observed more frequently in individuals with type 2 diabetes. This connection is likely related to other risk factors like obesity.
- Hazardous Work Environments: People working in environments exposed to chemicals, pesticides, dyes, or metallurgical substances face a higher risk of developing pancreatic cancer.
- Chronic Pancreatitis: Chronic pancreatitis, a condition where the pancreas remains inflamed over a long period, is linked to an increased risk of pancreatic cancer, though the risk is not as high as with some other factors.
- Stomach Issues: Infection with the ulcer-causing bacterium Helicobacter pylori can increase the risk of pancreatic cancer. Some believe that excessive stomach acid could also play a role.
- Family History: Individuals with a family history of pancreatic cancer are at higher risk of developing the disease themselves.

2. Techniques Used to Diagnose Pancreatic Cancer
If a pancreatic tumor is suspected, doctors may recommend undergoing specialized tests to confirm the diagnosis of cancer and determine the best course of treatment. Diagnostic techniques include ultrasound, computed tomography (CT) scans, magnetic resonance imaging (MRI), and sometimes positron emission tomography (PET) scans.
- Pancreatic Ultrasound: Ultrasound images of the pancreas help doctors identify abnormalities in the cells.
- Biopsy: A biopsy involves removing a small tissue sample to examine under a microscope. The doctor may collect a tissue sample from the pancreas by inserting a needle through the skin. Culturing the biopsy cells and performing necessary tests allow the doctor to detect any cancerous cells in the pancreas.
- Blood Test: A blood test used to detect pancreatic cancer is called CA19-9.
If the doctor confirms the presence of a tumor in the pancreas, they will work to determine the stage of the cancer, which helps decide the most appropriate treatment for the patient.


3. Treatment Methods for Pancreatic Cancer
The treatment approach depends on the stage and location of the cancer as well as the patient's overall health. Treatment options may include surgery, radiation therapy, chemotherapy, or a combination of these methods.
- Surgery: Surgical procedures used for individuals with pancreatic cancer include:
- Surgery for tumors at the head of the pancreas. If the tumor is located at the head of the pancreas, a procedure known as the Whipple procedure (pancreaticoduodenectomy) may be considered. This surgery involves removing the head of the pancreas, part of the small intestine (duodenum), the gallbladder, and part of the bile duct. In some cases, part of the stomach and nearby lymph nodes may also be removed. The surgeon then reconnects the remaining pancreas, stomach, and intestines to help with food digestion.
- Surgery for tumors in the body and tail of the pancreas: Surgery to remove the left side of the pancreas is called distal pancreatectomy. The surgeon may also remove the spleen during this procedure.
- Complete pancreatic removal surgery: In certain cases, the entire pancreas may need to be removed. While individuals can live relatively normal lives without a pancreas, they will require lifelong insulin supplementation to regulate blood sugar and digestive enzyme replacement.
- Chemotherapy: Chemotherapy uses drugs to destroy cancer cells. These drugs may be administered intravenously or orally. The doctor may use a single drug or a combination of 2-3 chemotherapy drugs depending on the disease's stage. Chemotherapy can also be combined with radiation therapy. Chemotherapy is commonly used for cancers that have spread beyond the pancreas. This combination may be used prior to surgery to shrink the tumor or after surgery to reduce the risk of recurrence. In cases where the cancer has metastasized, chemotherapy is often used to control the cancer's spread and prolong life.
- Radiation Therapy: Radiation therapy uses high-energy beams like X-rays and protons to destroy cancer cells. This treatment may be used before or after surgery, often in conjunction with chemotherapy. Traditional radiation uses X-rays, but some hospitals now offer proton beam therapy, which may be an option for certain patients with metastatic pancreatic cancer in stage III or IV.
