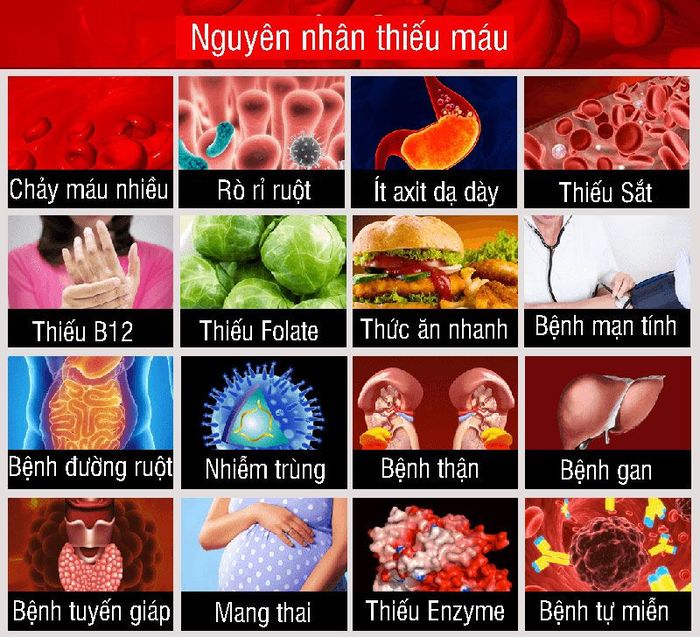
1. Factors That Increase the Risk of Anemia
Factors that increase the risk of developing anemia include:
- A diet lacking essential vitamins and minerals: Insufficient intake of iron, vitamin B12, and folate raises the risk of anemia.
- Intestinal disorders: Conditions like Crohn's disease and celiac disease, which impair nutrient absorption in the small intestine, increase the likelihood of anemia.
- Menstruation: Women who have not reached menopause are at higher risk of iron-deficiency anemia compared to men and postmenopausal women due to blood loss during menstruation.
- Pregnancy: Pregnant women not taking multivitamins with folic acid and iron are more prone to anemia, which can persist postpartum as postpartum anemia.
- Chronic diseases: Conditions such as cancer, kidney failure, diabetes, or other chronic illnesses can elevate the risk of anemia by causing a shortage of red blood cells. Chronic blood loss from internal ulcers can also deplete iron levels, leading to iron-deficiency anemia.
- Family history: A family history of inherited anemias, like sickle cell anemia, increases your risk.
- Other factors: Certain infections, blood disorders, autoimmune diseases, alcohol addiction, exposure to toxic chemicals, and specific medications can impair red blood cell production and cause anemia.
- Age: Individuals over 65 are at a higher risk of anemia.

2. Complications of Anemia
Mild anemia is not a major concern as it can often be improved through dietary changes, increased iron intake, and vitamin supplementation. However, anemia caused by underlying medical conditions requires early treatment to prevent serious health complications that can negatively affect the functioning of vital organs.
Harmful complications caused by anemia include:
- Severe physical weakness: Patients may experience extreme fatigue, making it difficult to perform daily activities.
- Pregnancy: Pregnant women with folate-deficiency anemia are at a higher risk of premature birth.
- Heart issues: Anemia can lead to irregular heartbeats, particularly abnormally fast heart rates. This occurs because the heart pumps more blood to compensate for the lack of red blood cells, which can eventually result in congestive heart failure.
- Death: Inherited anemias can lead to life-threatening complications. Prolonged anemia can also cause significant blood loss, leading to acute anemia and potentially fatal outcomes.
3. Diagnosing Anemia
Clinically, anemia is diagnosed based on the following signs:
- Pale skin and mucous membranes
- Tinnitus, dizziness, blurred vision, and fainting
- Loss of appetite and digestive disorders
- Palpitations, fatigue, and rapid heartbeat
- Women may experience amenorrhea
Through laboratory tests, anemia is diagnosed using blood tests, folic acid/ferritin levels, and bone marrow analysis:
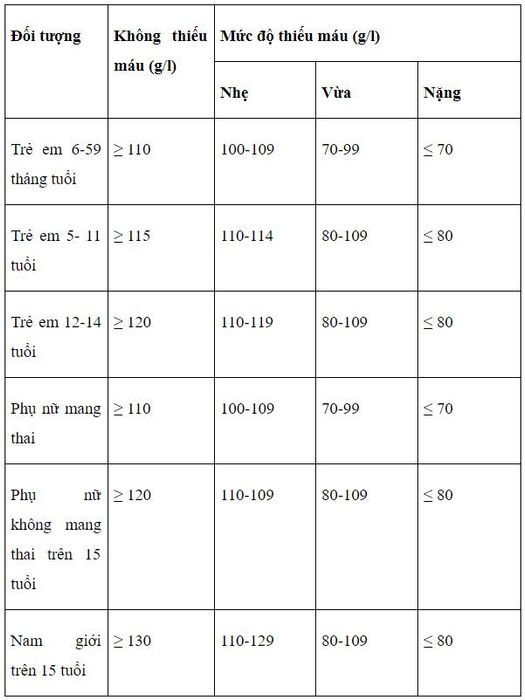
- Blood tests: Based on hemoglobin levels as follows:
- Below 13g/dl (130 g/l) for men.
- Below 12g/dl (120 g/l) for women.
- Below 11g/dl (110 g/l) for older adults.
- Decreased ferritin levels
- Reduced folic acid or vitamin B12 levels
- Decreased bone marrow production
4. Treating Anemia
Treatment for anemia depends on the underlying cause:
Anemia due to nutrient deficiencies
- Iron-deficiency anemia: Address the cause of bleeding and supplement with 2mg of elemental iron per kg/day. Blood transfusions are only necessary in severe cases.
- Folate-deficiency anemia: Address the cause of folate deficiency and supplement with 1-5mg of folic acid daily.
- Vitamin B12-deficiency anemia: Administer 1000 µg of vitamin B12 intramuscularly daily for 7 days, followed by long-term treatment of 1000 µg monthly.
Thalassemia
- Causes: Genetic abnormalities in hemoglobin chain production, leading to shorter red blood cell lifespans. Common types include Beta-Thalassemia and Alpha-Thalassemia.
- Treatment: Regular blood transfusions for moderate to severe cases. Early bone marrow transplantation from a healthy donor offers a high chance of cure.
Immune hemolytic anemia
- Causes: Abnormal antibodies attack red blood cells, causing them to rupture.
- Treatment: Corticosteroids at 1mg/kg for 4 weeks, then tapered. Immunosuppressants or bone marrow transplantation may be used in resistant cases.
Anemia due to bone marrow failure
- Causes: Bone marrow fails to produce enough blood cells due to infections, chemicals, radiation, genetics, or unknown reasons.
- Treatment: Blood transfusions, early bone marrow transplantation, or antiviral therapy if caused by a viral infection.
Anemia in chronic kidney disease
- Causes: Chronic kidney disease reduces erythropoietin production, leading to low red blood cell levels.
- Treatment: Subcutaneous erythropoietin injections at 50-150 units/kg every other day.

