1. Essential Tests

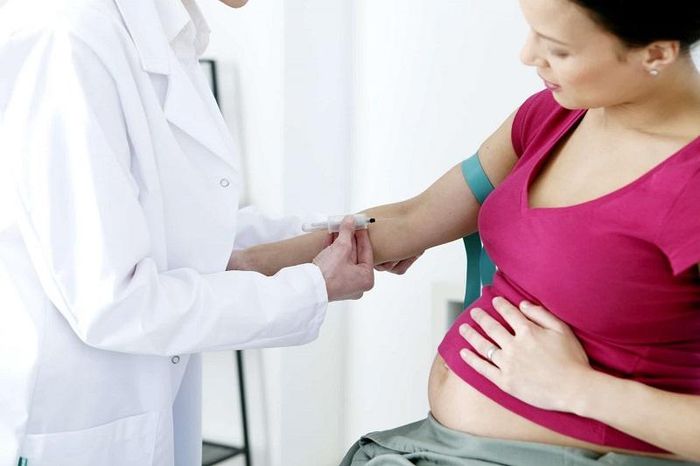
2. Tetanus Vaccination or Guidance for Tetanus Vaccination
From the very first consultation, it's essential to inquire whether the pregnant woman has immunity against tetanus and determine the need for any supplementary or initial vaccinations. If the woman hasn't had any tetanus shots yet, she should receive two doses, spaced one month apart, with the second dose at least 30 days before the expected delivery date. For women who have had two doses during a previous pregnancy, an additional dose should be recommended. If the woman received three childhood tetanus vaccinations as part of her extended immunization, she should also be advised to take an additional dose.
According to medical professionals, tetanus vaccination for pregnant women is crucial as it helps the mother generate antibodies in advance, preventing infection during labor. Furthermore, this vaccination protects the baby by reducing the risk of post-delivery tetanus infection. The tetanus vaccine for pregnant women has been proven safe for both mother and child, with no negative impact on the fetus, ensuring the health of both. Therefore, pregnant women should not be overly worried but should follow the vaccination guidelines as prescribed.
3. Health education, guidance on prenatal hygiene
This is a crucial step in the process of prenatal checkups. Health education and prenatal hygiene guidance should be provided at every prenatal visit. Healthcare providers should actively engage with the pregnant woman, offering answers, explanations, and addressing any questions she may have. Education and counseling for women before and during pregnancy equip the expectant mother with the necessary preparation, including potential risks for both mother and baby, important preventive measures, and steps to take during pregnancy.
Education and counseling must not be limited to one session but should occur multiple times throughout the pregnancy. Topics covered in pre-pregnancy education include basic knowledge about congenital disabilities, personal and family medical history, medications used before and during pregnancy, recommended vaccinations prior to pregnancy, prenatal care advice, nutrition, work routines, hygiene practices, and other aspects of living during pregnancy...


4. Provision of essential medications
During pregnancy, the mother’s body requires increased nutrients to meet both her needs and to adequately support the developing fetus. However, simply following a regular diet, especially for those experiencing severe morning sickness, may not provide sufficient nutrition. Typically, doctors recommend additional supplements and minerals such as iron, calcium, and folic acid. Depending on the individual's health condition, supplementation requirements will vary. During prenatal checkups, the doctor will assess and prescribe appropriate dosages.
In areas affected by malaria, malaria prevention medication should be given to pregnant women according to the malaria control protocols. Iodine-containing medications should be provided to regions with high rates of goiter, in line with the iodine deficiency prevention guidelines. To prevent anemia in both the mother and fetus, all pregnant women should be given iron/folic supplements throughout pregnancy and for one month postpartum. Additionally, pregnant women should consume DHA-rich foods regularly during pregnancy, such as seaweed, salmon oil, tuna oil, chicken, egg yolks, and fish liver oil.


5. Recordkeeping and medical examination slips
Record the pregnancy check-up logs, examination slips, or appointment slips in a folder or bag labeled with the month for the next scheduled visit. Create a "shrimp" chart to stick on the monitoring board with the expected delivery month of the expectant mother, starting from the first check-up. This step is crucial and should not be overlooked during the prenatal check-up process, as these records allow the doctor to track the health status of both the mother and the baby throughout the pregnancy.
Additionally, based on the information from each check-up, the doctor will advise the mother on the proper care and rest plan to ensure the best health as she prepares for the birth of her child. If the mother shows any abnormal symptoms during pregnancy, the doctor will take timely action. The logbook also includes space for family members to record the child's developmental milestones and provides vital information on caring for expectant mothers and infants. The logbook serves as an ongoing tool for maternal and child health management, from pregnancy until the child turns six and is ready for school.


6. Reporting results and scheduling follow-up appointments
This is the final step in the prenatal check-up process. After completing the previous steps, the doctor will inform the expectant mother of the examination results and provide an update on the health status of both mother and baby. If any irregularities are found, the doctor will offer advice and solutions to address the issues. If everything is stable, the doctor will schedule the next visit, allowing the mother to plan accordingly around her time and work commitments.
Furthermore, doctors will emphasize the key message: Pregnant women should have at least three check-ups during the three trimesters: the first, second, and third trimesters. If possible, it is advised to have at least two check-ups in the third trimester. If any unusual symptoms occur, immediate consultation is necessary.

