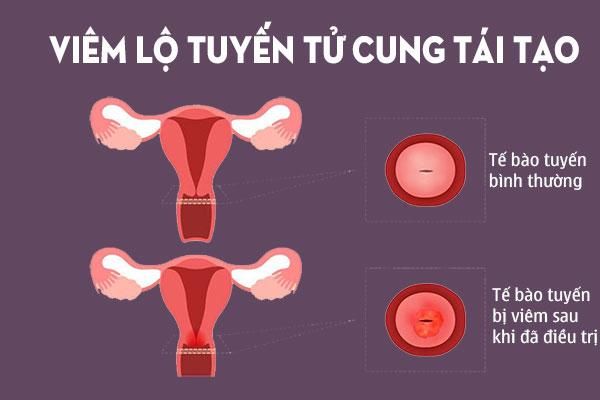
1. Cervicitis
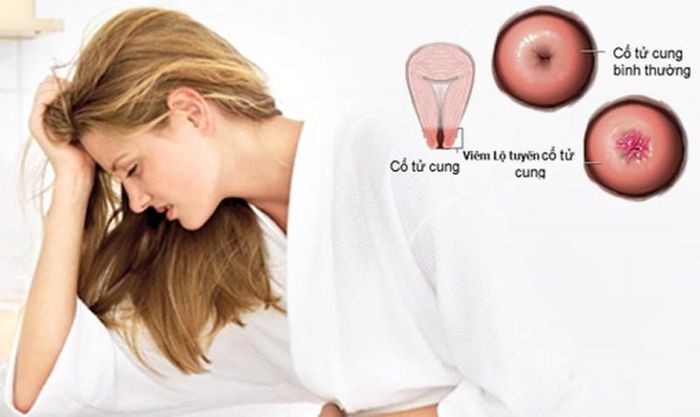
Cervicitis is a condition characterized by symptoms such as bleeding between menstrual cycles, pain during intercourse, and abnormal vaginal discharge. However, some cases show no symptoms at all. It is essential to identify the cause of cervicitis, as untreated infections can spread to the uterus, fallopian tubes, and pelvic cavity, leading to life-threatening infections and affecting future fertility and pregnancies.
The cervix acts as a barrier to prevent bacteria and viruses from entering the uterus. When infected, the risk of other infections spreading to the uterus increases. Gonorrhea or chlamydia-induced cervicitis can spread to the uterine lining and fallopian tubes, resulting in pelvic inflammatory disease (PID), which may cause reproductive problems if left untreated. Cervicitis can also increase the risk of women contracting HIV from an infected partner.
Causes:
- Poor personal hygiene, especially not cleaning the genital area before and after intercourse or during menstruation, creates favorable conditions for pathogens to enter the vagina and move upwards to the cervix, causing infection.
- Deep vaginal douching and using high-alkaline soaps or cleaning solutions can disrupt the vaginal balance, making it easier for bacteria to invade.
- Procedures like abortion, genital cosmetic surgery, or IUD insertion performed by inadequately trained medical professionals using unsterile instruments.
Symptoms:
- Unusual vaginal discharge.
- Frequent, painful urination.
- Pain during intercourse.
- Bleeding between menstrual cycles.
- Vaginal bleeding after intercourse unrelated to menstruation.
Treatment and Prevention:
- Cervicitis can also arise from improper hygiene practices. To reduce the risk of infection, women should maintain proper hygiene and use appropriate cleaning products correctly.
- If cervicitis is caused by sexually transmitted infections, doctors will prescribe antibiotics to treat the infection. If caused by a virus (such as genital herpes), antiviral medications are typically prescribed.
- It is also important to test and treat your partner, regardless of whether they show symptoms.

