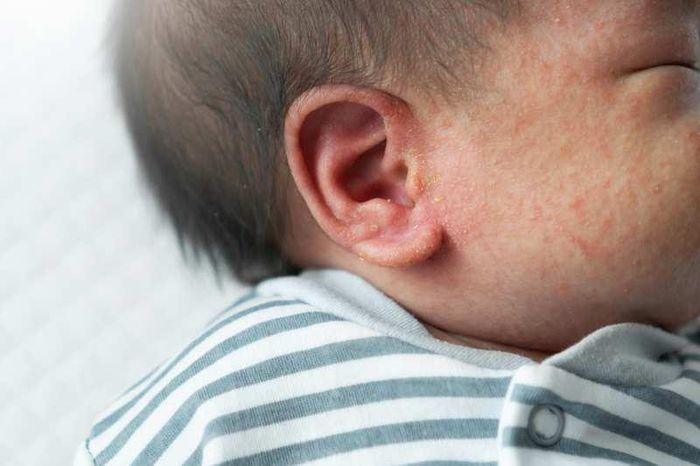
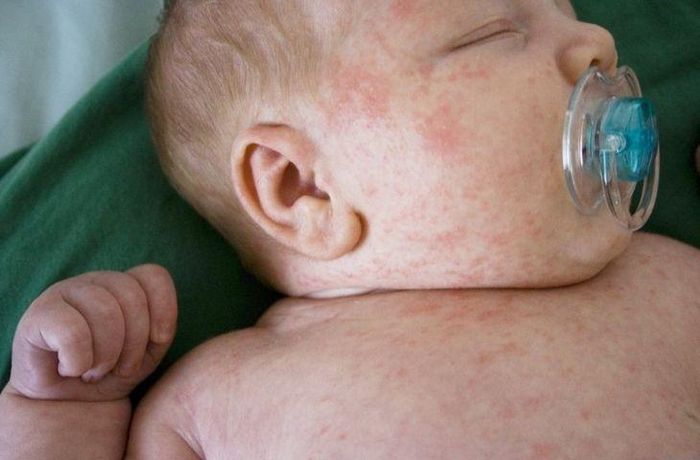
1. How to Recognize Heat Rash in Children
Most common signs to recognize heat rash:
- Small water-filled bumps appear in clusters on red, irritated skin.
- Child experiences itching, crying, restlessness, and discomfort.
- Scratching may cause skin abrasions, infections, and pus-filled pimples or boils.
- Commonly found in areas with abundant sweat glands such as the forehead, neck, shoulders, chest, and back.
Recognizing heat rash is generally easy, but it can be mistaken for other conditions like measles or allergic rashes.
If your child has heat rash, continue daily baths with gentle baby wash, avoid popping or bursting the blisters to prevent spreading infection. Do not use essential oils or apply leaves to the skin, as they can cause further irritation. Trim your child's nails and dress them in breathable clothing. Provide a diet rich in water, minerals, and vitamins from fruits and vegetables. Limit sugary and alcoholic foods.


2. Why Do Children Often Get Heat Rash in Summer?
Summer is a peak time for heat rash due to the following reasons:
- The sweat ducts in children are not fully developed, so sweat can't escape efficiently. In hot weather, the body sweats more to cool down, but this leads to blocked sweat ducts, causing heat rash.
- Sometimes, during summer, children may wear clothing that doesn't absorb sweat well, or they may be in diapers, especially tight ones, leading to sweat duct blockages.
- Summer is also when bacteria proliferate. Some bacteria living on the skin can secrete oils that block sweat ducts.
- If a child has a fever during the hot weather or is overly active, their body will produce more sweat to regulate temperature, which can also result in blocked sweat ducts.


3. Can heat rashes go away on their own?
In essence, heat rashes occur due to excessive heat, so they tend to disappear when the weather becomes cooler. However, "disappearing" does not mean the rashes are completely gone. It simply means that when the temperature drops, the child's skin cools down and stops sweating, causing the symptoms of the rash to subside. These symptoms may reappear in hot conditions, especially in the summer.