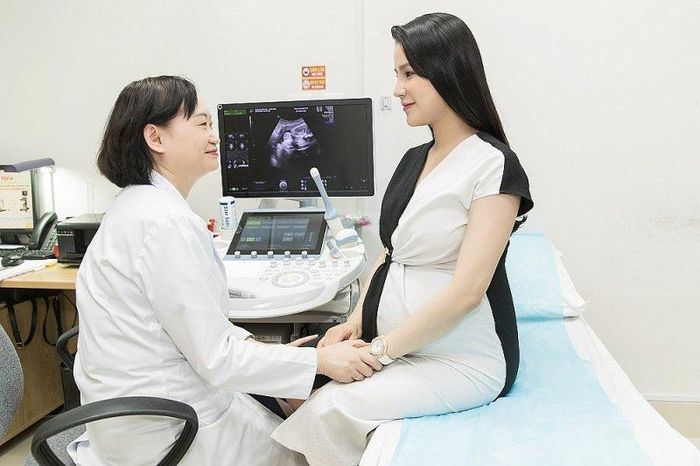
7. Hỏi
Trong suốt quá trình mang thai, mẹ bầu thường xuyên phải khám thai để nắm bắt tình hình sức khỏe của cả hai mẹ con. Mỗi lần khám thai sẽ là khác nhau nhưng hầu như đều cần trải qua các bước khám thai chuẩn để cho kết quả chính xác nhất. Hỏi thông tin - Đây là bước đầu tiên và không thể bỏ qua trong quy trình các bước khám thai chuẩn. Có nhiều mẹ cho rằng bước này không cần thiết, cứ vào khám thôi nhưng thật ra nó khá quan trọng. Bác sĩ cần hỏi những thông tin cần thiết để có những chẩn đoán ban đầu và quyết định nên khám gì, làm xét nghiệm gì cho chính xác. Tùy vào thời gian mang thai, mẹ bầu sẽ được hỏi những câu hỏi khác nhau.
Mang thai 3 tháng đầu: Bác sĩ sẽ hỏi mẹ các thông tin cá nhân như tên, tuổi, gia đình… Sau đó, mẹ sẽ được hỏi về các dấu hiệu thai nghén, tình hình sức khỏe hiện tại, các dấu hiệu bất thường và hỏi tiền sử bệnh tật trước đó… Mang thai 3 tháng giữa: Lúc này, mẹ sẽ được bác sĩ hỏi han về hiện tượng thai máy, về những thay đổi hay những dấu hiệu bất thường của cơ thể cũng như được hỏi về tình hình phát triển cân nặng của mẹ và những loại thuốc mẹ đang sử dụng… Mang thai 3 tháng cuối: Giai đoạn này, ở những lần khám thai, bác sĩ sẽ hỏi mẹ về thai máy, tình hình sức khỏe của mẹ và hỏi xem có xuất hiện triệu chứng cơ năng nào hay không…


8. Full-body examination
After gathering basic information in the first step, the pregnant woman will undergo a full-body examination. The doctor will assess her height, weight, heart rate, and blood pressure. Once the measurements are taken, the doctor will check for any abnormal signs, such as rapid or slow weight gain, and provide advice on diet and physical activity to maintain a healthy weight. If necessary, timely intervention will be recommended.
During the prenatal check-up, the expectant mother will have her height and weight measured, and her weight will be monitored monthly. If there is an increase of more than 2 kg per month or 500 grams within a week, there may be a risk of edema or water retention. The doctor will also check the pulse and blood pressure, which may rise by 10 to 15 beats per minute, but normally there should be no significant change in blood pressure during pregnancy. Additionally, the doctor will examine the heart and lungs, chest, and abdomen to check for any lumps or abnormalities.


9. Obstetric examination
Among the various steps in prenatal care, obstetric examination is a critical procedure that should not be skipped. This examination enables doctors to gather necessary information about both the mother and the baby, such as checking for any old surgical scars, measuring the height of the uterus, listening to the fetal heartbeat, and more. Additionally, the obstetric check-up helps identify any gynecological infections, enabling timely and effective treatment to minimize complications that could affect the baby’s development or the childbirth process.
The doctor will observe the abdomen, palpate to locate the bottom of the uterus, measure the height of the uterus, check the waist circumference, and evaluate the pelvic structure. They will also feel the abdomen to identify the position of the fetus. The doctor will assess the fetal presentation and listen for the fetal heartbeat. Depending on the gestational age, the specific aspects of the obstetric exam may vary. For example, during the early stages of pregnancy (3-4 months), it is not possible to hear the fetal heartbeat, and measuring the uterus height or waist circumference is unnecessary. At this stage, palpating to locate the bottom of the uterus is sufficient. In the later months, a more thorough examination of the fetal parts is necessary to diagnose the fetal position, presentation, and evaluate the height of the fetal position.