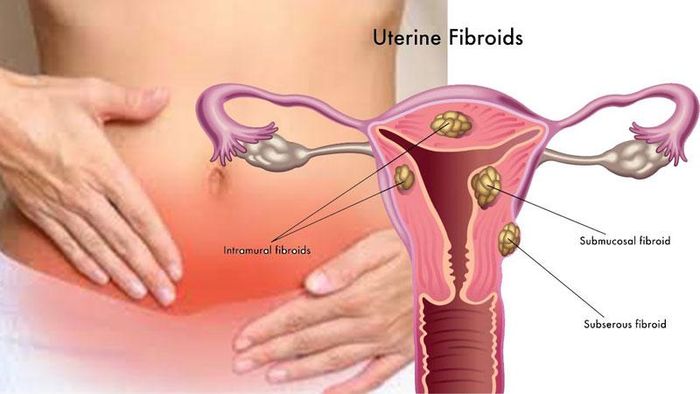
2. Uterine Fibroids
Uterine fibroids are common gynecological conditions that can occur at any age, especially in women during their reproductive years, pregnancy, or menopause. These are abnormal growths that develop from the uterine muscle. Fibroids can be located under the serosa, in the endometrium, within the muscle layer, or even outside the uterus. Despite extensive research, the exact cause of fibroids remains unclear, although factors such as excessive estrogen production, hormonal imbalances, and obesity are believed to increase the risk of developing them.
In all cases, women with uterine fibroids should undergo regular screenings, including ultrasound, to monitor the growth of the fibroids. Do not ignore the need for routine check-ups just because the fibroids are not causing discomfort, as they can silently increase in size and number. If left untreated, large fibroids can become dangerous and may pose serious risks to health. However, the likelihood of fibroids turning cancerous is extremely rare, as fibroids are typically benign. Nonetheless, early detection and treatment are essential to manage and prevent complications.
Causes:
- Most experts believe that fibroids develop due to hormonal imbalances, particularly an excess of estrogen.
- Genetics: There is a higher risk for women who have a family history of uterine fibroids, particularly if their mother or sisters have had them.
- Obesity: Women who are overweight, especially in middle age, are at a higher risk of developing fibroids.
- Early menstruation (before 12 years old) may also increase the risk of fibroids.
- Having early sexual activity after abortion or childbirth can lead to uterine injury, which may contribute to the development of fibroids.
- Long-term untreated gynecological infections may also contribute to fibroid development as the uterine lining becomes overgrown.
- Chronic stress can also play a role in increasing the likelihood of fibroids.
Symptoms:
- Irregular menstrual cycles, prolonged periods.
- Back pain, lower abdominal pain, or pain in the pelvic area.
- Frequent, painful urination.
- Abnormal vaginal discharge due to irritation of the uterine lining, clear and sometimes watery.
- Fibroids may be felt as a firm mass in the lower abdomen.
- Additional symptoms may include pain during intercourse, constipation, itching in the genital area, and burning sensations in the lower back.
Treatment and Prevention:
- Maintain good hygiene, especially during menstruation, and before and after sexual activity.
- If symptoms of fibroids appear, seek medical attention promptly for early diagnosis and treatment.
- Avoid spicy, fatty foods, sweets, alcohol, and stimulants.
- Maintain a balanced lifestyle, including regular rest, avoiding late nights, and managing stress to preserve health.

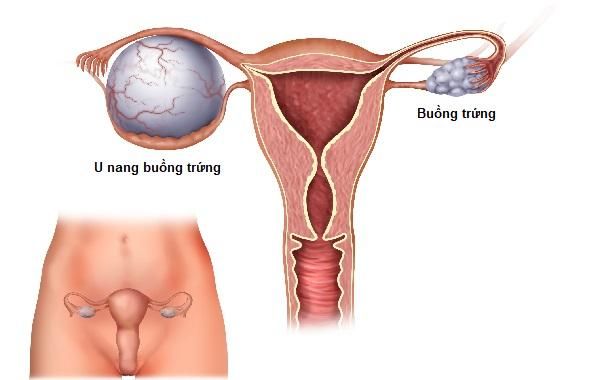
3. Ovarian Cysts
Ovarian cysts are fluid-filled or solid masses that form abnormally on or inside the ovaries. These cysts can develop from ovarian tissue, making up about 3.6% of all gynecological conditions. Ovarian cysts come in various types, and 90% are benign (unlikely to cause cancer), while 10% may develop into cancer. Women approaching menopause are at a higher risk of cancerous ovarian cysts compared to those in their reproductive years. Often, ovarian cysts grow silently with vague or no symptoms, sometimes resolving on their own without causing harm.
