1. What should you do if you have menorrhagia?
Adopt a scientific lifestyle
Adjusting your lifestyle is one of the most effective ways to improve menorrhagia. Women should:
- Rest adequately, avoiding strenuous activities;
- Maintain a positive attitude, steering clear of stress;
- Sleep well and keep a regular schedule;
- Ensure proper hygiene and change sanitary products regularly.
Follow a healthy diet
A well-balanced diet can help alleviate fatigue, prevent anemia, and provide the energy needed for better health. Women should pay attention to the following:
- Incorporate more fruits and green vegetables into your meals to stabilize blood sugar, balance hormones, and reduce infections;
- Include fatty fish in your diet to reduce pain and inflammation;
- Increase the intake of iron and vitamin B6 to improve anemia;
- Eat more whole grains as they have a low glycemic index that helps balance hormones;
- Avoid stimulants like alcohol, beer, and coffee;
- Refrain from spicy and hot foods like those with excessive chili or pepper.
Consult a gynecologist
Visiting a gynecologist is crucial when experiencing menorrhagia. The doctor will diagnose the exact cause and recommend the most effective treatment to address the issue, preventing serious complications that could affect health and fertility.

2. Diagnosis of Menorrhagia
To accurately diagnose the condition and the underlying cause of menorrhagia, it is necessary to gather detailed medical history (both personal and familial), perform a physical examination, and conduct blood tests if anemia is suspected.
Subsequently, patients may be recommended for additional tests to enhance the diagnostic accuracy. These tests include:
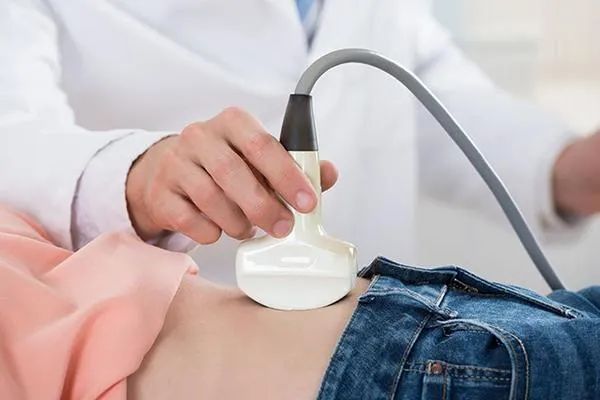
- Ultrasound: Uses sound waves to capture images of the uterus, ovaries, and pelvic area;
- PAP Test: A small sample of cells is taken from the cervix to check for infections, cancerous cells, or precursors to cancer;
- Endometrial Biopsy: A tissue sample is taken from the uterine lining to detect cancer cells.
- Laparoscopy: A small incision is made to examine the abdominal cavity.
- Hysteroscopy: A camera-equipped scope is inserted into the uterus for a visual examination.
- Hysterosalpingography: A contrast dye is injected into the uterus and fallopian tubes to visualize the uterus through X-rays.
3. Treatment of Menorrhagia
The approach to treating menorrhagia depends on two primary factors: the underlying cause and the woman’s desire to have children.
Typically, doctors will prescribe medications to address menorrhagia. This could include birth control pills, pain relievers, nonsteroidal anti-inflammatory drugs (NSAIDs), Progesterone hormone supplements, or iron supplements to prevent anemia. If medication does not yield results, surgery may be recommended.
Surgical treatments can include dilation and curettage, endometrial ablation, or even a hysterectomy (which involves removal of both the uterus and cervix). However, these procedures carry the risk of infertility, making them more appropriate for older women or those who no longer wish to conceive.
Since each individual's condition is unique, and causes vary, women who suspect they have this condition should seek immediate consultation at a reputable Obstetrics and Gynecology facility to confirm the cause and receive a personalized treatment plan.