Typically, when heat rashes recur frequently, they can develop into deep heat rashes. In simple terms, this refers to the condition that forms after multiple episodes of red heat rashes. At this point, the severity of the condition becomes much worse than before. The damage is no longer just on the surface of the skin but also affects the deeper layers, leading to dark-colored marks. This can also result in a lack of sweat, fatigue, rapid heart rate, continuous vomiting, etc.
In other words, heat rashes cannot resolve on their own unless parents intervene promptly. If the blisters rupture, it can create an opportunity for bacteria and fungi to invade the skin, causing chronic dermatitis, skin infections, and potentially leading to blood poisoning, which could endanger the child's life. Furthermore, prolonged heat rashes can lead to constant itching, crying day and night, refusal to eat, and rapid weakness and weight loss. The ruptured blisters may also leave scars, affecting the child's future appearance.

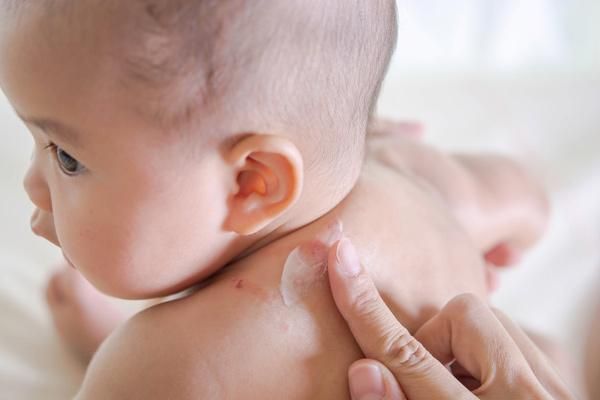
4. Treatment for Heat Rashes
The most effective way to treat heat rashes is to reduce sweating by regulating the temperature: using air conditioning, fans, wearing light clothing, and minimizing physical activity. Once the skin cools down, the heat rashes will quickly disappear.
For mild heat rashes, no treatment is necessary. However, in more severe cases, topical medications may be needed to alleviate discomfort and prevent complications. When a child has heat rashes, parents should prevent them from scratching or rubbing the rashes to avoid breaking the skin, which can allow bacteria to cause infections or lead to more serious complications. Gently rubbing the affected areas can provide some relief for the child. Additionally, it is important to keep the child cool, with breathable clothing, to minimize sweating.
Frequent bathing helps keep the body cool, the skin clean, and the pores open. A diluted solution of potassium permanganate (1:10,000) or a mild, soap-free, unscented bath solution for children can be used. Herbal remedies such as green tea leaves, bitter melon, or guava leaves can also be used to bathe the child at the first sign of rashes.
It is important to note that if these herbs are purchased from the market, they should be soaked in saltwater to remove any remaining chemicals before being boiled for the bath. Avoid squeezing too much lime or rubbing the affected areas of the child's skin, as this can damage the sensitive skin, causing sores and painful irritation.

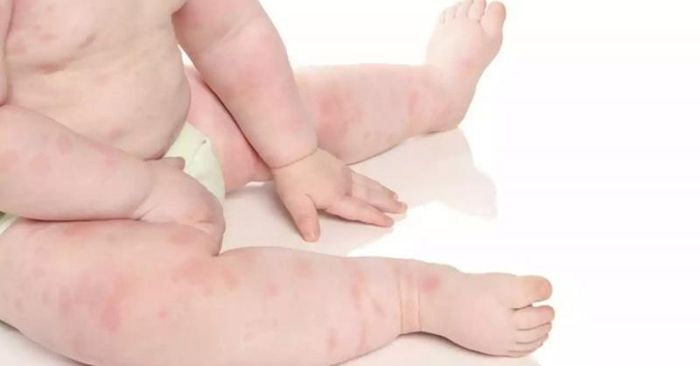
5. When Should You Take Your Child to See a Doctor?
In most cases, heat rashes will resolve on their own within a few days if the rash is mild and proper care and nutrition are provided. If the rash persists for 7 to 10 days or longer, spreads over the body, or shows signs of secondary infection such as swelling, warmth, redness, pain, pus, swollen lymph nodes in the neck, armpits, or groin, fever, or chills, parents should seek medical attention to prevent complications.