Causes:
- Functional cysts can result from hormonal imbalances or medications that support ovulation.
- Women with endometriosis may be more likely to develop ovarian cysts.
- Some cysts naturally form during early pregnancy to support the fetus until the placenta develops, though they may persist throughout pregnancy.
- Pelvic infections can spread to the ovaries and fallopian tubes, potentially leading to abscess formation.
Symptoms:
- Feeling of heaviness, fullness, or pressure in the lower abdomen.
- Pelvic pain.
- Lower back pain.
- Difficulties with urination and bowel movements.
- Pain during sexual intercourse.
- Unexplained weight gain.
- Painful menstrual cycles.
- Abnormal vaginal bleeding.
- Sore or swollen breasts.
- Frequent urination.
Treatment and Prevention:
- For functional ovarian cysts, no treatment is required; regular monitoring over 3-6 menstrual cycles is recommended, as these cysts typically resolve on their own.
- For persistent or complex cysts, surgical removal may be necessary to avoid complications or potential malignancy.
- Consume foods that support overall health while avoiding high-fat animal products, saturated fats, stimulants, and excessive protein. Include more vegetables, fruits, whole grains, and foods rich in vitamins A, C, and fiber in your diet. Drink 1.5-2 liters of water daily to stay hydrated.
- Enhance liver detoxification processes.
- Monitor thyroid function regularly.
- Maintain a balanced lifestyle with appropriate rest, and engage in light exercise to improve physical resilience and immune function.

4. Endometritis
Endometritis refers to the infection of the endometrial lining inside the uterus. The endometrium is a soft, spongy tissue that prepares to receive a fertilized egg and supports its development into an embryo. If no fertilization occurs, the tissue is shed during menstruation.
If left untreated, endometritis can lead to severe complications, such as sepsis, adhesions in the uterus, pelvic inflammatory disease causing blocked fallopian tubes, and ultimately infertility, where sperm cannot meet the egg, or the fertilized egg cannot implant in the uterus.
Causes:
- Endometritis is typically caused by infections or sexually transmitted diseases (STIs) such as Chlamydia, gonorrhea, tuberculosis, staphylococcal, and streptococcal infections. It may also be caused by bacteria migrating from lower reproductive organs after cervicitis or vaginitis.
- Infections may follow complications from childbirth, including retained placenta, prolonged labor, unsterilized surgical instruments, or infections after a cesarean section.
- Poor hygiene or unprotected sex are also potential causes.
Symptoms:
- Severe lower abdominal pain during or before menstruation, painful intercourse.
- Fatigue and painful urination.
- Digestive issues, including diarrhea, constipation, or vomiting.
- Frequent allergic reactions and recurrent vaginal infections.
- Excessive vaginal discharge with pus, fever.
Treatment and Prevention:
- To diagnose endometritis, a doctor will conduct a clinical examination, palpating the abdomen, uterus, and cervix. They may also perform diagnostic tests, such as culturing uterine tissue to detect infectious bacteria, endometrial biopsy, laparoscopy, blood tests (to check white blood cell count and erythrocyte sedimentation rate).
- Practice safe sex, get regular check-ups, and follow the prescribed treatment for STIs as advised by a doctor.
- Maintain proper genital hygiene daily.
- Adopt a balanced diet and lifestyle, avoid spicy, oily foods, and ensure adequate rest.


5. Pelvic Inflammatory Disease (PID)
Pelvic Inflammatory Disease (PID) is a common infection affecting the female reproductive organs, often caused by sexually transmitted infections (STIs). It is a widespread condition, with over a million women diagnosed annually in the United States. PID occurs when bacteria from the vagina and cervix ascend into the uterus, ovaries, or fallopian tubes. These bacteria can cause abscesses in the fallopian tubes or ovaries. Without timely treatment, PID can lead to long-term complications.