4. Methods to Prevent Pancreatic Cancer
While there is currently no foolproof way to completely prevent pancreatic cancer, several measures can reduce the risk of developing this disease:
- Avoid tobacco use: Smoking is a major risk factor for pancreatic cancer. Smokers are two to three times more likely to develop the disease compared to non-smokers. Scientists believe that carcinogenic chemicals in cigarette smoke enter the bloodstream, damaging the pancreas and leading to cancer. Even users of smokeless tobacco are at higher risk for pancreatic cancer. Similarly, switching to low-nicotine tobacco products does not reduce the risk of this serious condition. To prevent pancreatic cancer, it is best to avoid tobacco altogether, which also helps to lower the risk of lung cancer, heart disease, and stroke.
- Maintain a healthy weight: Being overweight or obese can increase the risk of pancreatic cancer. Research involving over 300,000 older adults showed that those with obesity had a 45% higher risk of pancreatic cancer compared to those with a normal body mass index. Regular physical activity can help maintain a healthy weight and lower the risk of pancreatic cancer and other diseases.
- Follow a balanced diet: A diet rich in fruits and vegetables is beneficial for overall health and can help protect against various cancers, including pancreatic cancer. Incorporating more leafy greens like spinach, broccoli, apples, oranges, tomatoes, and bananas into your diet can provide essential vitamins and fiber that lower pancreatic cancer risk. Fish and lean meats supply omega-3 fatty acids, supporting the healthy functioning of body organs.
- Avoid foods with high nitrate content: These are often found in dark-colored foods. Nitrates in food can be converted into nitrites in the body, which may form nitrosamines. Nitrosamines have been linked to pancreatic cancer in animals and are considered potential carcinogens for humans.
- Steer clear of foods contaminated with Aflatoxin (mold): Carcinogens can develop in food when certain molds grow on them during processing or storage. It is important to discard moldy foods to reduce exposure to these harmful toxins.
- Know the early signs of pancreatic cancer: Symptoms such as unexplained weight loss, abdominal pain, loss of appetite, and jaundice can indicate pancreatic cancer. Early detection leads to timely treatment, improving the chances of successful outcomes.


5. What is the pancreas?
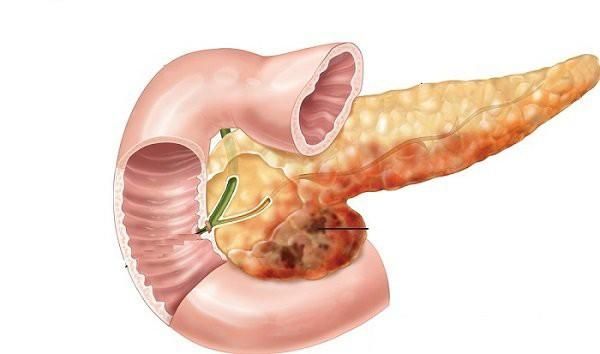
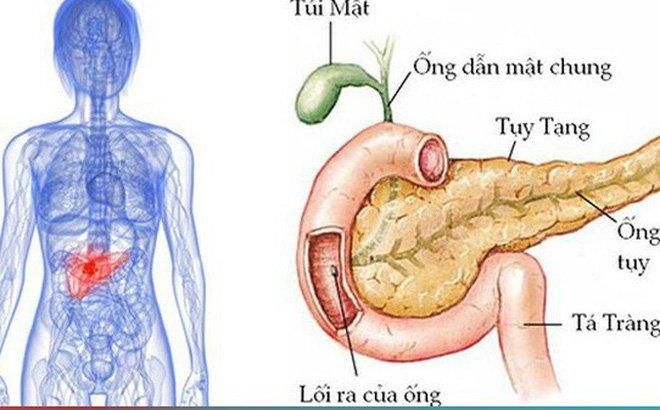
The pancreas is a leaf-shaped organ that produces digestive enzymes and hormones such as insulin. Located in the upper abdomen, near major arteries and veins, the pancreas consists of three parts – the head, body, and tail. The digestive enzymes and hormones produced in the pancreas are transported from the pancreas to the duodenum (the first part of the small intestine) via a duct called the pancreatic duct. The portion of the pancreas that produces hormones is referred to as the endocrine pancreas, while the part responsible for digestive enzyme production is known as the exocrine pancreas.