Parents should take their child to see a doctor if they experience the following:
- The child is extremely itchy and fussy, affecting their sleep.
- There are multiple pustules on the skin.
- There is pain, swelling, and warmth around the affected area.
- Swollen lymph nodes in the neck, armpits, or groin.
- Fever.
- The heat rashes persist or keep recurring.


6. How Can You Prevent Heat Rashes in Children?
To prevent heat rashes in children, experts recommend the following:
- Dress the child in soft, lightweight, breathable fabrics. Cotton clothing is the best choice.
- Avoid overdressing or making the child too warm.
- When the weather is very hot, keep the child out of direct sunlight. You can use a fan or air conditioning to keep them cool. Ensure the sleeping area is always cool and well-ventilated.
- Bathe the child daily with a gentle, non-irritating soap to remove dirt from the skin’s surface.
- Additionally, keep the child’s skin dry and clean. Avoid using excessive lotions or powders, as these can clog pores and make rashes worse.
- Ensure the child drinks enough water and consume plenty of fresh fruits and drinks rich in vitamin C to boost their immune system and protect against external factors.


7. What is a Heat Rash?
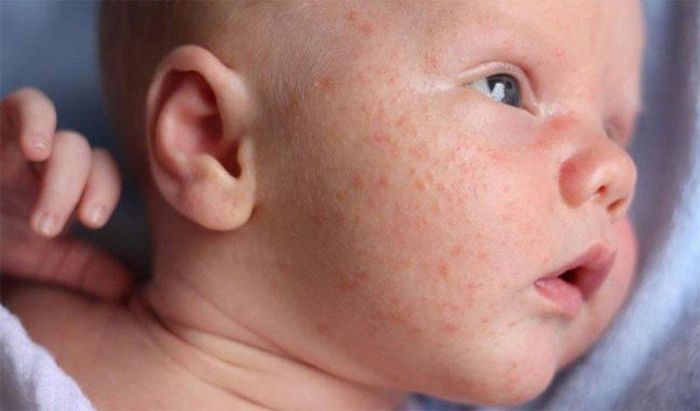
Heat rash occurs when sweat ducts become blocked, leading to the accumulation of sweat. The ducts can become clogged with dust or other impurities, causing inflammation of the skin and the formation of small, pink bumps.
In children, heat rash is common because their sweat ducts are still developing, and the hot summer weather causes them to sweat excessively, which may not be able to escape the skin, leading to sweat buildup and duct blockage.
Most children experience heat rash only when it's hot, and the rash often disappears on its own when the temperature cools down without causing any issues. However, there are many cases where the rash becomes itchy, prompting the child to scratch and potentially leading to skin abrasions, infections, and the development of pustules and boils.
8. What Causes Heat Rashes?
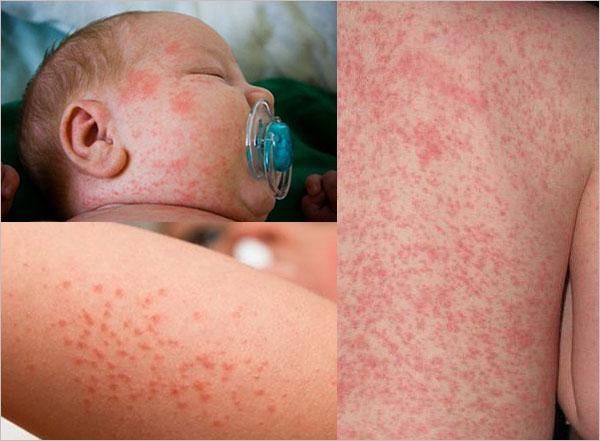
Heat rash occurs when some sweat ducts become blocked. While the exact cause is unclear, several factors play a significant role in this condition, including:
- Underdeveloped sweat ducts in infants, especially during the first week of life, in premature babies, or in those who are placed in incubators; wearing overly warm clothing or being covered with thick blankets; or when the child has a fever.