Research indicates that frequent vaginal douching increases the risk of PID. Douching not only promotes bacterial growth but can also push harmful bacteria into the uterus and fallopian tubes. As a result, doctors generally advise against douching. While PID can be treated, any scarring caused by the infection is permanent. If left untreated, the risk of further complications, including infertility, increases.
Causes:
- Unprotected sexual intercourse is one of the leading causes of PID.
- Poor personal hygiene that allows bacteria and viruses to enter the reproductive system.
- Using low-quality sanitary products, or having sex during menstruation without changing sanitary pads frequently can promote bacterial infections.
- Infections resulting from abortion procedures or childbirth.
- Failure to properly treat gynecological infections.
Symptoms:
- Abnormal vaginal discharge.
- Lower abdominal pain (usually mild).
- Upper right abdominal pain.
- Irregular menstrual bleeding.
- Fever and chills.
- Painful urination.
- Nausea and vomiting.
- Discomfort during intercourse.
Treatment and Prevention:
- Treatment for PID typically begins with oral antibiotics or intravenous antibiotics prescribed by a doctor.
- To prevent PID, use condoms during sexual activity to protect against sexually transmitted diseases. Condoms should still be used even if other contraceptive methods are in place. Limit the number of sexual partners and only engage with those who have no STDs.

6. Vaginitis
Vaginitis refers to inflammation of the vagina caused by infections from fungi, trichomonas, or bacteria, leading to abnormal and uncomfortable symptoms. Statistically, one-third of women will experience symptoms of vaginitis at some point in their life. It can affect women of all ages, but it is most common during the reproductive years. In young children, vaginitis is often linked to the bacterial flora of the digestive tract (non-specific vulvovaginitis). A contributing factor in girls aged 2 to 6 is poor hygiene practices (e.g., wiping from back to front after defecation, not washing hands after using the toilet, or frequently touching the genital area, especially when itchy). For women of reproductive age, healthy bacteria are the dominant microbes in the vaginal environment, maintaining the pH level (3.8 to 4.2), preventing the overgrowth of harmful bacteria. Additionally, higher estrogen levels support vaginal epithelial thickness, strengthening local defense mechanisms. Postmenopausal women experience a decrease in estrogen, thinning the vaginal epithelium and increasing susceptibility to infections. Certain treatments (such as ovarian removal, pelvic radiation, and chemotherapy) can also lower estrogen, leading to vaginal atrophy. Reduced estrogen levels can cause a more alkaline pH, fostering bacterial overgrowth that can lead to vaginal disease.
Causes:
- An imbalance in the yeast and bacteria living in the vagina, leading to inflammation of the vaginal lining.
- Unsafe sexual practices, multiple sexual partners with infections, or rough intercourse causing damage to the genital area can increase the risk of vaginitis.
- Frequent abortions or surgical procedures like unsafe IUD insertions may also cause vaginal and cervical trauma, leading to vaginitis.
Symptoms:
- Itching, swelling, and burning sensations in the vulva and vagina.
- White, clumpy discharge resembling cottage cheese, often increasing before menstruation.
- Painful intercourse.
- Frequent painful urination.
- Visual inspection may show white patches inside the vaginal walls or cloudy discharge resembling rice water.
Treatment and Prevention:
- Maintain proper hygiene, especially after sexual activity and menstruation.
- Consult a reputable healthcare facility for a proper diagnosis. After an assessment, the doctor will recommend the most effective treatment based on the causative agent and disease severity.


7. Menstrual Disorders
Menstrual disorders or discomfort experienced during the menstrual cycle are common issues for all women. These disorders vary widely, from menstrual cramps (dysmenorrhea) to heavy bleeding, irregular cycles, and even missed periods. Such menstrual irregularities can lead to significant discomfort and may reduce fertility.
Menstrual disorders refer to abnormal patterns in the menstrual cycle, including irregular periods, changes in the number of days or the amount of menstrual flow compared to previous cycles. These changes might indicate an underlying medical condition, hormonal imbalance, or even be linked to lifestyle changes. They can affect women at different life stages, such as adolescence, post-pregnancy, or menopause, and can directly impact overall health, sexual function, and reproductive ability if not treated promptly.