Pancreatic cancer is a type of cancer that forms in certain cells of the pancreas. Most pancreatic cancer patients (around 95%) develop it in the exocrine pancreas. Tumors can also form in the endocrine pancreas, but this is less common and often benign (non-cancerous). There are three main types of pancreatic cancer based on their nature:
- Exocrine carcinoma: This is the most common type of pancreatic cancer, accounting for about 80% of cases. Almost all cancers develop in the cells lining the pancreatic ducts.
- Cystic tumors are fluid-filled sacs that form in the pancreas. While most pancreatic cysts are benign, some can be cancerous.
- Acinar cell carcinoma: This type of cancer develops in the acinar cells of the pancreas, located at both ends of the ducts that produce digestive enzymes.
Pancreatic cancer is a disease that progresses silently, yet the cancer cells can spread quickly, especially during the metastatic stage. This is why it is one of the most difficult cancers to treat, with a high mortality rate.
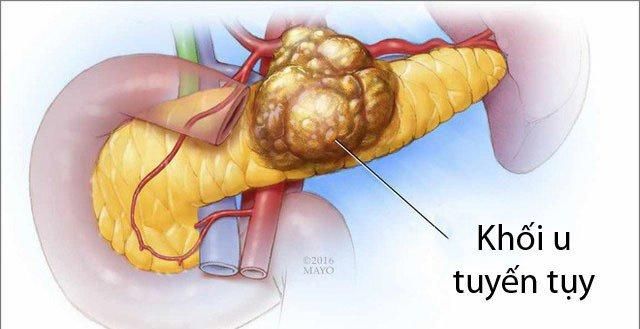
6. Phases of Pancreatic Cancer
Pancreatic cancer is a rare but highly dangerous condition due to its difficulty in early detection, challenging treatment options, and extremely high mortality rate. The majority of patients who undergo surgery for pancreatic cancer typically survive for 2-3 years, with a significant risk of recurrence after surgery. For those diagnosed at a later stage, where surgery is no longer an option, most patients do not survive beyond one year.
Pancreatic cancer is classified into four stages:
- Stage 1: A tumor appears in the pancreas, measuring less than 2cm, and typically does not present any noticeable symptoms, making it hard for patients to detect the illness.
- Stage 2: The tumor grows between 2cm and 4cm, invading surrounding pancreatic tissues but not yet affecting blood vessels. Cancer cells may also be present in nearby lymph nodes.
- Stage 3: The tumor can exceed 6cm in size, with cancer cells invading blood vessels and spreading to multiple lymph nodes and nearby organs.
- Stage 4: The tumor may reach any size and spread to distant organs such as the liver, lungs, and peritoneum.
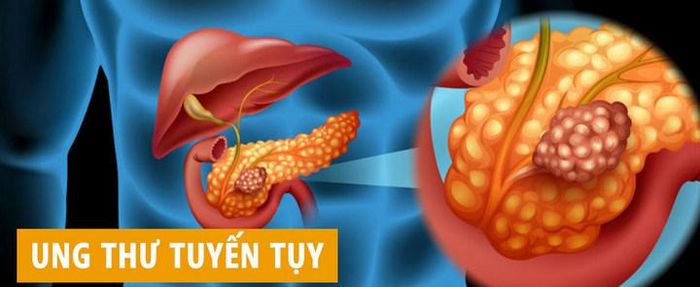
7. Symptoms of pancreatic cancer
Pancreatic cancer is one of the most deadly cancers because it disrupts the body’s hormone production, leading to severe consequences. Pancreatic cancer occurs when cells in the pancreas begin to divide uncontrollably. Symptoms can vary depending on the type of pancreatic cancer a patient has. There are two types of pancreatic cancer.