- Hot and humid weather, especially during the summer, when high temperatures lead to excessive sweating and overstimulation of sweat glands.
- Excessive physical exertion.
- Prolonged time spent lying on the bed.
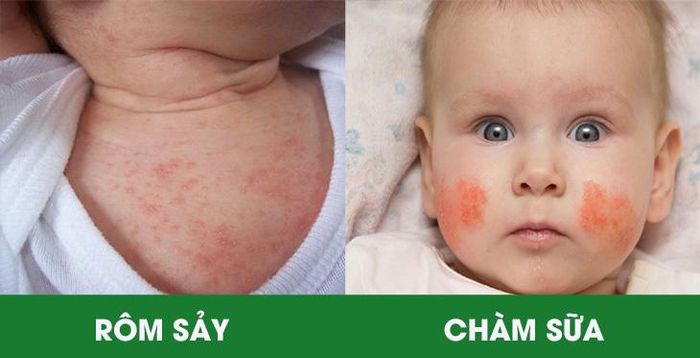
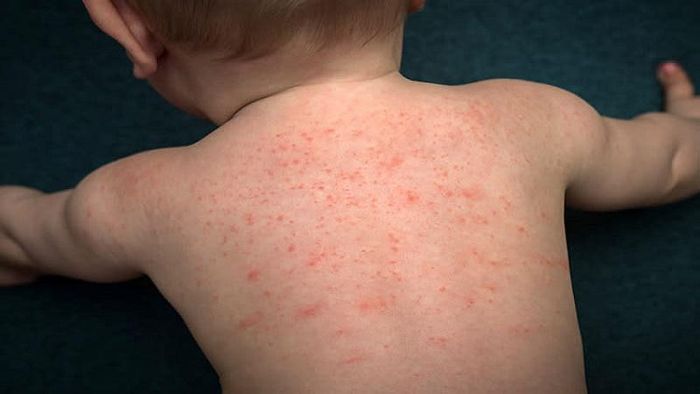
9. Symptoms of Heat Rashes
Hot and oppressive weather causes children to sweat excessively, but since their sweat ducts are not fully developed, the sweat gets trapped inside the skin. Additionally, sweat ducts can become blocked by dust or dirt, leading to small pink bumps on the skin. This typically happens in hot weather, though it may also occur when children are dressed in too many clothes. Children with high fever or those placed in incubators may also experience clogged sweat glands. Physical activity, intense play, wearing clothes made from synthetic fabrics that cause heat retention, or certain bacteria that naturally inhabit the skin can also contribute to sweat duct blockages.
Heat rashes appear as small, red bumps about the size of a pinhead, either in circular or scattered formations. The rash is usually surrounded by redness and may contain small amounts of fluid. The affected areas are commonly found on the head, neck, chest, and back. Where the rash is dense, it becomes red, itchy, and feels hot to the touch. As a result, children with heat rashes often scratch the area, which can lead to skin abrasions and infections.
There are three types of heat rashes in children:
- Crystal rashes: Typically occurs in infants due to underdeveloped sweat ducts. This type of rash is not inflamed and often appears after a high fever, leaving peeling skin once the rash heals.
- Red rashes: Commonly occurs due to hot and humid weather.
- Deep rashes: Occurs when sweat glands are severely damaged, usually after prolonged red rashes.