4. Will Menorrhagia Resolve on Its Own?
Case 1: Physiological Menorrhagia
Physiological menorrhagia (also known as functional menorrhagia) commonly occurs during certain life stages, such as early adolescence, post-childbirth, or perimenopause. During these phases, hormonal fluctuations in women, combined with physiological changes, can lead to an imbalance in the reproductive system. Therefore, it is not surprising when irregular or prolonged periods occur during these times.
Additionally, menorrhagia can be triggered by the use of contraceptive pills, especially emergency contraceptives, following an abortion or miscarriage, prolonged stress at work, or an unhealthy lifestyle.
Functional menorrhagia may resolve on its own if the body's systems return to balance, usually within a few months to a few years, depending on the individual's phase of life and lifestyle. However, to gain a clearer understanding of their current condition, women are encouraged to consult a specialist for an examination and advice. Furthermore, adopting a healthy lifestyle can help minimize discomfort during episodes of menorrhagia.
Case 2: Menorrhagia Caused by Medical Conditions
In addition to physiological causes, menorrhagia due to medical conditions (organic causes) is also common, though not everyone recognizes it, leading to neglect of health protection. In these cases, menorrhagia arises from issues with the uterus or ovaries, such as uterine polyps, fibroids, endometriosis, ovarian cysts, or polycystic ovary syndrome. Other medical conditions, like hypothyroidism, bleeding disorders, and chronic hepatitis, can also contribute to the condition.
Therefore, if you are wondering whether menorrhagia will resolve on its own, it is important to note that menorrhagia due to medical conditions will not improve without medical intervention. Worse, if left untreated, it can lead to severe complications affecting both general and reproductive health. Finding the exact cause is crucial for effective treatment, so patients should not delay in seeking medical help as soon as possible.


5. Herbal Remedies for Treating Menorrhagia
Treating Menorrhagia with Cinnamon
Cinnamon is a commonly used ingredient in many dishes. It helps purify the blood and improves circulation, which in turn alleviates menstrual cramps. Women can use cinnamon to treat menorrhagia in the following ways:
- Mix 1 teaspoon of cinnamon powder with cold water. Drink it 3 times a day to reduce blood loss caused by menorrhagia.
- You can also purchase cinnamon tea bags and drink it daily as a substitute for water. It has a similar effect as the previous method. Adding a bit of honey will enhance the flavor.
- For the best results, it is recommended to start using cinnamon a week before your menstrual cycle begins.
Treating Menorrhagia with Ginger
Ginger is a common food item in most households. According to Traditional Chinese Medicine, ginger has beneficial effects on the spleen, stomach, lungs, large intestine, and kidneys. It helps fight coldness, warms the body, stimulates circulation, and revives the body’s energy. Ginger is commonly used to treat various ailments, including menorrhagia.
To treat menorrhagia effectively with ginger, women can add ginger to their daily meals or brew ginger tea and drink it 4 times a day before their menstrual cycle to enhance its effectiveness.
Home Treatment for Prolonged Menorrhagia with Vitex
Vitex is a medicinal herb known for its positive effects on the uterus, cardiovascular system, and blood pressure, as well as its anti-inflammatory properties. In traditional medicine, Vitex is used in treatments for menorrhagia, irregular periods, and menstrual cramps.
To treat menorrhagia with Vitex, follow these steps:
- Combine Vitex with other herbs such as mugwort, Dong Quai, and cyperus (about 12g of each herb).
- After cleaning the herbs, simmer them in water and drink the tea twice a day. This is a simple yet effective home remedy for menorrhagia.
Amaranth
Amaranth is a common vegetable in Vietnamese cuisine. It has cooling properties and is known for its ability to clear heat, promote urination, treat kidney disorders, regulate menstruation, and alleviate dysentery.
Here’s how to treat menorrhagia with Amaranth:
- Include Amaranth in your daily meals.
- Alternatively, boil Amaranth and drink the extract, which is very effective in treating menorrhagia.