5. What Should You Eat if You Have Anemia?
Iron-rich foods
When planning a diet for anemia, iron-rich foods are essential since most anemia cases stem from iron deficiency. Consuming iron-rich foods not only nourishes cells better but also alleviates anemia. Examples include red meat, organ meats, mushrooms, and wood ear mushrooms.
Foods rich in B vitamins
Vitamins like B12, B9, B6, and others play a crucial role in red blood cell production and differentiation. Therefore, they are vital for those with anemia. Examples include eggs, dark leafy greens, legumes, asparagus, dairy products, salmon, tuna, nuts, and fresh fruits.
Foods rich in vitamin C
Vitamin C is excellent for preventing anemia. It also enhances iron absorption, fights inflammation, prevents infections, and aids collagen formation. Thus, it’s a must-have in an anemia-friendly diet. Examples include mangoes, oranges, kale, guava, papaya, and strawberries.
Specifically:
- Dark leafy greens: Spinach, kale, celery, betel leaves, and moringa are rich in non-heme iron, vitamin C, and folate, making iron absorption easier.
- Meats: Most meats contain heme iron, which helps the body absorb the necessary iron for red blood cell production. Examples include beef, pork, and chicken.
- Seafood: Shellfish and other seafood are rich in iron and folate, making them ideal for anemia patients. They also provide minerals like phosphorus, calcium, and zinc, which are good for bone health. Examples include shrimp, crab, oysters, sardines, and mackerel.
- Legumes: Beans are affordable and rich in vitamins and iron, making them suitable for everyone. Examples include black beans, peas, green beans, and soybeans.
- Nuts and seeds: Pumpkin seeds, sunflower seeds, and cashews are excellent sources of iron. They can be paired with salads, vegetables, or fruits for a nutrient-rich meal that boosts blood health and immunity.

6. Preventing Anemia
To prevent anemia, we should:
- Maintain a hygienic and balanced diet. Meals should be nutritious, flavorful, and free from artificial additives, flavorings, and excessive oils.
- Adopt a balanced lifestyle that combines work and physical exercise to improve overall health.
- Women should pay attention to their menstrual cycles and supplement with iron or consume iron-rich foods when deficient.
- Listen to your body and promptly identify signs of anemia or risk factors.
- Schedule annual health check-ups to detect any issues early.
While many types of anemia cannot be prevented, you can avoid iron-deficiency anemia and vitamin-deficiency anemia by consuming a diet rich in vitamins and minerals, including:
- Iron: Found in beef, other meats, lentils, iron-fortified cereals, dark leafy greens, and dried fruits.
- Folate: Present in fruits, fruit juices, dark leafy greens, green peas, kidney beans, peanuts, and fortified grain products like bread, cereal, pasta, and rice.
- Vitamin B12: Abundant in meat, dairy products, fortified cereals, and soy products.
- Vitamin C: Found in citrus fruits and juices, peppers, broccoli, tomatoes, melons, and strawberries. These also enhance iron absorption.