Causes:
- Pregnancy or breastfeeding: Missed periods may indicate pregnancy. After childbirth, menstruation may temporarily stop. Eating disorders, significant weight loss, or excessive physical activity can also cause menstrual disturbances.
- Polycystic Ovary Syndrome (PCOS): Women with this hormonal imbalance often experience irregular cycles and may have enlarged ovaries filled with numerous cysts visible on ultrasound.
- Premature Ovarian Failure: This condition occurs when the ovaries lose function before age 40, leading to irregular or absent periods over several years.
- Pelvic Inflammatory Disease (PID): This infection of the reproductive organs can cause irregular bleeding.
- Uterine Fibroids: Benign tumors in the uterus can result in heavy or prolonged menstrual bleeding.
Symptoms:
- PMS (Premenstrual Syndrome): Occurs 1-2 weeks before the period starts, with symptoms such as bloating, irritability, back pain, headaches, breast tenderness, acne, increased appetite, excessive fatigue, mood swings, anxiety, stress, insomnia, constipation, diarrhea, and mild abdominal pain.
- Menorrhagia: Heavy bleeding during menstruation, often lasting longer than usual (5-7 days).
- Amenorrhea: The absence of menstruation. Primary amenorrhea is the failure to start menstruation by age 16, possibly due to pituitary gland issues, congenital reproductive tract anomalies, or delayed puberty. Secondary amenorrhea refers to the absence of menstruation for more than six months after a normal cycle.
Treatment and Prevention:
- Adjusting your diet 14 days before your period may help manage mild menstrual irregularities.
- Reducing salt intake (sodium) can alleviate bloating. Limiting caffeine, sugar, and alcohol can also help.
- Getting adequate rest to reduce stress, particularly after intense academic work, helps balance your body’s hormonal function.
- Regular exercise improves overall health and can enhance the effectiveness of academic pursuits for young women.


8. Cervical Erosion
Cervical erosion is a condition where the glandular cells of the cervix grow excessively. These cells, which are normally found inside the cervical canal, now extend outward and invade the surface of the cervix. These cells continue to secrete fluids as usual, causing the vagina to emit a foul odor. This is known as cervical erosion.
Cervical erosion is a benign condition where glandular cells within the cervix invade the outer surface. Women with this condition often experience increased vaginal discharge, itching, and foul-smelling discharge, which can lead to infections (referred to as cervical erosion). The condition may not present noticeable symptoms, and patients often only discover it during gynecological examinations. Some women are born with cervical erosion, while others develop it due to birth control usage or during pregnancy. The condition is treatable but traditional methods may not fully resolve it.
Causes:
- Improper hygiene can easily lead to genital infections, including cervical erosion. Overuse of feminine hygiene products or douching can damage the vaginal area, increasing the risk of cervical erosion.
- Unsafe practices like abortions, genital cosmetic surgery, IUD insertion, or hymenoplasty may elevate the risk of developing cervical erosion.
- Unprotected sex can expose women to infections, including sexually transmitted diseases, which can also increase the risk of cervical erosion.
Symptoms:
- Discharge may have a foul, fishy smell, causing discomfort for the patient. In severe cases, the discharge may appear clumpy or curdled like yogurt, significantly affecting daily life and well-being.
- Increased discharge, coupled with poor hygiene, often causes itching and discomfort. Scratching the affected area can worsen the condition and spread the infection.
- Menstrual blood may turn dark brown or reddish-brown due to stagnation in the uterus. Infection can also cause clotting, making it difficult for menstrual blood to exit the body.
- During sexual intercourse, especially rough sex, small amounts of blood may be noticed. This is due to the cervical erosion being irritated by pressure from penetration.
Treatment and Prevention:
- Common treatments include cauterization, laser therapy, or cryotherapy. These methods are quick and yield clear results.
- If the condition is still in its early stages, antibiotics (both oral and topical) prescribed by a doctor can help eliminate harmful bacteria in the vaginal area.
- To prevent cervical erosion and other gynecological conditions, maintain a balanced vaginal pH, visit a gynecologist regularly, ensure proper hygiene, avoid douching, keep the area clean and dry, wear cotton underwear, and change it regularly.