6. What is Menorrhagia?
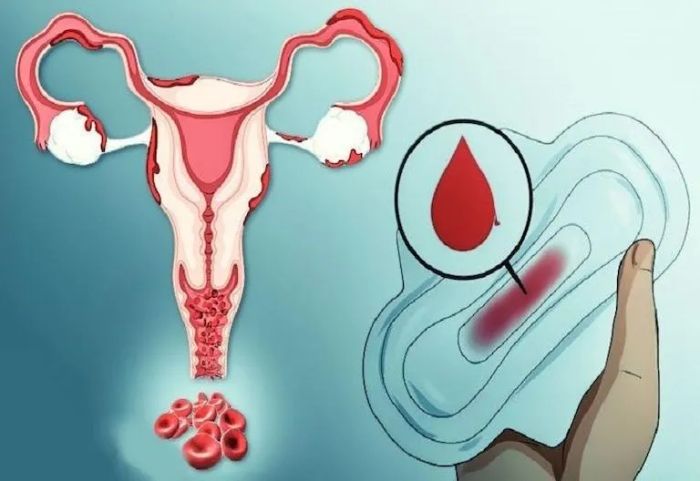
Menorrhagia (also known as Menorrhagia in English) refers to the condition where menstrual blood flow is excessive or lasts longer than a typical cycle. Normally, a menstrual cycle lasts 28-32 days, with menstruation occurring for 3-5 days. The average menstrual blood volume is around 50-80ml, which is the shedding of the uterine lining. Following this, a new uterine lining forms for the next cycle.
When the menstrual period exceeds 7 days or the blood loss exceeds 80ml, it is classified as menorrhagia. To assess whether menstrual blood loss is excessive, women can monitor the number of sanitary pads used and the frequency of changes. If a pad needs to be changed every few hours or more than two pads are used simultaneously, it is an indication of excessive bleeding.
Additionally, if there is heavy bleeding at night or the blood clots into large masses, this could also signal menorrhagia. Prolonged menorrhagia can result in anemia, fatigue, and pallor. More dangerously, this condition can facilitate bacterial growth, leading to infections in the reproductive organs, increased risk of gynecological diseases, and infertility in women.

7. What Causes Menorrhagia?
Menorrhagia can result from various factors, including hormonal imbalances, underlying health conditions, or even stress. Below are the most common causes:
Hormonal Imbalance
The balance between Estrogen and Progesterone in women regulates the buildup and shedding of the uterine lining during the menstrual cycle. If there is a deficiency or imbalance in any hormone, the uterine lining may grow excessively, leading to heavy menstrual bleeding.
Conditions that can disrupt hormone balance in women include polycystic ovary syndrome (PCOS), thyroid disorders, obesity, insulin resistance, and more.
Ovarian Dysfunction
If ovulation does not occur during the menstrual cycle, the body fails to produce Progesterone as would happen in a normal cycle, resulting in hormonal imbalance and, consequently, menorrhagia.
Other potential causes include:
- Uterine Fibroids: These benign growths can contribute to longer menstrual periods.
- Endometriosis: The presence of endometrial tissue outside the uterus can lead to pain and increased bleeding.
- Uterine Polyps: Small benign growths on the uterine lining can also result in prolonged bleeding.
- Intrauterine Devices (IUD): Menorrhagia is a common side effect of IUDs used for birth control.
- Pregnancy-related Issues: Miscarriage (fetal death in the womb) or ectopic pregnancies can cause abnormal bleeding.
- Medications: Certain drugs, such as anti-inflammatory drugs, blood thinners, and hormonal medications, can lead to extended menstrual bleeding.
- Other Health Conditions: Genetic blood clotting disorders like Von Willebrand disease and cancers such as cervical, uterine, or ovarian cancer can contribute to menorrhagia.
8. Is Menorrhagia Dangerous?
When menstrual bleeding lasts too long or becomes excessive without proper treatment, it can lead to the following complications:
- Prolonged menstrual bleeding causes significant blood loss, leading to anemia. Symptoms of anemia may include shortness of breath, fatigue, pale skin, and a lack of energy.
- Severe abdominal pain: In addition to excessive bleeding, women may experience intense abdominal pain (similar to menstrual cramps). In some cases, cramps are associated with prolonged bleeding.
- The ongoing bleeding creates an environment that allows bacteria to invade, resulting in genital infections. Bacteria may travel upward from the vulva into the vagina, uterus, or fallopian tubes, leading to pelvic inflammatory disease or even infertility later in life.
- Prolonged bleeding can significantly disrupt daily activities, leaving women feeling constantly uncomfortable or even fearful when their period arrives.
- Excessive menstrual bleeding can also be a symptom of various gynecological disorders, such as uterine fibroids, polyps, endometrial infections, or polycystic ovary syndrome. If untreated, these conditions can lead to severe complications.