The symptoms of exocrine pancreatic cancer and pancreatic neuroendocrine tumors often differ. Having one or more of the following symptoms does not necessarily indicate pancreatic cancer. In fact, many symptoms may be caused by another condition. However, if any of these symptoms appear, it is important to visit a doctor for diagnosis and treatment.
Symptoms of exocrine pancreatic cancer
Pancreatic cancer in its early stages often does not present any symptoms. By the time symptoms appear, the tumor is often already spread beyond the pancreas, according to Step To Health.
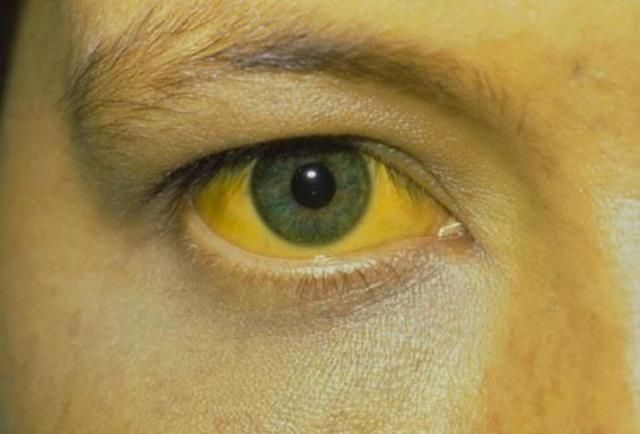
- Jaundice: Yellowing of the skin and eyes is one of the first signs of pancreatic cancer.
- Dark urine: The first sign can sometimes be darker urine due to an increase in bilirubin levels in the blood.
- Light-colored or greasy stools: Normally, bilirubin gives stool its brown color. If the bile ducts are blocked, stool can become pale or gray. Additionally, if bile and pancreatic enzymes cannot reach the intestine to help break down fats, stool can be greasy, according to Step To Health.
- Itching: When bilirubin builds up in the skin, it can cause itching.
- Abdominal or back pain: Pain in the abdomen or back is common with pancreatic cancer. However, this pain is quite common and can be caused by other issues as well.
- Unintended weight loss and poor appetite: Unintentional weight loss is very common in those with pancreatic cancer. Patients often lose interest in food and feel a lack of appetite.
- Nausea and vomiting: If the cancer compresses the far side of the stomach, it can obstruct the passage of food, leading to nausea, vomiting, and pain that worsens after eating, according to Step To Health.
- Enlarged gallbladder or liver: If the cancer blocks the bile ducts, bile can accumulate in the gallbladder, making it enlarge. Sometimes, a lump appears below the right side of the ribcage. Pancreatic cancer can also enlarge the liver, especially if the cancer has spread to the liver.
- Blood clots: Sometimes, the first clue that someone may have pancreatic cancer is a blood clot in a large vein, typically in the leg. However, having a blood clot doesn't necessarily mean cancer; most blood clots are caused by other factors.
- Abnormal fat tissue: Some people with pancreatic cancer develop uneven fat tissue under the skin. This is caused by the release of pancreatic enzymes that break down fat, according to Step To Health.
- Diabetes: This is rare, but pancreatic cancer can cause diabetes by damaging the insulin-producing cells. Symptoms may include increased thirst and hunger, and frequent urination.
Symptoms of pancreatic neuroendocrine tumors
Neuroendocrine tumors of the pancreas often release excess hormones into the blood. Different types of tumors produce different hormones, resulting in various symptoms, including:
- Gastritis, abdominal pain, nausea, poor appetite
- Frequent thirst, hunger, and urination.
- Diarrhea, weight loss, and malnutrition.
- Stimulation of the tongue and mouth corners, rashes.
- Symptoms of diabetes.
- Weakness, fatigue, cramps, confusion, sweating, and rapid heartbeat.
- Flushing of the face or neck, wheezing, and rapid heartbeat.
- Heart valve damage, shortness of breath, weakness, and abnormal heart sounds.
- Fainting or coma and seizures.