7. What is Anemia?
The human body has three types of blood cells:
- White blood cells to fight infections
- Platelets to help blood clot
- Red blood cells to carry oxygen throughout the body
Red blood cells contain hemoglobin, an iron-rich protein that gives blood its red color. Hemoglobin enables red blood cells to carry oxygen from the lungs to all parts of the body and transport carbon dioxide from other body parts to the lungs for exhalation.
Most blood cells, including red blood cells, are continuously produced in the bone marrow. To produce hemoglobin and red blood cells, the body requires iron, vitamin B12, folate, and other nutrients from the food you eat. Therefore, if the body has a low red blood cell count that cannot meet the demand for oxygen delivery to tissues, it results in anemia.
Anemia is a condition where the hemoglobin level and red blood cell count in peripheral blood decrease, leading to insufficient oxygen supply to the body's tissues.
There are many forms of anemia, each with its own cause. Anemia can be temporary or long-term, ranging from mild to severe. If you suspect anemia, consult a doctor as it could be a warning sign of a serious condition.
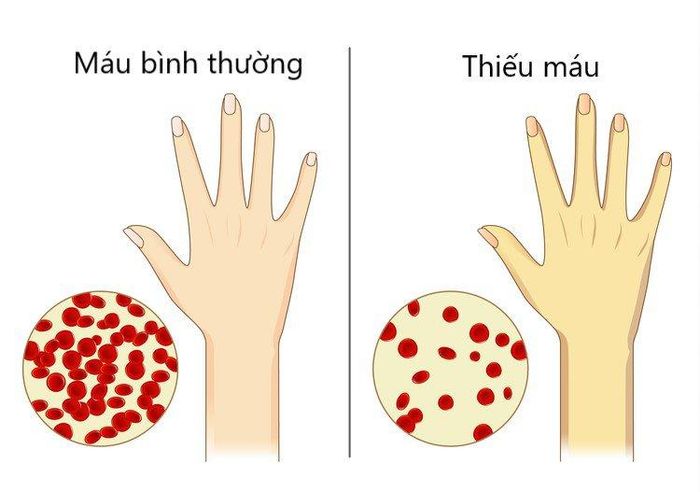
8. Symptoms of Anemia
The most common symptom of anemia is fatigue. Other common symptoms include:
- Pale skin
- Rapid or irregular heartbeat
- Shortness of breath
- Chest pain
- Headaches
Some people with anemia may also experience a loss of appetite, sleep disturbances, and difficulty breathing during physical activities. Over time, this can lead to abdominal pain and a weakened immune system.
Those with mild anemia may experience few or no symptoms. Certain types of anemia cause specific symptoms, such as:
- Aplastic anemia: May cause fever, frequent infections, and skin rashes.
- Folate-deficiency anemia: Can lead to irritability, diarrhea, and loss of appetite.
- Hemolytic anemia: May result in jaundice, dark urine, fever, and abdominal pain.
- Sickle cell anemia: Can cause painful swelling in the hands and feet, fatigue, and jaundice.
However, these symptoms can also be caused by other conditions. The only way to confirm anemia is through a series of blood tests to determine the exact levels of iron and other substances in the blood. If you suspect anemia, consult a doctor.

9. Causes of Anemia
Different types of anemia have different causes, including:
Anemia of inflammation
Certain diseases like cancer, HIV/AIDS, rheumatoid arthritis, kidney disease, Crohn's disease, and other acute or chronic inflammatory conditions can interfere with red blood cell production.
Aplastic anemia
This rare, life-threatening condition occurs when the body doesn't produce enough red blood cells. Causes include infections, certain medications, autoimmune diseases, and exposure to toxic chemicals.
Myelodysplastic anemia
Diseases like leukemia and myelofibrosis can cause anemia by affecting blood production in the bone marrow. The impact of these cancers and cancer-like disorders ranges from mild to life-threatening.
Iron-deficiency anemia
This is the most common type of anemia, caused by insufficient iron in the body. Bone marrow needs iron to produce hemoglobin, and without enough iron, the body cannot produce adequate hemoglobin for red blood cells.
This type of anemia often occurs in pregnant women or those with chronic blood loss, such as from prolonged menstruation, ulcers, cancer, or frequent use of over-the-counter pain relievers like aspirin, which can cause stomach lining inflammation and blood loss.
Vitamin-deficiency anemia
Besides iron, the body needs folate and vitamin B12 to produce enough healthy red blood cells. A diet lacking these and other essential nutrients can reduce red blood cell production.
Additionally, some people who consume enough B12 cannot absorb the vitamin, leading to vitamin-deficiency anemia, also known as pernicious anemia.
Thalassemia
This inherited blood disorder involves abnormal hemoglobin, the protein in red blood cells that carries oxygen. In thalassemia, red blood cells are destroyed excessively, leading to anemia.
Sickle cell anemia
Sickle cell anemia is a hereditary and sometimes severe form of hemolytic anemia. It is caused by a defective form of hemoglobin that makes red blood cells assume an abnormal sickle shape. These abnormal cells die prematurely, resulting in a chronic shortage of red blood cells.